
The immune system is meant to defend the body against harmful invaders. However, in some cases, it mistakenly attacks healthy organs. In autoimmune thyroid disease, this immune reaction targets the thyroid gland, affecting the hormones that regulate energy, metabolism, and mood. As symptoms often develop gradually, the condition may remain undiagnosed for months.
Autoimmune thyroid diseases (AITDs) are organ-specific autoimmune disorders, mainly Hashimoto's thyroiditis and Graves' disease. According to published research, AITDs affect about 2–5% of the general population. They are more common in women, affecting 5–15% of women and 1–5% of men.
This blog explains what autoimmune thyroid disease is, its types, possible causes and risk factors, diagnosis, and treatment options.
Synopsis
What Is Autoimmune Thyroid Disease?
The thyroid is a butterfly-shaped gland at the base of the neck. It produces the hormones thyroxine (T4) and triiodothyronine (T3), which regulate metabolism, heart rate, body temperature, and energy levels.
In autoimmune thyroid disease, the immune system produces antibodies that attack thyroid tissue. This immune reaction can either slow the thyroid down, causing hypothyroidism, or stimulate it excessively, causing hyperthyroidism.
Types of Autoimmune Thyroid Disorders
The two most common autoimmune thyroid disorders are Hashimoto’s thyroiditis and Graves’ disease.
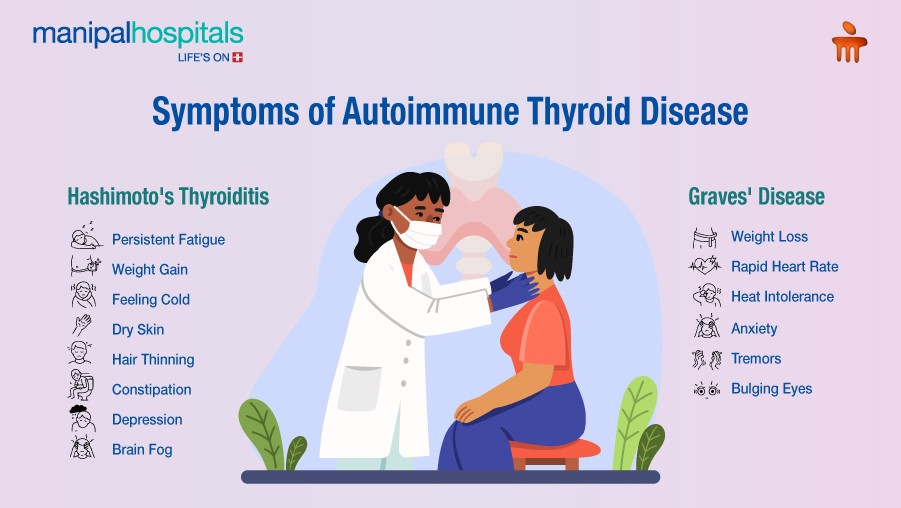
Hashimoto's Thyroiditis: In this condition, immune antibodies gradually damage thyroid cells, leading to hypothyroidism (underactive thyroid). It is the most common cause of hypothyroidism in iodine-sufficient countries.
Common symptoms include:
-
Persistent fatigue
-
Weight gain
-
Feeling cold
-
Hair thinning
-
Depression
-
Brain fog
Graves' Disease: In Graves’ disease, antibodies stimulate the thyroid gland to produce excess hormones, resulting in hyperthyroidism. It is the most common cause of hyperthyroidism.
Symptoms may include:
-
Unintentional weight loss
-
Rapid heart rate
-
Heat intolerance
-
Anxiety or irritability
-
Tremors
In some cases, thyroid eye disease (Graves’ orbitopathy), which may cause eye bulging or irritation
Less common autoimmune thyroid conditions include postpartum thyroiditis, which may occur within a year after childbirth, and painless sporadic thyroiditis.
Causes and Risk Factors for Autoimmune Thyroid Disease
The exact cause of autoimmune thyroid disease is not fully understood. It is thought to result from a combination of genetic susceptibility, hormonal influences, environmental factors, and immune system dysfunction.
Factors associated with a higher risk include:
-
Genetic predisposition: A family history of thyroid or other autoimmune diseases increases the likelihood of developing the condition.
-
Sex hormones: Women are affected much more frequently than men, suggesting a role for hormonal influences.
-
Nutritional factors: Low levels of certain nutrients, such as selenium or vitamin D, may be associated with increased risk.
-
Coexisting autoimmune diseases: People with conditions such as type 1 diabetes, coeliac disease, rheumatoid arthritis, or lupus have a higher likelihood of developing autoimmune thyroid disorders.
How Is Autoimmune Thyroid Disease Diagnosed?
Diagnosis usually involves a combination of blood tests and imaging studies.
-
Thyroid Function Tests (TFTs): Blood tests measure TSH, free T4, and sometimes free T3 to evaluate thyroid hormone levels.
-
Thyroid Antibody Tests
-
Anti-thyroid peroxidase (anti-TPO) antibodies support the diagnosis of Hashimoto’s thyroiditis.
-
TSH receptor antibodies (TRAb) help confirm Graves’ disease.
-
-
Thyroid Ultrasound: Ultrasound imaging may be used to assess the size and structure of the thyroid gland, especially when nodules or structural abnormalities are suspected.
Treatment for Autoimmune Thyroid Disease
Treatment depends on whether the thyroid is underactive or overactive.
-
Hypothyroidism (Hashimoto’s thyroiditis): This condition is usually treated with levothyroxine, a synthetic thyroid hormone that restores normal hormone levels. Regular TSH monitoring helps ensure the dose remains appropriate. This approach forms the basis of autoimmune thyroiditis treatment for patients with Hashimoto’s disease.
-
Hyperthyroidism (Graves’ disease): Medicines that reduce thyroid hormone production are typically the first-line treatment. In some cases, radioactive iodine therapy may be used to gradually reduce overactive thyroid tissue. Thyroidectomy (surgical removal of the thyroid) may be considered when medications or radioiodine therapy are unsuitable or ineffective.
Lifestyle measures such as a balanced diet, regular physical activity, stress management, and adequate sleep may help support overall wellbeing alongside medical treatment.
Conclusion
Autoimmune thyroid disease can affect metabolism, energy levels, and overall well-being. But with timely diagnosis and appropriate treatment, most people can manage the condition effectively. Recognising symptoms early and seeking medical evaluation can help prevent complications and support better long-term health outcomes.
At Manipal Hospitals, the endocrinology team provides comprehensive thyroid evaluation, advanced diagnostic testing, and personalised treatment plans for autoimmune thyroid disease.
FAQ's
Autoimmune thyroid disease itself cannot currently be cured, but the hormonal effects of the condition can usually be managed effectively with treatment.
Autoimmune thyroid disease occurs when the immune system attacks the thyroid gland. Other thyroid disorders may be caused by iodine deficiency, nodules, infections, or certain medications.
Genetics can play a role. People with a family history of thyroid disorders or other autoimmune diseases may have a higher risk of developing autoimmune thyroid disease.
Treatment duration depends on the specific condition. Many people with hypothyroidism require long-term or lifelong hormone replacement therapy, while hyperthyroidism treatments may vary depending on the response to medication or other therapies.
Women are affected much more often than men. Risk also increases with a family history of thyroid disease and the presence of other autoimmune conditions such as type 1 diabetes or coeliac disease. It may also be influenced by certain nutritional or hormonal factors.






















 5 Min Read
5 Min Read















