Many people ignore acid reflux as a small issue, something that comes and goes after a heavy meal. That assumption can be misleading. When the same burning feeling keeps returning or starts affecting sleep and daily comfort, it may no longer be simple reflux. The difference between acid reflux vs GERD lies in how often it happens and what it begins to do to the oesophagus over time. Persistent reflux can quietly cause damage even when symptoms feel manageable. Some people improve with medicines, but others do not.
Knowing when the condition has crossed that line becomes important, especially when surgery enters the discussion. In this article, we discuss all you need to know about GERD and when you need to consider surgery.
Synopsis
Acid Reflux vs GERD
Acid reflux and GERD are related but not the same. Acid reflux occurs when stomach acid flows back into the oesophagus due to the temporary relaxation of the lower esophageal sphincter. It is usually occasional and felt as a burning sensation after eating or lying down.
The difference in acid reflux vs GERD becomes clear when symptoms occur frequently or persist over time. GERD (gastroesophageal reflux disease) is a chronic condition, typically when reflux happens two or more times a week or starts affecting daily life. In such cases, the lower oesophageal sphincter does not function properly.
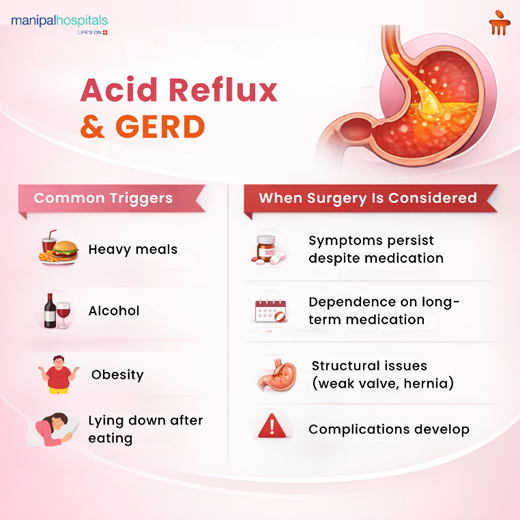
Triggers such as heavy meals, alcohol, obesity, and lying down soon after eating can worsen both conditions. The key difference lies in frequency and impact. Occasional reflux remains mild, while GERD can lead to ongoing symptoms and damage to the lining of the oesophagus over time.
GERD Symptoms
Symptoms do not stay mild once reflux becomes GERD. They start showing up more often and begin affecting day-to-day comfort. Paying attention to these GERD symptoms helps in catching the problem early.
-
Backflow (regurgitation): Food or acidic fluid may come back into the throat after the megaoesophagus. People notice a sour or bitter taste, especially when bending or lying down.
-
Burning in the chest: Acid irritates the lining of the oesophagus. The burning feeling can rise from the upper abdomen into the chest and may worsen at night.
-
Chest discomfort: Not every episode feels like classic heartburn. Some people describe a dull pressure or pain, which can be confusing.
-
Difficulty swallowing: Repeated irritation can make swallowing feel uncomfortable, as if food is getting stuck.
-
Nausea or lingering fullness: A heavy, unsettled feeling may stay even after eating small meals.
-
Throat irritation: Acid reaching higher can lead to hoarseness, a sore throat, or a constant need to clear the throat.
-
Persistent cough: Reflux can trigger a chronic cough even without infection.
GERD Complications
GERD does not stay limited to a burning feeling. The problem is ongoing acid contact with the lining of the oesophagus, which is not built to handle it. With time, that irritation starts to change the tissue.
|
Complication |
Description |
|
Oesophagitis |
Inflammation of the oesophagus causes pain and discomfort |
|
Oesophageal ulcers |
Small sores that may lead to pain or bleeding |
|
Strictures |
Narrowing of the oesophagus due to scar tissue, making swallowing difficult |
|
Barrett’s oesophagus |
Changes in the lining that may increase the risk of cancer |
|
Airway issues |
Acid reaching the throat can cause a cough or irritation |
Managing GERD: Treatment Approaches
Treatment for GERD moves step by step. It starts simple and builds up if symptoms continue.
Lifestyle changes
-
Weight gain can increase intra-abdominal pressure and worsen reflux.
-
Lying down soon after meals allows acid to move upward more easily
-
Staying upright after eating helps reduce symptoms
-
Raising the head end of the bed can improve nighttime reflux
-
Certain foods like oily meals, caffeine, and alcohol can trigger symptoms in some people
Medications
-
Antacids work quickly and neutralise acid, but relief is short-lived.
-
H2 blockers reduce acid production for a few hours.
-
Proton pump inhibitors are stronger and control acid for a longer period, often used when symptoms are frequent.
-
Baclofen may reduce reflux episodes by decreasing transient lower oesophageal sphincter relaxations.
How to Know When GERD Surgery Is Needed
Surgery is usually considered when GERD stops responding to medicines or starts affecting quality of life. While many people improve with treatment, some continue to have symptoms because the problem is structural rather than just acid-related.
Surgery may be needed if:
-
Symptoms continue despite proper medication and keep returning.
-
Long-term dependence on medicines is required for relief.
-
Structural problems such as a weak lower oesophageal sphincter or hiatal hernia are present.
-
Complications develop, including narrowing, ulcers, or cell changes in the oesophagus.
-
Objective findings on tests like endoscopy, pH monitoring, or manometry confirm ongoing reflux.
At this stage, acid control alone may not be enough, and GERD surgery is considered to correct the underlying issue.
Types of Surgery for GERD
Different types of surgery are used to treat GERD, depending on what is causing the reflux and how severe it is.
|
Fundoplication |
The most common procedure is where the upper part of the stomach is wrapped around the lower oesophagus to strengthen the valve and prevent acid reflux. It is usually done laparoscopically. |
|
LINX Device |
A small ring of magnetic beads is placed around the junction of the stomach and esophagus. It helps keep the valve closed while still allowing food to pass during swallowing. |
|
Transoral Incisionless Fundoplication (TIF) |
A minimally invasive procedure done through the mouth using an endoscope. It creates a partial wrap to improve valve function and is suitable for selected cases. |
Who Should Consider GERD Surgery?
GERD surgery is not needed for everyone. It is usually considered when symptoms are persistent or complications begin to develop despite proper treatment.
Surgery may be recommended if:
-
Symptoms continue despite medication, especially long-term use of proton pump inhibitors.
-
Dependence on daily medication for symptom control.
-
Structural issues such as a weak lower oesophageal sphincter or a hiatal hernia.
-
Complications like strictures, ulcers, or Barrett’s oesophagus.
-
Abnormal findings on tests, including endoscopy, pH monitoring, or manometry.
The decision is always based on individual evaluation and should be discussed with a specialist.
Conclusion
To wrap it up, reflux that keeps coming back, starts affecting sleep, or makes swallowing uncomfortable should not be ignored. Early assessment helps identify whether the issue is still manageable with treatment or has moved to a stage where procedures are needed.
If you are dealing with ongoing symptoms, it warrants getting checked. Talk to our specialists at Manipal Hospitals, Whitefield to learn about GERD surgery in Whitefield and whether it’s the best approach for you today.
FAQ's
If it happens once in a while after a heavy meal, that’s reflux. If it keeps coming back every week, disturbs sleep, or needs regular medication, it has likely moved into GERD.
If medicines are not helping, your doctor may suggest a scope test to look inside, a 24-hour acid test, or a muscle test. These help figure out what exactly is going wrong.
Simple changes like eating lighter meals or not lying down early can help in the beginning. But if symptoms keep returning, lifestyle steps alone may not be enough, and treatment needs to go further.
The acid keeps irritating the food pipe. Over time, it can cause wounds, narrowing, or even changes in the lining. You may not feel it daily, but the damage can still build up.
Surgery targets the underlying mechanisms contributing to reflux. Many people get long-term relief, but the decision depends on your reports and how your body is responding to treatment.





















 7 Min Read
7 Min Read