The rhythmic beat of your heart is a testament to its incredible efficiency, constantly working to pump life-giving blood throughout your body. But what happens when that rhythm falters, skips a beat, or races uncontrollably? This is the essence of a heart arrhythmia – a condition where the electrical impulses that coordinate your heartbeats don't function properly, leading to an irregular heartbeat. At Manipal Hospitals, our dedicated team, including our highly experienced cardiologists in Gurugram, are at the forefront of diagnosing and treating these complex conditions, helping patients regain their heart's natural rhythm and quality of life.
An arrhythmia can range from a harmless, occasional flutter to a serious medical emergency, potentially affecting your heart's ability to pump blood effectively. Understanding the various types, recognising heart arrhythmia symptoms, identifying the underlying causes, and exploring modern treatment options is crucial for anyone experiencing an irregular heartbeat.
Synopsis
What is an Arrhythmia?
An arrhythmia refers to any disorder of the heart rate or heart rhythm. It means that your heart is beating too fast, too slow, or with an irregular pattern. A normal adult heart typically beats 60 to 100 times per minute at rest. When the heart's electrical system, which generates impulses that tell your heart muscle when to contract, goes awry, it can disrupt this normal rhythm.
The heart has four chambers: two upper chambers (atria) and two lower chambers (ventricles). The sinoatrial (SA) node, often called the heart's natural pacemaker, is located in the right atrium and initiates the electrical impulse for each heartbeat. This impulse then travels through the atria, causing them to contract, and then through the atrioventricular (AV) node to the ventricles, prompting their contraction. Any interference in this intricate pathway can lead to heart arrhythmia disease.
Globally, millions are affected by arrhythmias. For instance, atrial fibrillation, a common type of arrhythmia, affects over 33 million people worldwide, highlighting the widespread impact of these conditions. Early detection and intervention are key to managing these conditions effectively.
Types of Arrhythmias
Arrhythmias are broadly classified based on the heart rate they cause (tachycardia or bradycardia) and where they originate in the heart (atrial or ventricular). Here are some of the most common types:
-
Bradycardia: This refers to a heart rate that is too slow, typically fewer than 60 beats per minute. It can be caused by problems with the SA node, certain medications, or underlying heart conditions. While some athletes naturally have a slow heart rate, persistent bradycardia can lead to fatigue, dizziness, and fainting.
-
Tachycardia: This is a heart rate that is too fast, usually more than 100 beats per minute. Tachycardias can originate in the atria (supraventricular tachycardias) or the ventricles (ventricular tachycardias).
-
Atrial Fibrillation (AFib): The most common type of serious arrhythmia, AFib involves chaotic electrical signals in the atria, causing them to quiver rather than contract efficiently. This leads to an irregular and often rapid ventricular response. AFib significantly increases the risk of stroke.
-
Atrial Flutter: Similar to AFib but with more organised, rapid electrical activity in the atria, leading to a faster but often regular atrial rate.
-
Supraventricular Tachycardia (SVT): A broad term for fast heart rates originating above the ventricles. This includes conditions like Atrioventricular Nodal Reentrant Tachycardia (AVNRT) and Wolff-Parkinson-White (WPW) syndrome.
-
Ventricular Tachycardia (VT): A rapid heart rate originating in the ventricles. This can be very serious, as it can compromise the heart's ability to pump blood and may degenerate into ventricular fibrillation.
-
Ventricular Fibrillation (VFib): A life-threatening arrhythmia where the ventricles quiver uselessly instead of pumping blood, leading to sudden cardiac arrest. Immediate medical intervention is critical.
-
-
Premature Beats: These are extra, early heartbeats that originate in the atria (premature atrial contractions - PACs) or ventricles (premature ventricular contractions - PVCs). They are often harmless but can sometimes indicate an underlying heart condition or be bothersome.
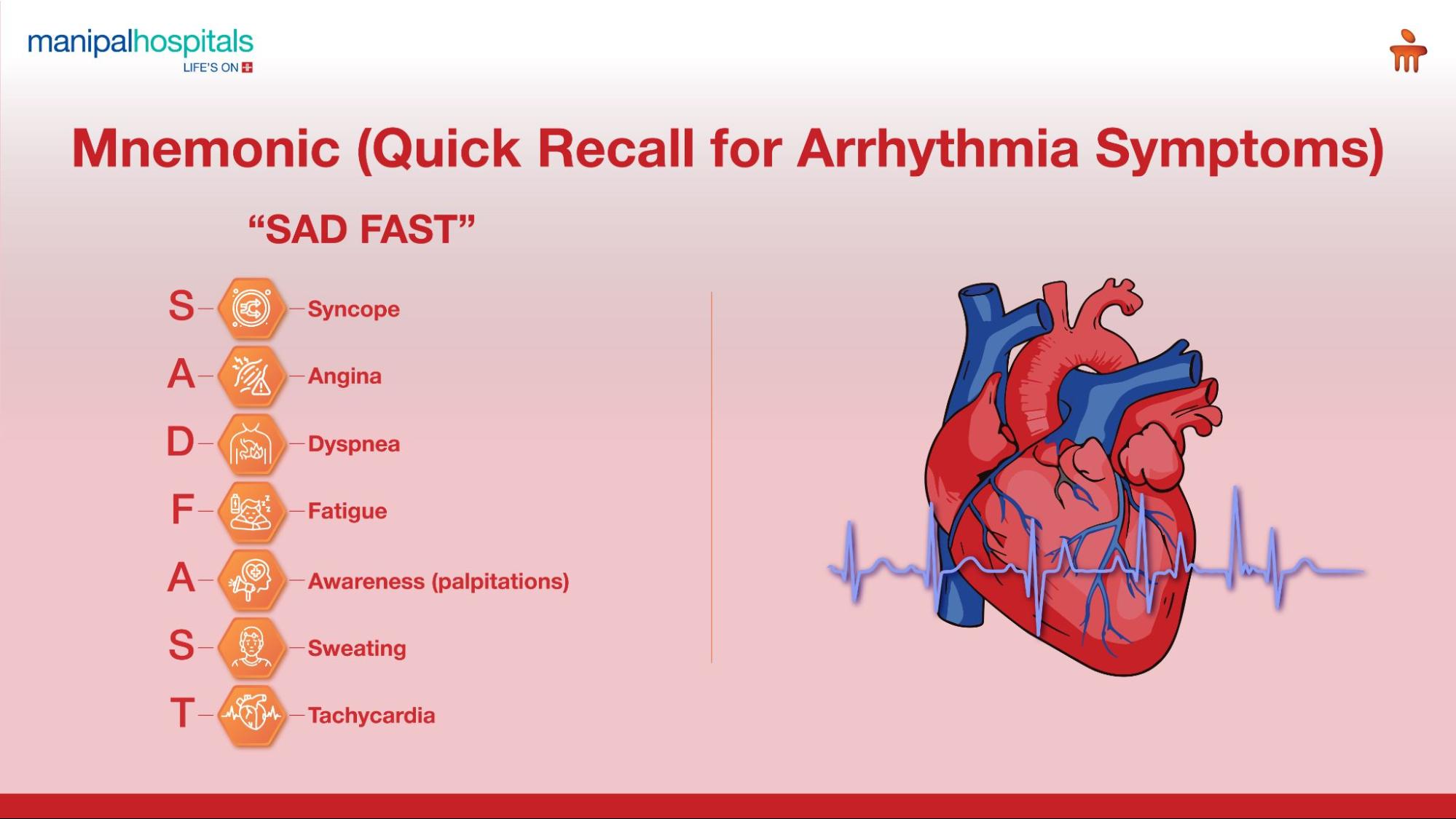
Understanding Heart Arrhythmia Symptoms
The heart arrhythmia symptoms can vary widely, from barely noticeable to severe and debilitating. Some individuals may experience no symptoms at all, with an arrhythmia only discovered during a routine check-up. However, it's crucial to be aware of the common signs of an irregular heartbeat:
-
Palpitations: A feeling of a racing, pounding, fluttering, or skipping heart. This is often described as feeling your heart beating in your chest or throat.
-
Dizziness or Light-headedness: A reduced blood flow to the brain due to inefficient pumping can cause these sensations.
-
Fainting (Syncope): In severe cases, a significant reduction in blood flow to the brain can lead to a temporary loss of consciousness.
-
Shortness of Breath: The heart's inability to pump enough blood efficiently can lead to fluid build-up in the lungs, causing breathlessness, especially during exertion.
-
Chest Discomfort or Pain: While not always present, some arrhythmias can cause angina-like symptoms due to increased oxygen demand or decreased blood flow.
-
Fatigue: Persistent tiredness, even with adequate rest, can be a symptom as the heart works harder to compensate for its irregular rhythm.
-
Anxiety: The unsettling feeling of an irregular heartbeat can sometimes trigger anxiety.
If you experience any of these heart arrhythmia symptoms, especially if they are severe, frequent, or occur suddenly, seeking immediate medical attention is vital. Early diagnosis can prevent more serious complications.
Causes and Risk Factors of Irregular Heartbeat
Understanding what cardiac arrhythmia disease is often involves looking into its roots. An irregular heartbeat can stem from a variety of factors, ranging from underlying heart conditions to lifestyle choices. Common causes and risk factors include:
-
Coronary Artery Disease: Blocked arteries can reduce blood supply to the heart muscle, potentially damaging the electrical system.
-
High Blood Pressure (Hypertension): Over time, high blood pressure can stiffen and thicken the heart muscle, leading to electrical problems.
-
Heart Attack: Scar tissue from a previous heart attack can interfere with electrical signal conduction.
-
Heart Failure: A weakened heart that cannot pump blood effectively is more prone to arrhythmias.
-
Cardiomyopathy: Diseases of the heart muscle that cause it to become stretched, thickened, or stiffened.
-
Diabetes: Uncontrolled blood sugar levels can damage nerves and blood vessels, impacting heart function.
-
Thyroid Gland Disorders: Both an overactive (hyperthyroidism) and an underactive (hypothyroidism) thyroid gland can affect heart rate and rhythm.
-
Electrolyte Imbalances: Abnormal levels of potassium, sodium, calcium, and magnesium in the blood can disrupt electrical impulses.
-
Certain Medications: Some prescription and over-the-counter drugs, including decongestants and certain asthma medications, can trigger arrhythmias.
-
Excessive Alcohol or Caffeine Consumption: These stimulants can directly affect heart rhythm.
-
Stress and Anxiety: High levels of stress can release hormones that temporarily alter heart rate.
-
Smoking: Nicotine can increase heart rate and blood pressure, contributing to arrhythmias.
-
Sleep Apnoea: Interrupted breathing during sleep can put stress on the heart, leading to arrhythmias.
Studies indicate that addressing modifiable risk factors like high blood pressure, diabetes, and obesity can reduce the incidence of certain arrhythmias by up to 40%. Our team, including our cardiologists in Gurugram, focuses on comprehensive patient education to manage these risk factors effectively.
Diagnosis of Arrhythmias
Diagnosing heart arrhythmia disease typically begins with a thorough medical history and physical examination. Your doctor will ask about your symptoms, lifestyle, and any underlying health conditions. Diagnostic tests may include:
-
Electrocardiogram (ECG/EKG): Records the electrical activity of your heart, showing if it's beating too fast, too slow, or irregularly.
-
Holter Monitor: A portable ECG device worn for 24 to 48 hours, or sometimes longer, to record heart activity during daily routines.
-
Event Monitor: A portable device that you activate when you feel symptoms, recording heart activity for longer periods (weeks or months).
-
Implantable Loop Recorder: A small device implanted under the skin to continuously monitor heart rhythm for up to three years.
-
Echocardiogram: Uses sound waves to create images of your heart's structure and function.
-
Cardiac CT Scan or MRI: Provides detailed images of the heart and surrounding structures.
-
Electrophysiology (EP) Study: A more invasive procedure where thin, flexible wires are guided to your heart to map its electrical activity and pinpoint the source of the arrhythmia.
Treatment Options for Heart Arrhythmia Disease
The treatment for heart arrhythmia disease depends on the type, severity, and underlying cause of the arrhythmia. The goal is to restore a normal heart rhythm, control heart rate, prevent blood clots (if applicable), and manage symptoms. Options include:
-
Lifestyle Modifications: For mild arrhythmias, changes such as reducing caffeine and alcohol intake, quitting smoking, managing stress, and maintaining a healthy weight can be effective.
-
Medications:
-
Antiarrhythmic Drugs: Help restore or maintain a normal heart rhythm.
-
Beta-blockers and Calcium Channel Blockers: Slow down the heart rate.
-
Blood Thinners (Anticoagulants): Prescribed for certain arrhythmias like AFib to reduce the risk of stroke by preventing blood clot formation.
-
-
Cardioversion: A procedure that uses controlled electrical shocks (external cardioversion) or medications (chemical cardioversion) to reset the heart's rhythm. This procedure boasts high immediate success rates, often over 80-90% for restoring sinus rhythm.
-
Catheter Ablation: A minimally invasive procedure where thin, flexible catheters are guided to the heart to identify and destroy (ablate) the small areas of heart tissue responsible for the irregular electrical signals. This procedure has significantly advanced, with success rates for paroxysmal atrial fibrillation reaching 70-80% after one procedure, and even higher with repeat procedures.
-
Implantable Devices:
-
Pacemakers: Small devices implanted under the skin, with wires leading to the heart, to send electrical impulses to regulate a slow heart rate (bradycardia).
-
Implantable Cardioverter-Defibrillators (ICDs): Devices implanted similarly to pacemakers, designed to detect dangerously fast heart rhythms (like VT or VFib) and deliver an electrical shock to restore normal rhythm.
-
-
Surgery: In some cases, such as complex structural heart disease, surgical procedures like the Maze procedure may be performed to create scar tissue that blocks abnormal electrical pathways.
Our expert team, including our cardiologists in Gurugram, provides personalised treatment plans, combining advanced medical therapies with cutting-edge procedural interventions to ensure the best possible outcomes for our patients.
If you are experiencing these symptoms, it's crucial to seek timely medical advice. Book an appointment with our expert cardiologists at Manipal Hospitals today.
FAQ's
Not always. Many people experience occasional harmless irregular heartbeats (like premature beats). However, some arrhythmias can be serious and require medical attention. It's best to consult a doctor if you notice persistent or concerning symptoms.
Yes, stress and anxiety can contribute to or worsen arrhythmias in some individuals. They can trigger the release of hormones that affect heart rate and rhythm. Managing stress is often part of an arrhythmia management plan.
An ECG is a snapshot of your heart's electrical activity at a single moment. A Holter monitor is a portable device worn for 24-48 hours (or longer) that continuously records your heart's activity during your daily routine, helping to detect intermittent arrhythmias.
Some arrhythmias can be effectively cured, particularly with procedures like catheter ablation. For others, the condition can be very well managed with medications, lifestyle changes, or implanted devices, allowing patients to live full and active lives.
Untreated arrhythmias can lead to serious complications such as stroke (especially with AFib), heart failure, and even sudden cardiac arrest. Prompt diagnosis and treatment are essential to prevent these adverse outcomes.





















 7 Min Read
7 Min Read