
Have you been ignoring persistent back pain as “just a strain”? Do you notice tingling down your leg or a sharp pain when bending? For many people, these can be early slipped disc symptoms in the lower back. The condition often begins gradually before it starts affecting everyday activities.
A slipped disc is also known as a herniated or ruptured disc. This occurs when the soft, gel-like centre of a spinal disc pushes through a tear in its outer ring and irritates or compresses nearby nerves. Although it sounds serious, most people recover with conservative treatment and time. In this blog, we explain what a slipped disc is, why it happens, the signs you shouldn’t ignore, and how treatment and recovery work.
Synopsis
What is a Slipped Disc?
The spine is a flexible structure designed to move, bend, and support your body. The bones, called vertebrae, sit one on top of another, with cushion-like discs between them that act as shock absorbers, helping you move comfortably.
Each disc has two parts:
-
A soft, gel-like centre (nucleus pulposus)
-
A tough outer ring (annulus fibrosus)
Disc Bulge vs Disc Herniation: With age or strain, the outer ring can weaken or develop small tears.
Disc Bulge: The disc extends outward beyond its normal boundary, but the outer ring remains intact. A bulge may not cause symptoms unless it presses on a nearby nerve.
Disc Herniation (Slipped Disc): A tear develops in the outer ring, allowing part of the inner gel-like material to push outward. This can irritate or compress adjacent nerves and is more likely to cause pain, tingling, numbness, or muscle weakness.
A slipped disc can occur anywhere along the spine, but most commonly affects the lower back (lumbar spine) and, less often, the neck (cervical spine).
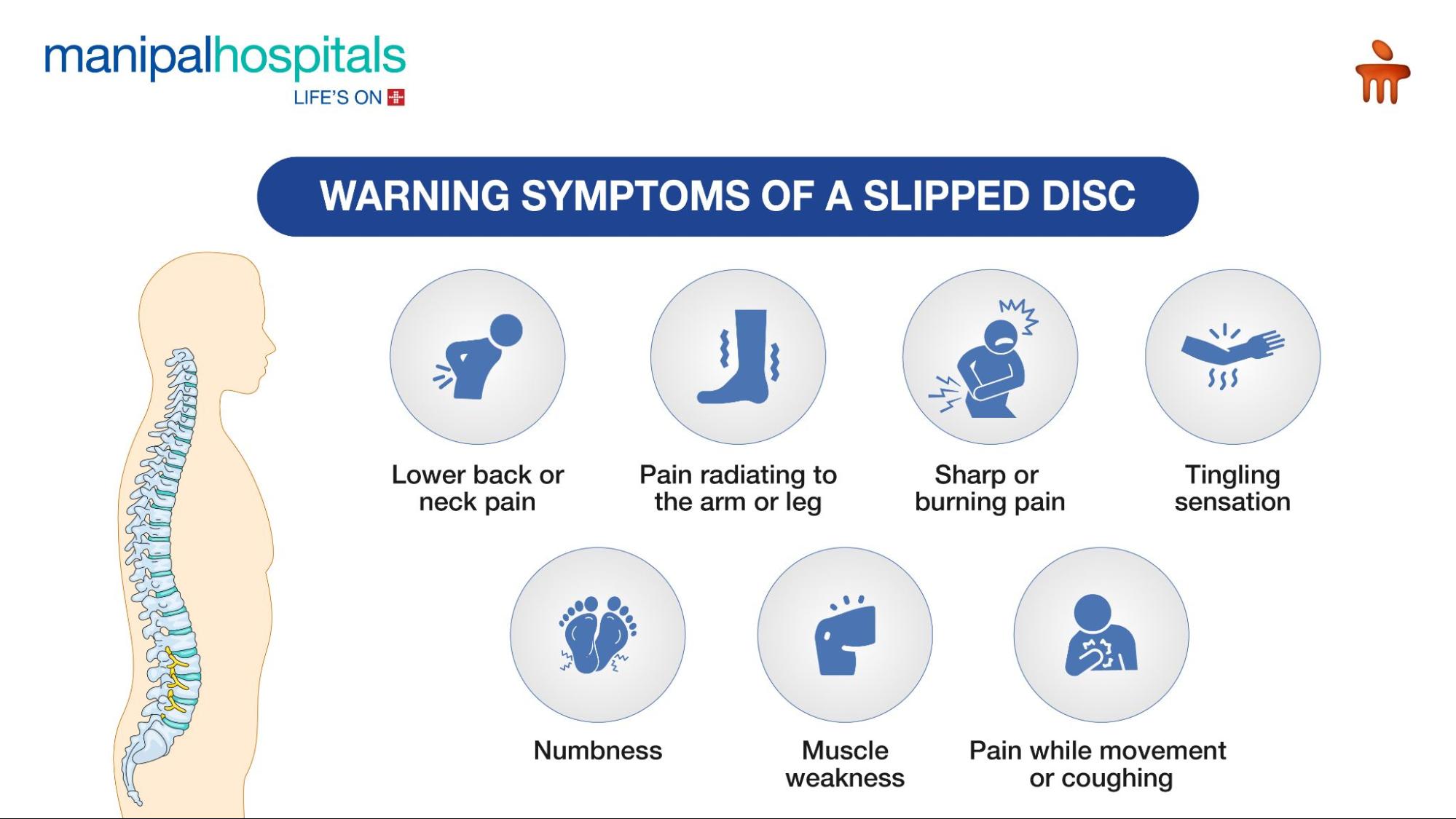
Common Symptoms You Shouldn’t Ignore
Not everyone with a slipped disc feels pain. Some cases are discovered incidentally during scans for other reasons. When symptoms do occur, they usually affect one side of the body and follow the path of an irritated nerve.
If the lower back is affected:
-
Pain in the lower back, buttocks, thigh, or calf
-
Pain that may extend into the foot (sciatica)
-
Sharp, burning, or shooting pain that worsens with coughing or sneezing
-
Numbness or tingling in the leg
-
Muscle weakness, difficulty walking, or reduced reflexes
If the neck is affected:
-
Pain in the shoulder and arm
-
Tingling or numbness in the hand or fingers
-
Weak grip strength
Disc-related pain often radiates along a nerve and changes with posture or movement.
Why Does It Happen?
Spinal discs gradually lose water content and elasticity with age, a process called disc degeneration. As they become less flexible and more brittle, they are more likely to bulge or develop small tears in the outer layer (annulus fibrosus). Increased spinal pressure can then cause the inner gel-like material (nucleus pulposus) to protrude outward.
Common slipped disc causes and risk factors include:
-
Age-related wear and tear
-
Falls or sudden injuries
-
Repeated bending, twisting or heavy physical work
-
Poor lifting technique
-
Prolonged sitting, obesity, or smoking
A slipped disc is often the result of gradual strain rather than a single event.
How Is a Slipped Disc Diagnosed?
Doctors diagnose a slipped disc through symptom history and physical examination, assessing movement, strength, reflexes, and sensation.
Imaging is not always required immediately. MRI or CT scans may be recommended if symptoms are severe or persistent. MRI is the most useful test for visualising discs and nerves. X-rays help rule out fractures or alignment problems. In rare cases where infection is suspected, blood tests may be needed.
Slipped Disc Treatment: What Are the Options?
Most slipped discs improve within 4-8 weeks without surgery. Treatment focuses on pain relief and supporting healing.
Common slipped disc treatment approaches include:
-
Pain relief medicines, including medication for nerve-related pain
-
Physiotherapy and guided rehabilitation
-
Gentle manual therapy when appropriate
-
Heat or cold packs for symptom relief
-
Staying active and avoiding prolonged bed rest
Targeted exercises are an important part of recovery. They strengthen the muscles that support the spine, improve posture, and reduce strain on the affected area. Many people improve as inflammation settles and the body gradually adapts to the disc injury.
Surgery, such as a discectomy or laminectomy, is considered only in selected cases, including when:
-
Nerve weakness worsens
-
Pain remains severe despite treatment
-
There is a loss of bladder or bowel control (medical emergency)
If an infection is present, antibiotic treatment will be required.
Conclusion
A slipped disc may seem mild at first, but ignoring early warning signs can allow nerve symptoms to worsen. Slipped disc symptoms in the lower back often start subtly, so early awareness and timely medical care are important.
If you notice persistent back pain, tingling, numbness, or weakness in your arm or leg, seek medical care promptly. Early diagnosis and treatment support recovery and protect long-term spinal health. Manipal Hospitals provides expert spine care and personalised treatment plans to help patients return to daily activities comfortably.
FAQ's
Many people improve within 4–6 weeks with medication, gentle activity, and physiotherapy. If pain continues or weakness worsens, further evaluation may be needed. A small number of cases require injections or surgery.
Slipped disc exercises are guided movements designed to strengthen the core and back muscles, improve flexibility, and support spinal stability. When performed correctly under professional supervision, they can reduce pain and support recovery.
No. Most people recover without surgery. It is usually considered only for severe nerve compression, worsening weakness, or symptoms that do not improve with conservative treatment.
Yes. Maintaining a healthy weight, strengthening core muscles, practising good posture, and staying active help reduce strain on the spine. Avoiding smoking and unsafe lifting techniques also lowers the risk of recurrence.
Seek urgent medical attention if you develop loss of bladder or bowel control, numbness around the groin, rapidly worsening leg weakness, or difficulty walking. These may signal severe nerve compression and require immediate treatment.






















 6 Min Read
6 Min Read
















