Back pain is a common ailment, but understanding its root cause is crucial for effective treatment. Often, terms like spondylosis and spondylitis are used interchangeably, leading to confusion. While both affect the spine and cause discomfort, they are distinct conditions with different origins, prognoses, and management strategies. At Manipal Hospitals, we believe in empowering our patients with clear, accurate information to navigate their spine health journey.
This comprehensive guide from our expert orthopaedic in Ghaziabad aims to demystify these conditions, helping you understand the nuances between them. Recognising the specific diagnosis is the first step towards personalised and effective spine care.
Synopsis
- Spondylosis: The Degenerative Wear and Tear
- Causes and Risk Factors
- Common Spondylosis Symptoms
- Diagnosis and Treatment for Spondylosis
- Spondylitis: The Inflammatory Condition
- Causes and Risk Factors
- Common Spondylitis Symptoms
- Diagnosis and Treatment for Spondylitis
- Spondylosis vs Spondylitis: Key Distinctions
- Conclusion
Spondylosis: The Degenerative Wear and Tear
Spondylosis refers to the general degeneration of the spine due to age-related wear and tear. It's not a single disease but rather a term encompassing various degenerative changes in the spinal discs and joints. This condition is incredibly common; studies show that over 85% of people over the age of 60 show signs of spondylosis on X-rays, though many remain asymptomatic. It can affect any part of the spine, leading to conditions like cervical spondylosis (neck), thoracic spondylosis (mid-back), or lumbar spondylosis (lower back).
Causes and Risk Factors
-
Ageing: The natural process of discs drying out and shrinking, and bones developing spurs.
-
Genetics: A family history may increase susceptibility.
-
Occupational Stress: Jobs involving repetitive movements, heavy lifting, or prolonged sitting.
-
Injuries: Previous spinal injuries can accelerate degeneration.
-
Obesity: Excess weight puts additional strain on the spine.
Common Spondylosis Symptoms
Symptoms often develop gradually and can range from mild to severe, frequently worsening with activity and improving with rest.
-
Chronic Back Pain or Neck Pain: Often described as a dull ache.
-
Stiffness: Especially in the morning or after periods of inactivity.
-
Reduced Flexibility: Difficulty in bending or twisting the spine.
-
Numbness or Tingling: If nerve compression occurs, radiating into the arms or legs.
-
Muscle Weakness: In affected limbs, in severe cases.
Diagnosis and Treatment for Spondylosis
Diagnosis typically involves a physical examination, review of medical history, and imaging tests such as X-rays, MRI, or CT scans. Treatment for spondylosis is largely conservative, focusing on pain management and improving function. At Manipal Hospitals, our integrated approach often includes:
-
Physical Therapy: Strengthening exercises and stretching to improve flexibility and support.
-
Pain Management: Medications, including NSAIDs, muscle relaxants, or nerve pain medications.
-
Lifestyle Modifications: Weight management, ergonomic adjustments, and regular low-impact exercise.
-
Injections: Epidural steroid injections for localised pain relief.
-
Surgery: Rarely needed, but may be considered for severe spinal cord compression or intractable pain. Approximately 90% of patients with cervical or lumbar spondylosis experience significant relief with non-surgical treatments within 6-12 weeks under expert care.
Spondylitis: The Inflammatory Condition
In contrast to spondylosis, spondylitis is an inflammatory condition that primarily affects the spine and sometimes other joints. It is an autoimmune disease, meaning the body's immune system mistakenly attacks its own tissues. The most common form is Ankylosing Spondylitis (AS), which often starts in the sacroiliac joints (where the spine meets the pelvis) and can progress to fuse vertebrae, leading to a rigid spine. It often manifests in younger adults, typically before the age of 45.
Causes and Risk Factors
The exact cause of spondylitis is unknown, but genetics play a significant role.
-
Genetics: The presence of the HLA-B27 gene is a strong risk factor, though not everyone with the gene develops the condition.
-
Age: Onset typically occurs in late adolescence or early adulthood.
-
Gender: Historically, AS was thought to be more common in men, but it affects women nearly as often, though often with milder symptoms.
Common Spondylitis Symptoms
Inflammatory back pain is the hallmark of spondylitis and has distinct characteristics:
-
Chronic Back Pain: Often insidious in onset, lasting more than 3 months, worse in the morning or after inactivity, and improves with exercise.
-
Morning Stiffness: Can last for more than 30 minutes.
-
Fatigue: A common and often debilitating symptom.
-
Pain in Other Joints: Hips, shoulders, heels, or ribs can also be affected.
-
Sacroiliac Joint Pain: Deep pain in the buttocks or lower back.
-
Enthesitis: Inflammation where tendons or ligaments attach to bone (e.g., Achilles tendonitis, plantar fasciitis).
Diagnosis and Treatment for Spondylitis
Diagnosing spondylitis can be challenging, especially in its early stages. It involves a thorough clinical assessment, blood tests (to check for inflammatory markers and HLA-B27 gene), and imaging (X-rays, MRI of the sacroiliac joints). Early diagnosis is critical for better outcomes, with studies indicating that early intervention within 3 months of symptom onset can significantly improve long-term prognosis and reduce disease progression in up to 70% of patients.
Treatment focuses on reducing inflammation, managing pain, preventing spinal fusion, and maintaining mobility.
-
Medications: NSAIDs are often the first line. Disease-modifying antirheumatic drugs (DMARDs) and biologics are used for more severe or progressive cases to control the immune response.
-
Physical Therapy: Tailored exercises to improve posture, maintain flexibility, and strengthen core muscles are vital.
-
Lifestyle Adjustments: Regular exercise, smoking cessation, and maintaining a healthy weight.
-
Surgery: Rarely needed, mainly for severe deformities or hip joint replacement.
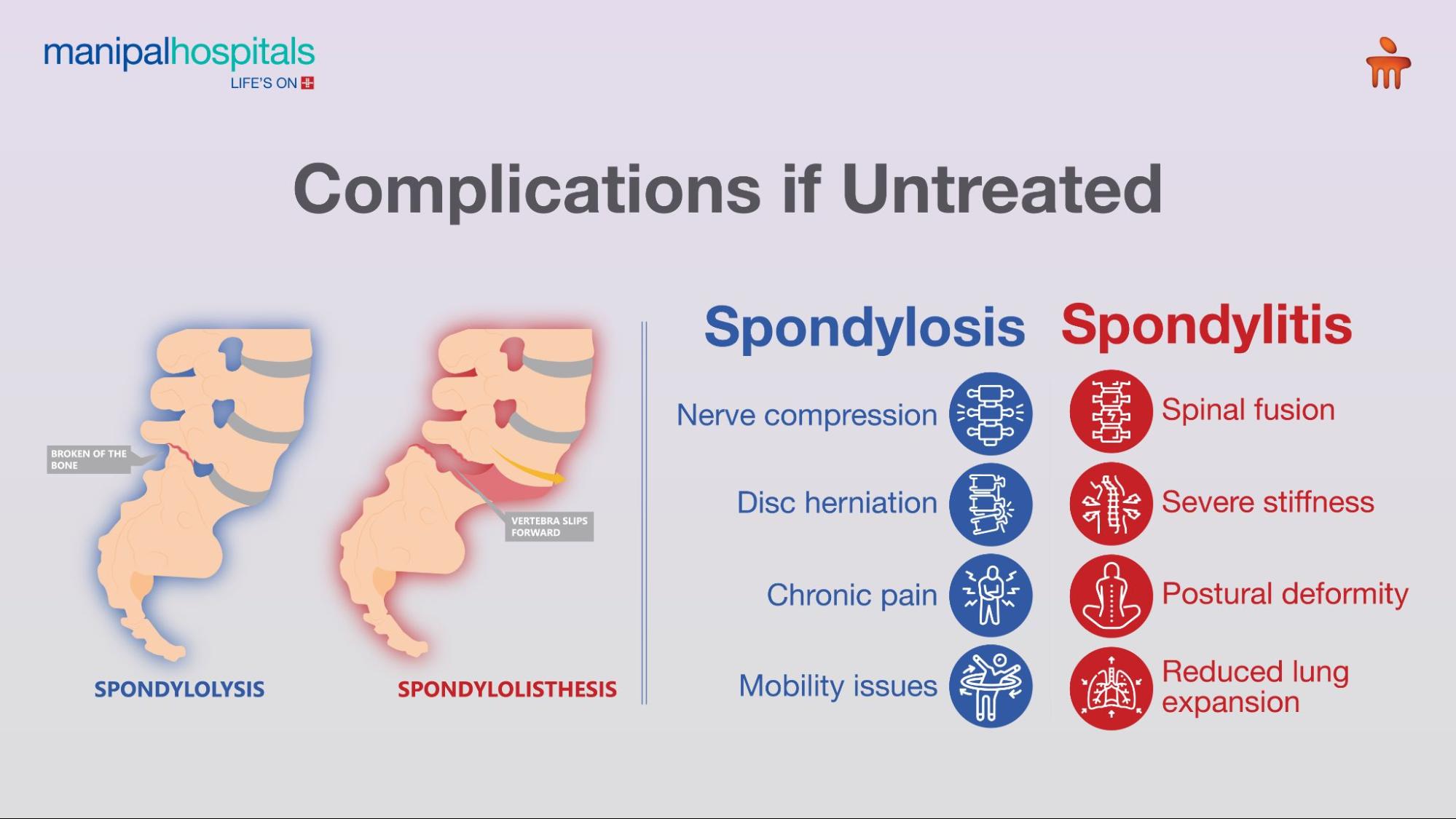
Spondylosis vs Spondylitis: Key Distinctions
Understanding the fundamental differences is key to accurate diagnosis and effective joint pain relief.
-
Nature: Spondylosis is degenerative ("wear and tear"); spondylitis is inflammatory (autoimmune).
-
Cause: Spondylosis is primarily age-related; spondylitis is genetic/autoimmune.
-
Onset: Spondylosis usually develops gradually later in life; spondylitis often starts in young adulthood.
-
Pain Characteristics: Spondylosis pain often improves with rest and worsens with activity. Spondylitis pain typically worsens with rest (especially in the morning) and improves with activity.
-
Systemic Symptoms: Spondylitis can cause fatigue, fever, and inflammation in other organs; spondylosis is generally localised to the spine.
-
Progression: Spondylosis involves bone spurs and disc degeneration. Spondylitis can lead to spinal fusion and rigidity.
Conclusion
If you are experiencing persistent back or neck pain, it's crucial to seek timely medical advice. Book an appointment with our expert orthopaedics in Ghaziabad today for an accurate diagnosis and personalised treatment plan.
FAQ's
No, spondylosis is a degenerative condition, while spondylitis is an inflammatory autoimmune condition. They have different underlying causes, and one cannot "turn into" the other. However, it's possible to have both concurrently.
Yes, regular physical activity is crucial for both, but the type and intensity of exercise may differ. For spondylosis, it helps strengthen supporting muscles. For spondylitis, it's essential to maintain spinal mobility and prevent fusion. Always consult your doctor or physical therapist for a personalised exercise plan.
Genetics play a stronger role in spondylitis, particularly the HLA-B27 gene, which significantly increases the risk of developing ankylosing spondylitis. While family history can be a minor risk factor for spondylosis, it's primarily age-related degeneration.
Absolutely. Maintaining a healthy weight, practising good posture, regular exercise, and avoiding smoking are beneficial for managing symptoms and slowing the progression of both conditions. Diet may also play a supportive role, especially in inflammatory conditions.
You should consult a doctor if your back pain is persistent (lasting more than a few weeks), severe, worsens at night or with rest, is accompanied by numbness or weakness in limbs, or if you experience unexplained weight loss or fever. Early diagnosis and treatment can significantly improve outcomes for both spondylosis and spondylitis.





















 6 Min Read
6 Min Read