Knee pain is a pervasive health concern that can diminish an individual's quality of life, restricting mobility and affecting daily activities from simple walking to athletic pursuits. This discomfort happens when the cartilage and surrounding soft tissues in the knee joint are affected. Understanding what causes knee tissue damage is essential getting the proper treatment to ensure that one can move toward a pain-free life.
Synopsis
What is Knee Tissue Damage?
The knee which is the largest joint in the human body, comprises of bones, ligaments, tendons, and cartilage to facilitate movement and bear significant weight. A reason why pain in this joint happens is knee cartilage damage, specifically the articular cartilage found behind of the kneecap. This cartilage allows the bones to glide effortlessly against each other. It also acts as a shock absorber, distributing forces across the joint during movement. When this tissue is injured, it can lead to chronic pain, swelling, and stiffness.
However, knee tissue damage can also occur when the ligaments, and tendons are impaired. These include
-
Menisci: Found between the thigh bone and shin bone, these c-shaped cartilages help improve joint stability and enable shock absorption. Meniscal tears are very common injuries, often leading to pain, swelling, and mechanical symptoms like clicking or locking.
-
Ligaments: These are strong, fibrous bands that connect bones to other bones. The major knee ligaments include:
-
Anterior Cruciate Ligament (ACL): Prevents the shin bone from sliding forward excessively relative to the femur.
-
Posterior Cruciate Ligament (PCL): Prevents the shin bone from sliding backward excessively.
Damage to any of these, particularly common in sports, can result in instability and significant pain.
-
Tendons: Connect muscles to bones, allowing movement. Key tendons around the knee include the quadriceps tendon (connecting the thigh muscles to the kneecap) and the patellar tendon (connecting the kneecap to the shinbone). Tendinitis or tears in these tendons can also cause knee pain and functional limitation.
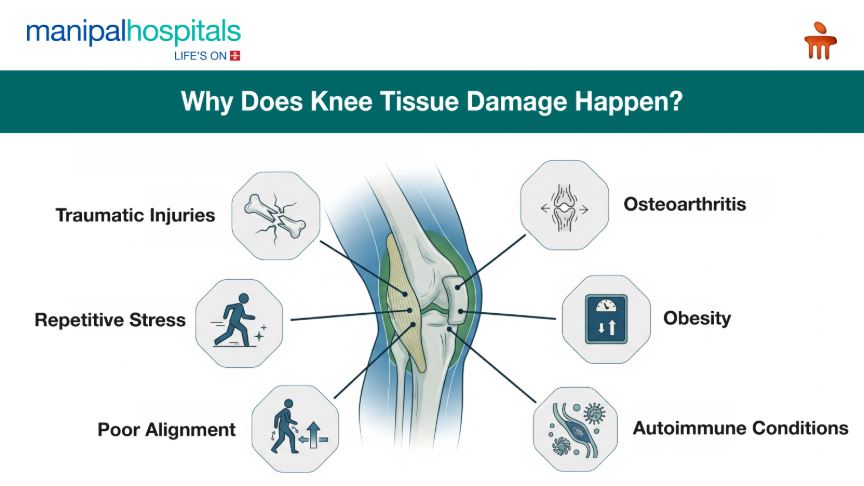
Why Does Knee Tissue Damage Happen?
Several factors can cause knee tissue to degenerate or injure:
-
Traumatic Injuries: Rapid twisting motion, a direct blow to the knee, or a hard fall can cause acute knee cartilage injury, meniscal tears, or ligamentous ruptures. Such injuries usually happen with high-impact sports or during accidents.
-
Degenerative Changes (Osteoarthritis): This is a leading cause of chronic knee pain in older adults. In this condition there is cumulative wear and tear (over decades on the knee joint which causes the articular cartilage to progressively erode.
-
Repetitive Stress: Chronic, low-level trauma, can accumulate over time leading to significant knee tissue damage. Activities requiring repeated bending, prolonged kneeling, squatting, or heavy lifting (common in certain occupations like construction, landscaping, or nursing) can place excessive, Fcumulative strain on the knee joint.
-
Obesity: Excess body weight increases load on the knee joints. This constant, amplified pressure exacerbates knee cartilage damage and increases the risk of meniscal tears.
-
Poor Biomechanics and Alignment: In conditions where there are gait and posture abnormalities, misalignments in the knee, the hip, or the ankle can disrupt the weight distribution on the knee joint, worsening tissue damage.
-
Inflammatory Conditions: Autoimmune diseases, such as rheumatoid arthritis, psoriatic arthritis, or lupus, can trigger chronic inflammation within the joint lining (synovium). This inflammation affects the articular cartilage and surrounding tissues, resulting in severe knee tissue damage.
Knee Tissue Damage Symptoms
Recognizing knee cartilage damage symptoms helps with early intervention to improve treatment outcomes:
-
Pain: It can manifest as a dull, persistent ache that worsens with activity, a sharp, stabbing pain during specific movements, or a deep, throbbing sensation at rest.
-
Swelling: When there is inflammation of the knee joint, fluid tends to accumulate causing it to appear visibly enlarged or feel tender to the touch.
-
Stiffness: The joint usually feels tight when attempting to bend or straighten the knee. Often occurs in the morning or after prolonged inactivity.
-
Clicking, Popping, or Grinding Sensations (Crepitus): These audible or palpable sounds and sensations happen when damaged cartilage surfaces rub against each other, or as torn meniscal fragments move within the joint during movement.
-
Reduced Range of Motion: The inability to fully extend (straighten) or flex (bend) the knee compared to the uninjured leg which can severely impair activities like squatting, kneeling, or even walking.
-
Weakness or Instability: Feeling that the knee might give way or buckle, especially during weight-bearing activities, ascending/descending stairs, or pivoting.
Diagnosing Knee Tissue Damage
Diagnosis usually begins with a thorough discussion of your symptoms, medical history, activity levels, and any specific incidents that may have led to the injury. After which the specialist will conduct a physical examination to assessing your knee's range of motion and stability and identify areas of tenderness and swelling.
Imaging Tests:
-
X-rays: Help to rule out fractures and bony abnormalities
-
Magnetic Resonance Imaging (MRI): Provides highly detailed images of cartilage, ligaments (ACL, PCL, MCL, LCL), menisci, tendons, and surrounding muscles to reveal the location, type, and extent of knee cartilage damage.
-
Ultrasound: Evaluates superficial soft tissues like tendons (e.g., patellar tendinitis) and for detecting fluid collections within the joint.
-
Arthroscopy: A minimally invasive surgical procedure where a small camera (arthroscope) is inserted into the joint through tiny incisions. This procedure is only performed when the non-invasive methods don’t give a conclusive answer. It directly visualises the extent of the damage to cartilage, menisci, and ligaments in real-time.
Effective Management: Knee Tissue Damage Treatment Options
Knee tissue damage treatment is broadly classified into two types:
1. Conservative Management
For many patients with less severe damage or acute injuries, non-surgical approaches are highly effective. These include:
-
Rest and Activity Modification: Temporarily reducing, eliminating or finding alternate activities that aggravate the knee.
-
Physical Therapy: Physiotherapists may help create a personalised program which focusses on strengthening muscles surrounding the knee and enhancing joint stability. They also include gentle stretches, mobilisation techniques, exercises to improve balance and correcting walking patterns.
-
Pain Management: Pain-relieving medications, anti-inflammatory drugs, corticosteroid injections, or hyaluronic injections can help with reducing pain.
-
Bracing: Knee braces can provide external support and stability, especially for ligament injuries.
-
Lifestyle Modifications: Weight management, proper footwear, and ergonomic adjustments can reduce stress on the knee.
2. Surgical Intervention
For severe knee tissue damage, more extensive surgical interventions may be necessary:
-
Partial Knee Replacement: A partial replacement involves resurfacing only the affected section with metal and plastic components, whilst preserving the healthy parts of the knee.
-
Total Knee Replacement (Total Knee Arthroplasty): For widespread, severe tissue damage affecting multiple compartments of the knee, replacing the entire damaged joint surfaces with prosthetic metal and plastic components can provide excellent pain relief, restore motion, and significantly improve quality of life.
-
Osteotomy: In cases of malalignment (e.g., bow-leggedness), an osteotomy involves surgically cutting and realigning a bone (usually the shin or thigh bones).
Knee Injury Recovery Time
Knee injury recovery time vary significantly based on factors like the type and severity of knee tissue damage, the chosen treatment modality, the individual's overall health, age, and their adherence to rehabilitation protocols. While conservative treatments might show improvement within weeks to a few months, surgical procedures typically necessitate a longer structured recovery period, ranging from several months to over a year for full recuperation.
Proactive Strategies for Optimal Knee Health and Prevention
While injuries can sometimes be unavoidable, many forms of knee tissue damage can be prevented through proactive measures such as:
-
Maintain a healthy body weight
-
Engage in regular, low-impact exercises
-
Practice proper form and technique when exercising
-
Wear supportive footwear
-
Incorporate warm-up and cool-down routines
-
Listen to your body and rest when needed
-
Stay hydrated and nourished
-
Pay attention to your posture and positioning during prolonged sitting, standing, or repetitive tasks
Seek early medical advice if you experience new or worsening knee pain, stiffness, or instability.
Conclusion
Persistent knee discomfort that limits your movement, feels unstable, or remains swollen may indicate underlying knee tissue damage. A clinical evaluation is essential to accurately diagnose knee tissue injury and establish a recovery plan. The experts at the Department of Orthopaedics at Manipal Hospital, Goa can help determine the extent of the damage and provide the necessary treatment to restore your mobility.
FAQ's
Articular cartilage injury has a very limited capacity to heal spontaneously due to its avascular nature (lack of direct blood supply) and absence of nerve endings. However, various treatments, both surgical and non-surgical, can stimulate the growth of new cartilage-like tissue, repair the damaged area, or mitigate symptoms to improve function.
Generally, low-impact exercises are recommended to minimise stress on the joint. These include activities like cycling (stationary or outdoor), swimming (especially aqua jogging or water aerobics), elliptical training, and walking on soft surfaces. Strengthening exercises for the quadriceps, hamstrings, glutes, and calf muscles are also help to support the knee joint. Please consult with a specialist who can design a personalised exercise program tailored to your specific condition and recovery stage.
Key strategies include maintaining a healthy body weight to reduce joint load, engaging in regular low-impact exercises to strengthen supporting muscles, always warming up before physical activity and cooling down afterward, wearing appropriate and supportive footwear, practicing proper form and technique during sports or heavy lifting, and listening to your body to avoid overexertion.
Many cases of knee tissue damage, especially those detected early or resulting from mild to moderate injuries, can be effectively managed with conservative treatments such as physical therapy, rest, activity modification, pain management, and bracing. Surgical options are typically considered for more severe or extensive damage, when conservative methods have failed to provide adequate relief.
Ignoring knee tissue damage symptoms can lead to several significant risks and complications. These include progressive worsening of the damage (e.g., small cartilage defects enlarging, meniscal tears extending), increased pain, chronic inflammation, joint instability, and progression to more severe conditions like advanced osteoarthritis. Delaying treatment can cause functional impairment which may require more extensive interventions.





















 6 Min Read
6 Min Read