Living with chronic digestive issues can be challenging and often confusing. Two common conditions that frequently get mistaken for one another are Irritable Bowel Syndrome (IBS) and Inflammatory Bowel Disease (IBD). While both affect the gastrointestinal (GI) tract and share overlapping symptoms, they are fundamentally different in their pathology, diagnosis, and long-term implications. Understanding these differences is crucial for effective management and improving the patient’s quality of life. At Manipal Hospitals, our gastroenterologists in Delhi are dedicated to providing accurate diagnosis and personalised treatment plans for both IBS and IBD, helping the patient navigate their path to better gut health.
Synopsis
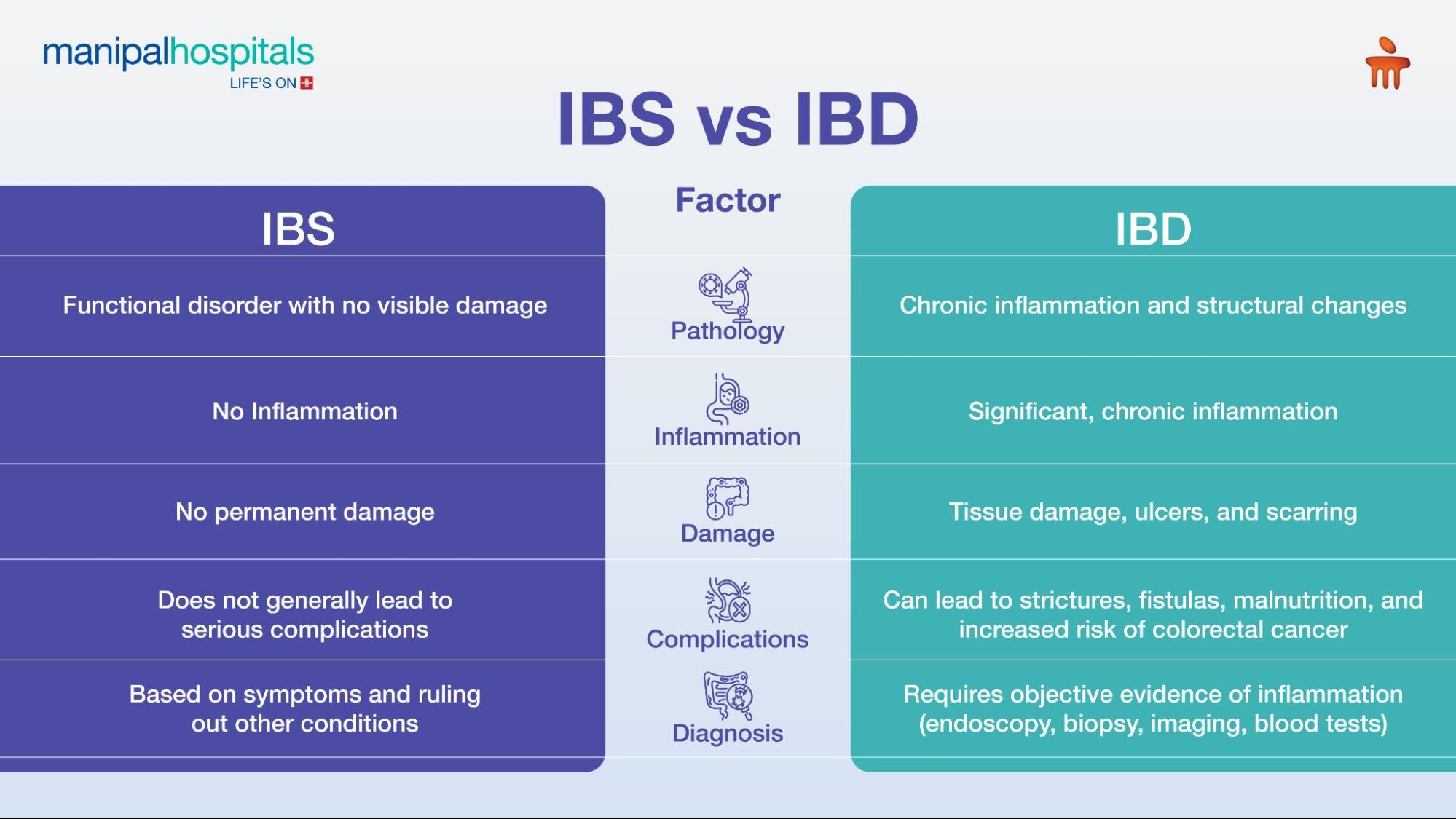
Understanding the Difference: IBS vs. IBD
The primary distinction between Irritable Bowel Syndrome and Inflammatory Bowel Disease lies in the illness. IBS is classified as a functional gastrointestinal disorder, meaning there's a problem with the gut's motility, but there is no visible damage or inflammation. IBD, on the other hand, is a group of chronic inflammatory conditions that cause structural changes and damage to the digestive tract.
Irritable Bowel Syndrome (IBS): Often referred to as a "gut-brain axis disorder," IBS predominantly affects the large intestine. It's characterised by a group of symptoms that may occur together, including abdominal pain, bloating, gas, and changes in bowel habits (diarrhoea, constipation, or both). The exact cause is unknown, but factors like diet, stress, gut microbiota, and nerve sensitivity in the bowel are believed to play a role. Importantly, IBS is a motility disorder and does not lead to permanent damage to the intestine or increase the risk of more serious diseases. It is noteworthy that IBS can coexist with other
Inflammatory Bowel Disease (IBD): This is a more severe, chronic inflammatory condition of the GI tract. The two main types of IBD are Crohn's disease and Ulcerative Colitis. In IBD, the body's immune system mistakenly attacks healthy cells in the digestive system, leading to chronic inflammation, tissue damage, and potentially life-threatening complications. IBD can significantly impact a patient's health and requires ongoing medical management. Ulcerative Colitis affects the large intestine, whereas Crohn’s disease can affect any part of the GI Tract, predominantly the large and small intestine.
Irritable Bowel Syndrome (IBS): A Deeper Look
IBS is incredibly common, affecting an estimated 15-30% of the global population, with many more remaining undiagnosed. While it doesn't cause physical damage, its symptoms can be debilitating and significantly impact daily life.
Symptoms of IBS (IBS symptoms)
- Recurrent abdominal pain, often relieved by a bowel movement.
-
Changes in bowel frequency or consistency.
-
Bloating and gas.
-
Mucus in the stool.
-
Feeling of incomplete evacuation.
IBS Treatment Options
Management of IBS is focused on symptom relief and improving quality of life. Many patients find significant relief through a multifaceted approach. Studies show that up to 70% of IBS patients experience improved symptoms with targeted dietary and lifestyle modifications.
-
Dietary Modifications: Identifying trigger foods (e.g., high-FODMAP foods, certain dairy products, gluten) and adjusting diet can be highly effective. A registered dietitian can provide personalised guidance.
-
Stress Management: Techniques like mindfulness, meditation, yoga, and regular exercise can significantly reduce IBS symptoms, as stress is a major trigger. CBT also has a good role to play in the care.
-
Lifestyle Changes: Regular sleep, adequate hydration, and avoiding smoking and excessive alcohol.
-
Pharmacological Support: Depending on predominant symptoms (diarrhoea or constipation), specific medications can help manage symptoms under medical supervision.
Inflammatory Bowel Disease (IBD): The Chronic Inflammation
IBD is a chronic condition that involves inflammation of the digestive tract. It's characterised by periods of remission and flare-ups. Early diagnosis and consistent management are critical to prevent complications. With modern therapies, a significant percentage of patients with IBD can achieve long-term remission and maintain a good quality of life.
Types of IBD
-
Crohn's Disease: Can affect any part of the GI tract from the mouth to the anus, though it most commonly affects the small intestine and the beginning of the large intestine. Inflammation can penetrate deep into the bowel wall.
-
Ulcerative Colitis: This type of IBD specifically affects the large intestine (colon and rectum). The inflammation is typically continuous and affects the innermost lining of the colon.
The IBD can be classified as mild/moderate/severe depending on the extent of the disease.
Symptoms of IBD (inflammatory bowel disease)
While some symptoms overlap with IBS, IBD symptoms are generally more severe and can include:
-
Persistent diarrhoea, often with blood or mucus.
-
Severe abdominal pain and cramping.
-
Weight loss and fatigue.
-
Fever.
-
Anaemia due to blood loss.
-
Malnutrition due to poor absorption of nutrients.
-
Extra-intestinal manifestations like joint pain, skin rashes, or eye inflammation.
Treatment for IBD
IBD treatment aims to reduce inflammation, relieve symptoms, correct nutritional deficiencies, and prevent complications. A personalised approach, often involving a multidisciplinary team including our expert gastroenterologists in Delhi, is essential.
-
Anti-inflammatory Therapies: Medications designed to reduce inflammation in the GI tract are central to IBD management.
-
Immunomodulators: These therapies work by suppressing the immune system to reduce inflammation.
-
Biologic Therapies: Advanced treatments that target specific proteins involved in the inflammatory process.
-
Dietary Management: While diet doesn't cause IBD, specific dietary changes can help manage symptoms during flare-ups and ensure adequate nutrition.
-
Surgical Intervention: In some cases, surgery may be necessary to remove damaged parts of the intestine or manage complications.
conclusion
If you are experiencing persistent digestive symptoms or are concerned about your gut health, it's crucial to seek timely medical advice. Book an appointment with our expert gastroenterologists at Manipal Hospitals today.
FAQ's
No, IBS is a functional disorder and does not progress into IBD. They are distinct conditions. However, it is possible to have both IBS and IBD concurrently, which can complicate diagnosis and management.
IBD is diagnosed through a combination of physical examination, blood tests, stool tests, imaging studies (like MRI or CT scans), and endoscopic procedures (colonoscopy or endoscopy with biopsy) to visualise and sample the inflamed tissue.
Yes, but they differ. For IBS, a low-FODMAP diet is often recommended to identify triggers. For IBD, dietary management focuses on reducing inflammation during flares, ensuring nutrient absorption, and avoiding foods that irritate the gut, which can be highly individualised.
With proper management, individuals with IBS can lead full and active lives. While it's a chronic condition, symptoms can be effectively controlled through diet, lifestyle, and medical therapies.
You should consult a doctor if you experience persistent abdominal pain, changes in bowel habits lasting several weeks, unexplained weight loss, fever, blood in your stool, or severe fatigue. Early consultation is key to accurate diagnosis and effective management.





















 6 Min Read
6 Min Read