A child who bruises easily, falls ill repeatedly, or seems unusually tired often leaves parents searching for answers. In many cases, these signs are linked to routine childhood illnesses or minor nutritional issues. Occasionally, however, they may point to something deeper happening inside the body, particularly within the bone marrow, the soft tissue responsible for producing blood cells. When the marrow stops producing enough healthy cells, the body gradually loses its ability to carry oxygen, fight infections, and prevent bleeding. Bone marrow failure in children can begin quietly, with symptoms that are easy to overlook. But if it goes unnoticed for too long, it can become a serious health concern.
By recognising bone marrow failure symptoms and understanding the available treatments, parents and caregivers can seek timely medical support and ensure children receive the specialised care they need. This blog walks you through the causes, warning signs, diagnosis, and modern treatment approaches for bone marrow failure in kids, helping families navigate a condition that demands both vigilance and hope.
Synopsis
Bone Marrow Failure in Kids
Bone marrow is responsible for producing three essential types of blood cells, namely, red blood cells, which transport oxygen; white blood cells, which fight off infections; and platelets, which prevent blood loss. When all of this is functioning well, the body will be in a healthy state of balance with regard to blood cell production.
Problems arise when the marrow loses its ability to generate enough of them. Doctors refer to this condition as bone marrow failure, a group of disorders where the production line slows down or shuts down entirely. As cell counts fall, the body begins to struggle with everyday functions.
Unlike short-term illnesses, these changes tend to persist and gradually worsen without medical intervention, which is why early recognition becomes so important.
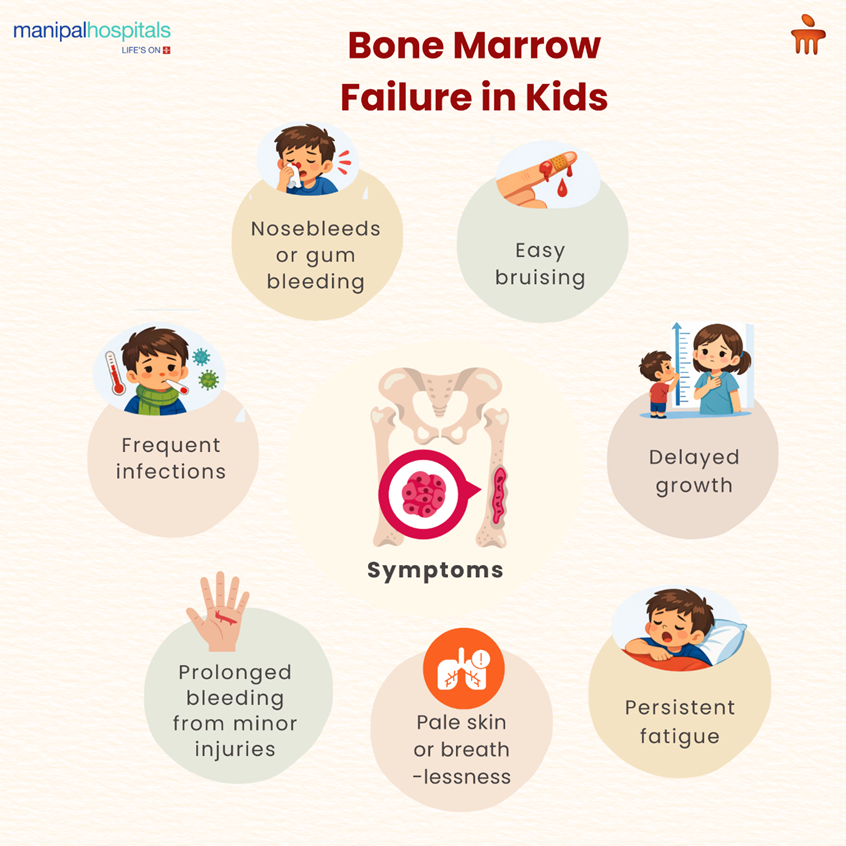
Early Warning Signs Parents Should Notice
Children do not always articulate how they feel, which makes observation especially important. The body often sends subtle signals long before laboratory tests confirm a diagnosis.
Some of the symptoms may take time to show up, while some may show up suddenly as a result of low blood cell production.
Common symptoms of bone marrow failure include:
-
Frequent or severe infections, which take longer than usual to heal
-
Easily bruising or having unexplained marks on the skin
-
Bleeding, such as from the nose or gums, with no obvious cause
-
Fatigue or low energy levels
-
Shortness of breath or pale skin, such as when performing routine activities
-
Delayed growth or development
Medical professionals may also detect some symptoms when performing routine checkups on the patient. A blood test, also known as a complete blood count (CBC), may show abnormal blood cell production, or cytopenias, as a result of bone marrow failure, indicating low blood cell counts.
In some children, certain physical traits may raise suspicion of an inherited syndrome related to bone marrow failure. These may include short stature, unusual skin pigmentation, nail abnormalities, limb differences, or developmental delays. Such findings help doctors determine whether the condition has a genetic basis.
Conditions Linked to Inherited Bone Marrow Failure
While some cases develop later due to environmental or immune factors, several children are born with genetic conditions that affect how bone marrow functions. These conditions fall under the category of inherited bone marrow failure syndrome, and each has distinct characteristics.
Several syndromes have been identified through decades of medical research. Key inherited disorders include:
-
Fanconi Anaemia: One of the most recognised inherited causes, often associated with café-au-lait skin spots, short stature, and abnormalities of the thumb or forearm bones.
-
Diamond–Blackfan Anaemia: A rare disorder usually identified in infancy, characterised by a severe reduction in red blood cell production.
-
Shwachman–Diamond Syndrome: A condition affecting both bone marrow and the pancreas, frequently accompanied by skeletal abnormalities and low white cell counts.
-
Dyskeratosis Congenita: Known for a distinctive combination of skin pigmentation changes, nail dystrophy, and white patches inside the mouth.
-
Thrombocytopenia-Absent Radius Syndrome: A rare condition in which children have low platelet counts alongside the absence of the radius bone in the forearm.
Each of these disorders affects the marrow differently, but all share a common feature: the inability to maintain healthy blood cell production over time.
How Do Doctors Confirm Bone Marrow Failure?
Because many childhood illnesses can cause temporary drops in blood counts, diagnosis requires careful evaluation. Specialists typically follow a structured approach to confirm whether a child truly has bone marrow failure in kids.
Testing usually begins with blood investigations and gradually moves to more specialised assessments.
Diagnostic steps often include:
-
Complete Blood Count with differential to measure levels of red cells, white cells, and platelets
-
Reticulocyte count, which shows how actively the bone marrow is producing new red cells
-
Peripheral blood smear to examine the shape and appearance of blood cells
-
Bone marrow aspirate and biopsy to assess whether the marrow is underactive or hypocellular
-
Genetic testing to identify inherited conditions affecting blood production
-
Chromosomal breakage studies when Fanconi anaemia is suspected
-
Flow cytometry tests in specific cases to evaluate related blood disorders
These investigations help doctors determine not only whether bone marrow failure exists but also its underlying cause, which directly influences treatment decisions.
Treatment for Bone Marrow Failure in Kids
Managing this condition involves both stabilising the child’s health and addressing the root cause of marrow failure. The treatment strategy often evolves depending on disease severity and the child’s response to therapy.
Supportive care forms the first line of management, helping control symptoms and prevent complications.
Supportive treatments may include:
-
Blood transfusions to manage severe anaemia
-
Platelet transfusions to reduce bleeding risk
-
Antibiotics for bacterial infections
-
Growth factors that stimulate blood cell production in selected cases
While these measures help control symptoms, they do not permanently restore marrow function.
For many children, the most effective long-term solution is haematopoietic stem cell transplantation, commonly known as bone marrow transplantation. This procedure replaces the damaged marrow with healthy stem cells from a compatible donor, allowing the body to rebuild its blood-forming system.
Living with the Condition: What Families Should Expect
A diagnosis of bone marrow failure in kids changes the rhythm of family life. Frequent hospital visits, blood tests, and treatments may become part of the routine for some time. Yet many children continue attending school, socialising, and participating in activities with appropriate medical guidance.
Emotional support is equally important. Parents often benefit from counselling, patient support groups, and close collaboration with paediatric haematology teams. Understanding the condition empowers families to manage day-to-day challenges while focusing on long-term recovery.
Medical progress over the past two decades has dramatically improved survival and quality of life for children affected by bone marrow failure, offering hope that once-serious conditions can now be treated effectively.
Conclusion
Recognising early signs such as unexplained bruising, repeated infections, or persistent fatigue can make a meaningful difference in the outcome of bone marrow failure in kids. Early evaluation allows doctors to identify the cause, monitor complications, and begin treatment before severe complications develop. Although bone marrow failure can arise from genetic conditions or acquired causes, modern medicine offers several effective treatment strategies, from supportive therapies to curative stem cell transplantation. With proper care and lifelong monitoring, many children go on to lead healthy and active lives. Families seeking specialised care or treatment for bone marrow failure in kids in Whitefield should consult experienced paediatric haematology teams at Manipal Hospitals.
FAQ's
Yes, it can in many cases. When the bone marrow is unable to produce enough white blood cells, the body’s natural defense system becomes weaker. As a result, the child may become more vulnerable to infections. However, many children also regain their immune function post-transplant or successful treatment.
Not necessarily. While certain conditions fall under inherited bone marrow failure, other cases develop later due to immune disorders, viral infections, medications, or environmental toxins. Doctors determine the cause through genetic testing, medical history, and laboratory studies.
Nutritional anaemia usually occurs due to deficiencies such as low iron or vitamin B12 and typically improves with dietary correction or supplements. In contrast, anemia due to bone marrow failure results from the marrow’s inability to produce red blood cells. Treatment, therefore, focuses on addressing the underlying marrow disorder rather than simply correcting nutrient levels.
In many situations, they can, provided their doctors consider it medically safe. Some precautions may be necessary, particularly when white blood cell counts are low. Schools may need to be informed about infection precautions, fatigue management, and emergency contact protocols.
Several factors influence this decision, including the severity of blood cell deficiency, genetic diagnosis, risk of complications, availability of a compatible donor, and how well the child responds to supportive treatments. Specialists carefully evaluate these elements before recommending transplantation as the best long-term option.





















 8 Min Read
8 Min Read