.png)
Most people do not really take active interest in their kidney health until something feels off. One morning your shoes fit a little tighter, or you tire more easily going up a few flights of stairs. Those small changes can be the earliest hints that kidney function is slowing. When this happens gradually over months or years, the condition is called chronic kidney disease (CKD). This long-term condition often develops slowly, sometimes over many years. In its early phases, many people may not notice any clear symptoms, which is why awareness and routine health checks play an important role.
In this blog, a top nephrologist and kidney transplant surgeon in Yeshwanthpur helps you understand the CKD stages, symptoms, causes, and chronic kidney disease treatment options for chronic kidney disease, enabling early recognition and timely medical intervention. Early diagnosis and appropriate management can slow disease progression and improve quality of life.
Synopsis
What Is Chronic Kidney Disease (CKD)?
To understand what is chronic kidney disease, picture the kidneys as a pair of sieves, filtering waste and excess fluid from your blood. Each kidney is made up of millions of tiny filters called nephrons. When those filters become damaged, they accumulate waste and affect many body systems.
In chronic kidney disease (CKD), these filtering units become damaged over time. Healthy kidneys filter about 120–150 quarts of blood daily, producing around 1–2 quarts of urine. With the progression of CKD, the kidneys start losing their filtering capacity, which results in the accumulation of toxins and fluids. These conditions can adversely affect multiple organ systems. CKD is known as chronic because kidney damage persists for three months or longer.
Understanding CKD Stages
Clinicians describe progression using CKD stages, which are determined mainly by the eGFR value and by markers of kidney damage such as protein in the urine. Staging guides how aggressively doctors monitor and treat the condition:
|
CKD Stages |
Kidney Function Level |
What It Means |
|
Stage 1 |
Normal or high eGFR with kidney damage |
Early changes detected through tests |
|
Stage 2 |
Mild decline in kidney function |
Kidney damage with slight reduction in filtration |
|
Stage 3 |
Moderate reduction in kidney function |
Waste begins accumulating in the body |
|
Stage 4 |
Severe reduction in kidney function |
Symptoms often become noticeable |
|
Stage 5 |
Kidney failure |
Dialysis or transplant may be required |
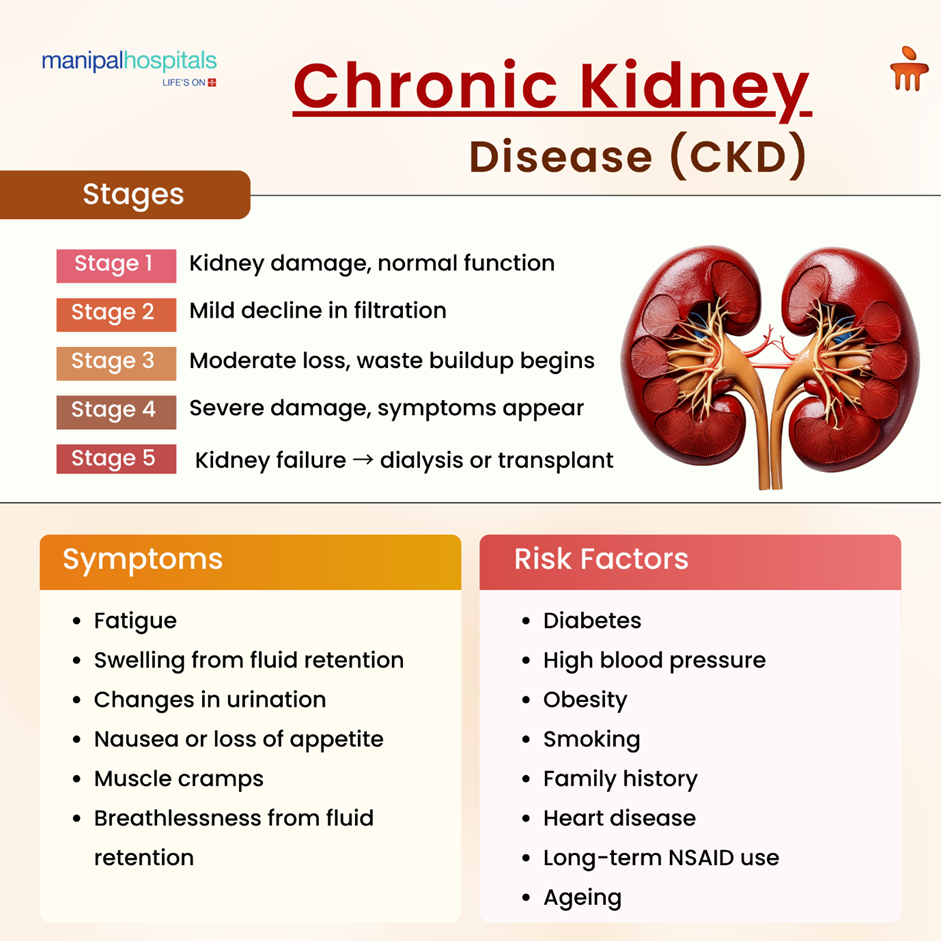
Early CKD stages often don't show any noticeable signs, so regular health check-ups are important for finding them early.
Causes of Chronic Kidney Disease
Several health conditions and lifestyle factors can gradually damage the kidneys over time. In most cases, Chronic Kidney Disease (CKD) does not develop due to a single reason. Instead, it usually results from long-term strain on the kidneys caused by other medical problems or habits that affect overall health.
Some common causes include:
-
Diabetes: High blood sugar can damage the small blood vessels in the kidneys.
-
High blood pressure: Increased pressure in blood vessels can damage kidney tissues.
-
Glomerulonephritis: Inflammation of the kidney’s filtering units.
-
Polycystic kidney disease: A genetic disorder causing cysts in the kidneys.
-
Repeated kidney infections: Frequent infections can scar and weaken kidney tissue.
-
Urinary tract blockages: Obstructions restrict urine flow and strain the kidneys.
-
Long-Term Use of Certain Medications: Long-term use of certain pain relievers or anti-inflammatory drugs can sometimes lead to gradual kidney damage.
Key CKD Risk Factors
Several medical and lifestyle factors can increase the likelihood of developing CKD. Recognising these CKD risk factors allows individuals to take preventive steps and monitor their kidney health.
Important CKD risk factors include:
-
High blood pressure
-
Family history of kidney disease
-
Heart disease
-
Obesity
-
Smoking
-
Increasing age
-
Long-term NSAID use
-
Autoimmune diseases
Awareness of these risk factors enables individuals to adopt preventive measures and undergo regular screening to monitor kidney function.
CKD Symptoms
Early CKD symptoms are often subtle, and many people attribute them to tiredness or ageing. As kidney function declines, symptoms become clearer. Typical signs include:
-
Persistent fatigue and difficulty concentrating
-
Swelling in the legs, ankles, or around the eyes, from fluid retention
-
Changes in urination, such as more frequent visits at night, foamy urine, or reduced volume
-
Loss of appetite, nausea, or an unpleasant metallic taste in the mouth
-
Muscle cramps and persistent itching
-
Shortness of breath when fluid accumulates in the lungs
Because fluid retention is a common and important symptom, monitoring sudden weight gain, increasing puffiness, or breathlessness is essential. If you notice any of these CKD symptoms persistently, seek medical assessment.
How Is Chronic Kidney Disease Diagnosed?
Diagnosis begins with a careful history and simple tests.
-
Doctors use blood tests to measure serum creatinine and calculate the estimated glomerular filtration rate (eGFR), which indicates kidney filtration efficiency.
-
Urine tests show protein or blood, both markers of kidney damage.
-
Imaging, such as an ultrasound or a CT scan, evaluates kidney size and any structural problems.
-
In select cases, a kidney biopsy is performed to identify the specific type of kidney disease and guide treatment.
Together, these tests show the stage of disease and help plan chronic kidney disease treatment.
Chronic Kidney Disease Treatment
The primary objectives of CKD treatment are to slow disease progression, manage symptoms, and prevent complications.
1. Lifestyle Changes
Lifestyle modification is a critical component of maintaining kidney health. Alongside medical care, healthy habits can significantly improve outcomes for people with chronic kidney disease (CKD).
Doctors often recommend the following:
-
Maintaining healthy blood pressure levels
-
Managing blood sugar if diabetes is present
-
Reducing salt intake to prevent fluid retention
-
Staying physically active
-
Avoiding smoking and limiting alcohol intake
-
Drinking adequate water as advised by your doctor
These measures may help slow the progression of kidney damage.
2. Medications
To protect kidney function, doctors may prescribe drugs to treat underlying conditions.
Common medications include:
-
Blood pressure medicines (ACE inhibitors/ARBs): Protect kidney function
-
Diabetes medications: Help control blood sugar
-
Diuretics: Reduce fluid buildup
-
High Cholesterol medications: Lower cardiovascular risk
-
Vitamin supplements: Support bone health
Each patient's condition is considered when making medication plans.
3. Dialysis
Dialysis may be necessary to filter blood when the kidneys are not working well enough.
Types of Dialysis
-
Hemodialysis: Blood is filtered through a dialysis machine
-
Peritoneal dialysis: The lining of the abdomen filters waste using dialysis fluid
Dialysis is usually considered when eGFR falls below 10–15 mL/min, and symptoms of kidney failure appear. It helps the body get rid of extra fluid and waste.
4. Kidney Transplant
In cases of advanced kidney failure, transplantation may become necessary. During this procedure, doctors replace the damaged kidney with a healthy one from a donor. The benefits include improved quality of life, increased independence compared to dialysis, and better long-term health. However, recipients must adhere to lifelong immunosuppressive therapy to prevent organ rejection and maintain graft function.
When Should You See a Doctor?
Many early CKD symptoms can be mistaken for general fatigue or ageing. However, a medical evaluation becomes important if you notice persistent changes.
Consult a doctor if you experience:
-
Unexplained swelling in the legs or ankles
-
Persistent fatigue or weakness
-
Changes in urination patterns
-
High blood pressure that is difficult to control
-
Symptoms of fluid retention such as sudden weight gain
Routine health checks and kidney function tests allow doctors to detect chronic kidney disease (CKD) before it progresses to advanced stages.
FAQ's
In the early stages of CKD, you may not notice any symptoms. Some people, on the other hand, may feel tired, have mild swelling in their legs, experience changes in urination, or have trouble focusing.
CKD is not usually completely curable because kidney damage is often permanent. But an early detection of symptoms and getting the right care can slow down the damage and improve kidney health.
Chronic kidney disease progresses gradually over months or years, whereas acute kidney injury occurs suddenly and may be reversible with timely intervention.
People with CKD may need to cut back on foods rich in sodium, potassium, and phosphorus. Medical advice recommends you avoid processed foods, salty snacks, and too much protein.
With the right care, regular checkups, and changes to their lifestyle, many people with CKD can live full and active lives. Managing your kidneys early on is crucial for their long-term health.





















 7 Min Read
7 Min Read