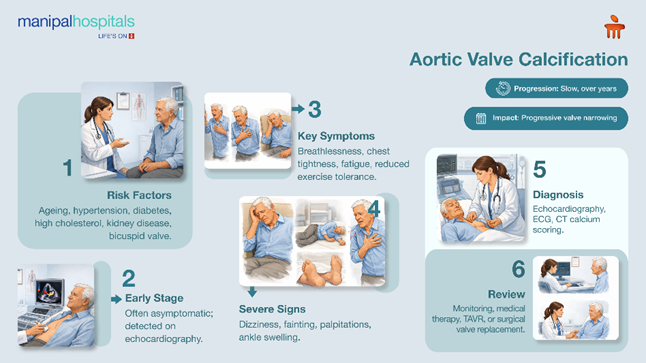
Aortic valve calcification is a common degenerative heart valve disorder that becomes increasingly prevalent with advancing age. The burden of disease is expected to grow as populations live longer, and risk factors such as hypertension, diabetes, and metabolic disorders become more widespread.
In its early stages, the condition may produce few or no symptoms. However, progressive narrowing of the valve can lead to significant complications, including heart failure, arrhythmias, and reduced functional capacity. Understanding risk factors, recognising clinical features, and obtaining timely evaluation are essential for appropriate management.
This blog explains the causes, diagnostic approach, available aortic valve calcification treatment options, and indications for specialist cardiology care.
Synopsis
What Is Aortic Valve Calcification?
Aortic valve calcification refers to the progressive accumulation of calcium deposits on the leaflets of the aortic valve, the structure responsible for directing oxygenated blood from the heart into the aorta. As these deposits increase, the valve becomes thickened and less mobile, restricting its ability to open completely. This process can lead to aortic stenosis.
The condition typically advances over time, gradually narrowing the valve opening. As resistance to blood flow rises, the heart must generate greater pressure to maintain circulation, increasing the workload on the myocardium. Over time, the increased workload can reduce heart function and raise the likelihood of heart failure and other complications.
Causes of Aortic Valve Calcification
Understanding what causes aortic valve calcification helps in prevention and risk management. Some common causes are:
-
Age-related degeneration: Progressive structural wear over time makes the valve leaflets thicker, less flexible, and more prone to calcium accumulation, particularly after the age of 60.
-
Hypertension: Chronic pressure overload increases mechanical stress on the valve and accelerates damage.
-
Hyperlipidaemia: Lipid deposition promotes inflammatory activity that favours calcification.
-
Diabetes mellitus: Metabolic dysfunction contributes to vascular and valvular mineralisation.
-
Chronic kidney disease: Abnormal calcium–phosphate balance significantly heightens risk.
-
Congenital bicuspid aortic valve: Individuals born with this anatomical variation frequently develop calcification at a younger age.
-
Smoking and sedentary lifestyle: These factors amplify systemic inflammation and overall cardiovascular risk.
Recognition of these associations supports risk stratification, closer monitoring, and timely cardiology referral when indicated.
Symptoms of Aortic Valve Calcification
Aortic valve calcification usually develops slowly and can go unnoticed for years. As calcium accumulates and the valve opening gets smaller, the heart has to work harder to move blood forward. This increased workload eventually impacts circulation, leading to symptoms that typically become more noticeable over time.
Patients commonly experience:
-
Breathlessness, first during exertion and sometimes later, even at rest
-
Chest pain, heaviness, or tightness, especially with physical activity
-
Persistent fatigue or a clear reduction in exercise capacity
-
Dizziness or fainting (syncope) when the blood supply to the brain falls
-
Palpitations or awareness of irregular heartbeats
-
Swelling in the ankles or feet in the advanced stages of the disease
Many people attribute these changes to ageing or reduced fitness, which can delay evaluation. Persistent or worsening symptoms should prompt consultation with a cardiologist, since severe valve narrowing can impair heart function and lead to significant complications.
How Is Aortic Valve Calcification Diagnosed?
Getting an early and accurate diagnosis is important to determine how severe the valve narrowing is and how best to treat it.
|
Test |
What It Does |
|
Echocardiography |
Shows valve structure, measures narrowing, and checks heart function. |
|
Electrocardiogram (ECG) |
Records the heart’s electrical activity; detects rhythm problems and signs of heart stress. |
|
CT Calcium Scoring |
Provides a detailed count of calcium deposits on the aortic valve. |
|
Cardiac MRI |
In a complex case, it offers detailed images of the heart structure. |
|
CT Angiography |
Visualises blood vessels and valve anatomy. |
These tests help figure out how severe the disease is and whether medical treatment or surgery is needed.
Aortic Valve Calcification Treatment Options
The right treatment depends on how much the valve has narrowed, your symptoms, and your overall health. Here are some common options:
-
Medical Management: Medications can help control blood pressure, cholesterol, and diabetes. These treatments reduce strain on the heart, but they cannot stop calcification.
-
Regular Monitoring: Echocardiography and ECG track valve function and disease progression, guiding timely intervention.
-
Transcatheter Aortic Valve Replacement (TAVR): A minimally invasive catheter‑based procedure, ideal for older adults or high‑risk patients; faster recovery and fewer complications compared to open surgery.
-
Surgical Aortic Valve Replacement (SAVR): Traditional open‑heart surgery; recommended for younger patients or those with complex valve anatomy and severe symptoms.
-
Lifestyle and Cardiac Rehabilitation: Healthy dietary habits, appropriate physical activity, stopping smoking, and effective stress control play an important role in maintaining long-term heart health.
When Should You See a Cardiologist
Certain symptoms and risk factors warrant timely evaluation by a heart specialist at Manipal Sarjapur road, bangalore. You should arrange an aortic valve calcification consultation in Sarjapur Road if you experience:
-
Persistent shortness of breath or unusual fatigue
-
Chest discomfort during routine physical activityDizziness or fainting episodes
-
A known history of valve disease or congenital heart abnormalities
-
A noticeable or unexplained decline in exercise capacity
Early cardiology assessment helps confirm the diagnosis, determine disease severity, and identify the most appropriate time for intervention, thereby reducing the risk of complications.
Conclusion
Aortic valve calcification is a heart valve disease that can be managed with advanced care. This condition is most often seen in older adults and people with heart risk factors, but early detection makes a big difference. With better diagnostic tools, less invasive procedures, and improved surgeries, today’s treatments can lead to great results and a better quality of life. At the Cardiology, Manipal Hospitals Sarjapur Road, Bangalore our heart specialists offer detailed check-ups, advanced imaging, and personalised care plans tailored to each person with valve disorders.
FAQ's
Common causes include ageing, high cholesterol, hypertension, diabetes, kidney disease, and congenital valve abnormalities. Over time, these factors promote calcium deposition, valve narrowing, and impaired cardiac function.
Yes, medicines and lifestyle changes can help manage symptoms during the initial phase. But if the problem gets worse, replacing the valve is often best for lasting relief.
If you have chest pain, shortness of breath, dizziness, or fainting, see a doctor right away. These symptoms could mean the valve is very narrow and needs urgent attention.
Yes, transcatheter valve replacement is a safe, well-tested option for many people. It is especially appropriate for older adults or those who may not do well with open-heart surgery.
If you have known valve disease, persistent cardiac symptoms, or significant risk factors, seek evaluation from a cardiologist promptly. Early detection enables timely treatment and supports improved long-term outcomes.





















 6 Min Read
6 Min Read