Deep Brain Stimulation (DBS) is a cutting-edge neurosurgical procedure that has transformed the lives of many individuals struggling with debilitating movement disorders. It uses a small device, like a pacemaker, that is implanted to regulate abnormal brain activity. DBS is commonly used to manage conditions such as Parkinson’s disease, Essential Tremor, and Dystonia, helping reduce symptoms like tremors, stiffness, and involuntary movements while improving patients’ quality of life. Since its first use, statistically, over 200,000 individuals worldwide have benefited from this therapy, regaining independence and enhancing their daily activities.
Synopsis
What is Deep Brain Stimulation (DBS)?
Deep Brain Stimulation is a state-of-the-art procedure that involves implanting a small pacemaker-like device, about the size of a coin, into the chest area. This device, called a ‘neurostimulator’, delivers electrical impulses to specific, targeted areas of the brain that control movement. These impulses help to block the abnormal brain signals causing symptoms like tremors, rigidity, and slow movement, which in turn can effectively reset the brain's activity patterns. DBS is not a cure, but a sophisticated solution that can efficiently control symptoms and ensure an improved quality of life for carefully selected patients.
Symptoms that indicate the need for Deep Brain Stimulation
Certain persistent and disabling symptoms may indicate that Deep Brain Stimulation (DBS) could be a suitable treatment option:
-
Tremors (jitters) that are persistent and affect daily activities
-
Severe muscle stiffness (rigidity)
-
Slowed movements (bradykinesia)
-
Symptoms not controlled with medication
-
Motor fluctuations (on-off episodes)
-
Medication is wearing off quickly
-
Involuntary movements (dyskinesia)
-
Difficulty in walking or balance
-
Reduced ability to perform daily tasks
The Deep Brain Stimulation surgery
The Deep Brain Stimulation surgery is a meticulously planned and executed procedure, typically performed in two main stages:
Brain mapping and electrode implantation
The procedure starts with implanting the electrodes precisely into specific target areas of the brain. This is often done while the patient is awake (but comfortable and pain-free), allowing the neurosurgeon to monitor brain activity and test the effects of stimulation in real-time. This ensures optimal precision in placement for maximum therapeutic benefit and contributes to the high success rates of this procedure.
Neurostimulator (IPG) implantation
Once the electrodes are secured in place, they are connected to a neurostimulator by thin wires running under the skin. The neurostimulator is usually implanted under the skin near the collarbone or in the chest and contains the battery and the computer chip that generates the electrical pulses. Post-surgery, there is a recovery period before the neurostimulator is programmed. Initial programming usually occurs a few weeks after the surgery, to allow sufficient time for healing.
When is Deep Brain Stimulation treatment required?
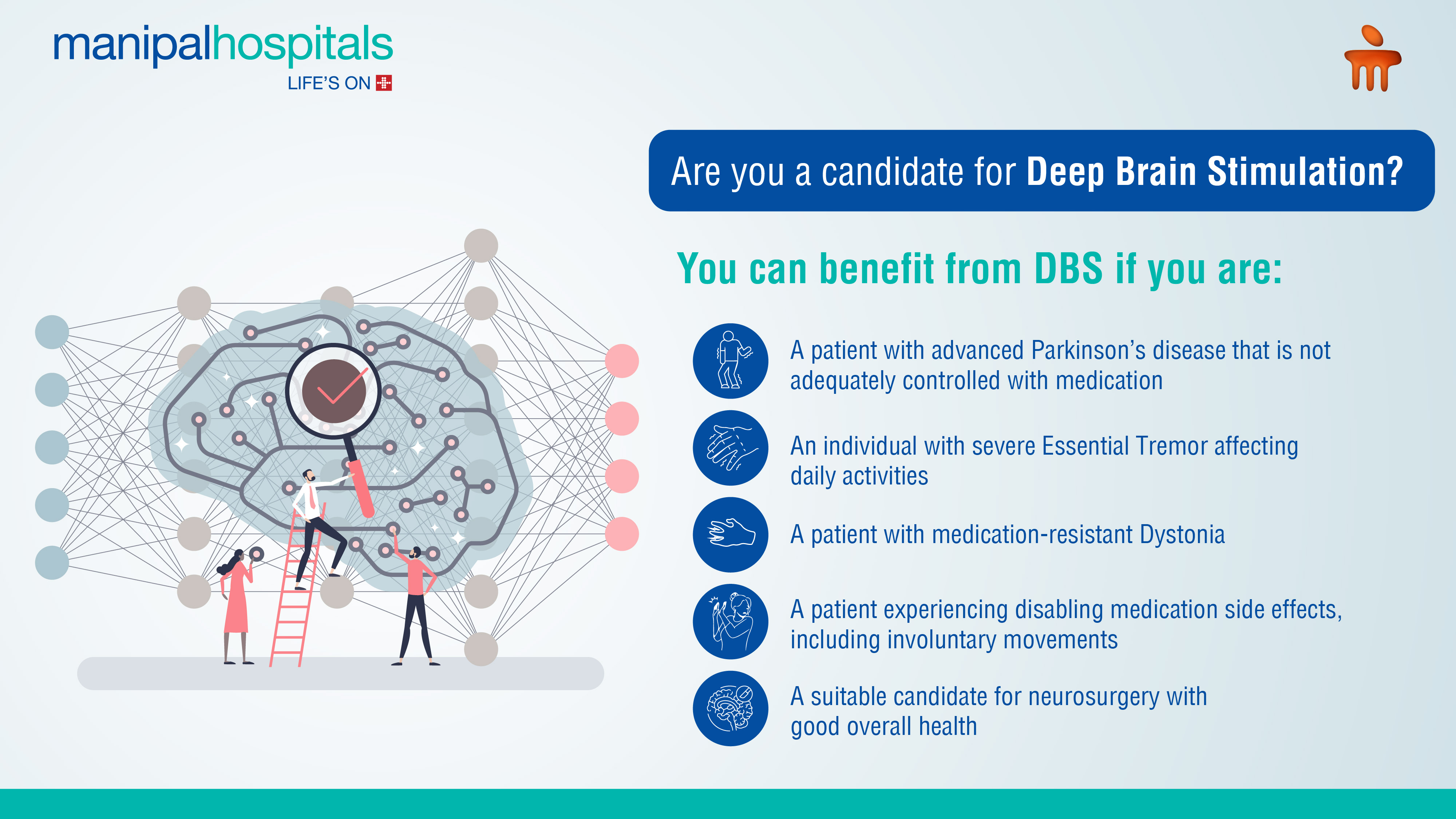
Deep Brain Stimulation treatment is primarily used for movement disorders that have not responded adequately to medication. A thorough evaluation by a multidisciplinary team, including neurologists and neurosurgeons, can determine if a patient is a suitable candidate for this life-changing therapy. Candidates for this procedure include patients with:
-
Parkinson's Disease - DBS can be especially helpful in managing tremors, rigidity, bradykinesia (slow movement), and dyskinesia (involuntary movements). Many patients experience a 50-60% reduction in medication needs, leading to fewer side effects.
-
Essential Tremor- DBS is capable of significantly reducing severe tremors in the hands, arms, and head.
-
Dystonia - DBS helps to alleviate sustained muscle contractions that cause twisting and repetitive movements or abnormal fixed postures.
Important Guidelines
Navigating DBS therapy involves specific care considerations. Following a checklist of Yes and No rules helps ensure better recovery and prolonged DBS benefits:
|
Yes |
No |
|
Attend all follow-up appointments for programming and device checks. |
Do not ignore any changes in your symptoms or device function. |
|
Keep the incision sites clean and dry as instructed by your medical team. |
Never attempt to adjust your neurostimulator settings without medical supervision. |
|
Always carry your DBS identification card, especially when travelling. |
Avoid exposing the device to strong magnetic fields (e.g., MRI machines) unless specifically cleared by your doctor for MRI-compatible devices and settings. |
|
Report any unusual symptoms, pain, or signs of infection immediately to your doctor. |
Refrain from participating in contact sports or activities that could damage the implanted device |
|
Engage in rehabilitation therapies as recommended to maximise functional improvements. |
Never stop taking prescribed medications unless advised by your doctor, as DBS often works best in conjunction with other treatments. |
Conclusion
Deep Brain Stimulation can significantly improve symptom control in conditions like Parkinson’s disease, Essential Tremor, and Dystonia when medications are not effective. It helps enhance daily functioning and overall quality of life. If you or a loved one is considering this innovative treatment, understanding the procedure and the journey involved can provide immense clarity and peace of mind. Talk to our expert neurology team at Manipal Hospitals Mukundapur for a customised treatment plan that offers optimal symptom control and minimal side effects, often achieving up to 70-80% improvement in motor symptoms. At Manipal Hospitals, our commitment to pioneering medical advancements ensures that patients receive the highest standard of care, guided by expert neurosurgeons and dedicated support staff.
FAQ's
The battery life varies depending on the type of device and stimulation settings. Non-rechargeable batteries typically last 3-5 years, while rechargeable batteries can last up to 15 years before needing replacement.
Most patients undergoing Deep Brain Stimulation do not feel the electrical stimulation during treatment. If any sensation occurs, the device settings can usually be adjusted by the doctor to make it unnoticeable while still maintaining the desired therapeutic benefits.
As with any surgery, there are risks, including infection, bleeding, and adverse reactions to anaesthesia. Specific to DBS, there's a small risk of lead misplacement or device malfunction. Your medical team will discuss all potential risks with you.
Yes, the neurostimulator can be turned off or adjusted at any time by your doctor using a special programmer. Patients also typically have a handheld device to make minor adjustments within a safe range.
While some patients experience immediate relief, the full benefits of DBS often become apparent gradually over weeks to months, as the device is precisely programmed and adjusted to your individual needs.





















 8 Min Read
8 Min Read