Imagine going for a pleasant evening stroll, only to find that after just a few hundred metres, your legs begin to feel heavy, cramped, or strangely weak. You stop, lean forward against a railing, or sit down for a moment, and almost magically, the discomfort vanishes. You start walking again, only for the cycle to repeat. This "stop-and-go" life is the hallmark of a condition known as neurogenic claudication. For many, the most frustrating part of neurogenic claudication is the unpredictability. You might feel perfectly fine while sitting in a chair or cycling yet find yourself unable to walk through a grocery store without needing to lean over the shopping cart for relief. Because the pain often disappears when you rest, it’s easy to dismiss it as "just getting older" or simple muscle fatigue. However, neurogenic claudication is actually a specific neurological signal from your spine, often acting as the primary messenger for an underlying condition called spinal stenosis.
Understanding the neurogenic claudication causes and recognising the early warning signs is the first step toward regaining your mobility. This blog explores why these leg symptoms occur, how to differentiate them from circulation issues, and the various paths available for neurogenic claudication treatment. By addressing the root cause in the spine, you can move away from the frustration of limited mobility and back toward an active, steady lifestyle.
What Is Neurogenic Claudication?
The term "neurogenic claudication" is derived from the Latin word "claudicare," meaning to limp. Unlike many types of back pain that stay localised in the spine, neurogenic claudication is a "nerve-based" discomfort that manifests primarily in the legs. It occurs when the nerves in your lower back (the lumbar spine) become compressed as they travel to your lower extremities.
When you stand or walk, the natural curve of your lower back narrows the space available for these nerves. If that space is already tight due to spinal changes, the nerves become "squeezed," much like a garden hose being stepped on. This compression interferes with the nerve's ability to transmit signals and receive blood flow, leading to the classic neurogenic claudication symptoms of pain, tingling, and weakness.
Crucially, neurogenic claudication is a clinical syndrome, not a standalone disease. It is a cluster of symptoms that tells your doctor there is a mechanical "traffic jam" in your spinal canal that needs attention.
Common Neurogenic Claudication Causes
Our spines go through a lot of wear and tear over the decades. While there are several neurogenic claudication causes, they all share a common theme: a reduction in the space available for the spinal cord and nerve roots.
-
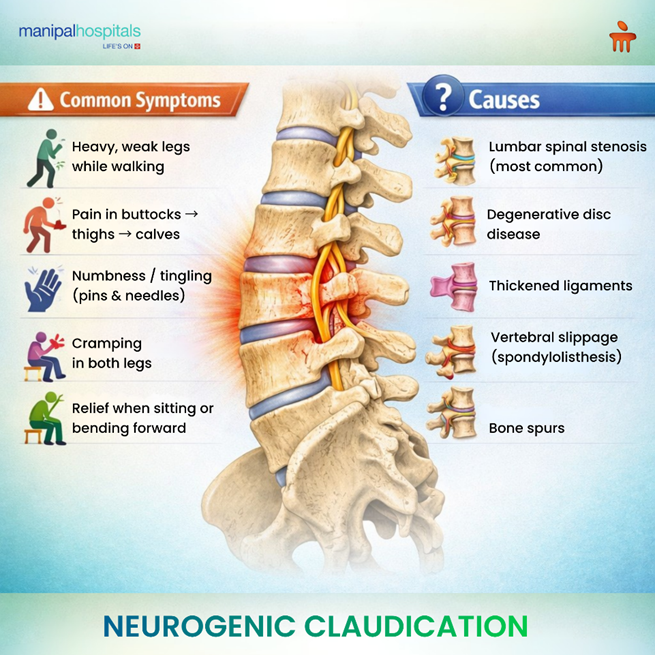
Lumbar Spinal Stenosis: This condition is the most frequent culprit. Over time, the spinal canal can narrow due to osteoarthritis, causing the bones to crowd the nerve pathways.
-
Degenerative Disc Disease: As spinal discs lose their height and "bulge" outward, they can encroach on the space where nerves exit the spine, triggering neurogenic claudication.
-
Thickened Ligaments: The ligaments that support the spine can become stiff and thick (hypertrophy) with age, buckling inward and pressing against the nerves.
-
Spondylolisthesis: This occurs when one vertebra slips forward over another, misaligning the "tunnel" through which the nerves pass and causing neurogenic claudication.
-
Bone Spurs (Osteophytes): In response to joint friction, the body may grow small bony projections that can poke into the spinal canal.
Understanding these neurogenic claudication causes helps specialists tailor a plan that doesn't just mask the pain but addresses the physical narrowing in the spine.
Recognising Neurogenic Claudication Symptoms
One of the most unique aspects of this condition is that the symptoms are "position-dependent." You might have zero pain while lying flat, but significant distress while standing upright.
Commonly reported neurogenic claudication symptoms include:
-
The "Heavy Leg" Sensation: A feeling that your legs weigh a ton, making it difficult to lift your feet properly while walking.
-
Bilateral Cramping: Pain or tightness that usually affects both legs simultaneously, often starting in the buttocks and moving down to the calves.
-
The Shopping Cart Sign: A classic sign where a person finds significant relief by leaning forward (flexing the spine), which temporarily opens up the spinal canal.
-
Paresthesia: Feelings of "pins and needles," numbness, or tingling that intensify after standing for a long duration.
-
Positional Relief: Symptoms almost always improve when sitting down or bending forward at the waist.
If you notice that your neurogenic claudication symptoms are limiting your ability to perform daily chores or enjoy hobbies, it is a clear sign that the nerves are under significant pressure.
The Path to Diagnosis
To plan effective neurogenic claudication treatment, the doctor first needs to understand exactly what is causing the nerve pressure in the spine. Diagnosis usually comes from a combination of your symptoms, a physical examination, and imaging tests.
-
Clinical History: Your doctor will ask about the "shopping cart sign" and how long you can walk before the neurogenic claudication sets in.
-
MRI (Magnetic Resonance Imaging): is the most reliable method for diagnosing neurogenic claudication. It allows the doctor to see the exact degree of nerve compression and identify which ligaments or discs are at fault.
-
CT Myelogram: If an MRI isn't possible, a CT scan with a special dye can highlight the pressure points on the spinal nerves.
-
Physical Assessment: Testing your reflexes and strength while in different positions can help confirm that the symptoms are indeed neurogenic claudication.
Neurogenic Claudication Treatment: What Actually Works?
The goal of neurogenic claudication treatment is to reduce the pressure on the spinal nerves and improve your walking distance. Most doctors prefer a "staircase" approach, starting with the least invasive options.
Non-Surgical Strategies
Activity modification: Some patients benefit from reducing activities that trigger symptoms and learning positions that relieve pressure on the spine. This may mean avoiding long periods of standing or taking breaks during walks.
-
Physiotherapy: Targeted exercises can improve posture, strengthen supportive muscles, and help reduce strain on the lower back. Many physiotherapy plans focus on flexion-based movements, since bending forward often eases symptoms.
-
Medications: Doctors may prescribe pain relief or anti-inflammatory medicines to help control discomfort. In certain cases, other medicines may be used depending on how the symptoms behave.
-
Epidural injections: For some patients, a steroid injection near the affected nerves may help reduce inflammation and provide temporary relief. This does not cure the narrowing, but it can sometimes make symptoms easier to manage.
Surgical Interventions
If conservative neurogenic claudication treatment is not effective in relieving symptoms, then there is an option for neurogenic claudication treatment.
-
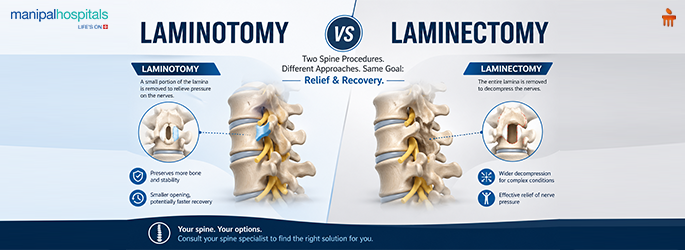
Decompression (Laminectomy): A small part of the bone or ligament is removed by a surgeon. This is an effective form of neurogenic claudication treatment for stenosis.
-
Interspinous Spacers: Spacers are inserted between the vertebrae, which then makes them lean forward. This action permanently opens up the spinal canal for the nerves.
How to Manage Neurogenic Claudication in Daily Life
Neurogenic claudication treatment is incomplete without your own efforts. Your habits have a huge impact on how much neurogenic claudication affects your life.
Here are some tips that could be helpful in your daily life:
-
Short breaks in sitting during long walks or outings
-
Maintain a slightly forward-leaning stance during standing if comfortable doing so
-
Engage in low-impact physical activities, e.g., stationary cycling or short walks
-
Avoid lifting or doing physical activities unless recommended by your doctor
-
Maintain your back and abdominal muscles with doctor-approved exercises
-
Wear comfortable shoes, especially if you plan on being on your feet for long periods of time
This is not an alternative form of neurogenic claudication treatment, but it is something that could make your life with neurogenic claudication more tolerable.
When to Seek Medical Help
It is important to see a specialist if your neurogenic claudication begins to interfere with your independence. While the condition often develops slowly, there are "red flag" situations. You should consult a doctor if your neurogenic claudication is accompanied by:
-
Sudden loss of bowel or bladder control.
-
Progressive weakness that makes your legs buckle.
-
Numbness in the "saddle area" (inner thighs and groin).
-
Pain that persists even when you are lying down.
A specialist can offer a tailored neurogenic claudication treatment plan that helps prevent long-term nerve damage and keeps you on your feet.
Conclusion
Neurogenic claudication can make simple movement feel unexpectedly difficult, especially when walking or standing triggers leg pain, heaviness, numbness, or weakness. Because the symptoms are often tied to spinal stenosis, proper evaluation is important to confirm the cause and rule out other problems. If you are experiencing these leg symptoms, consulting a spine specialist at Manipal Hospitals can help you find the right neurogenic claudication treatment, ensuring you receive the personalised care your back deserves.