It is a common experience to wake up and find that your back or neck feels significantly stiffer than it did a few years ago. You might find that sitting in a chair for a long duration now results in a dull, persistent ache that wasn't there before or that a simple task like bending over to tie your shoes requires more deliberate effort. This physical change is often the result of a process that is frequently misunderstood. Despite its intimidating name, this condition is not actually a "disease" in the traditional sense, such as an infection or a sudden illness. Rather, it is a gradual mechanical breakdown of the intervertebral discs that act as the structural support between the bones of your spine.
In many cases, once the specific nature of the breakdown is understood, clarity and function can be restored through a combination of lifestyle adjustments and specialised clinical care. This article explores the biological reality of spinal ageing, how to identify the specific signals your body is sending, and the comprehensive pathways available for degenerative disc disease treatment.
Understanding the Disc Degeneration Meaning
To get a handle on how to address the pain, we first need to look at what disc degeneration actually involves. Your spine is made up of bones called vertebrae. Between these bones are small, circular cushions known as spinal discs. These discs have a very important job: they keep the bones from rubbing against each other, and they allow your spine to bend and twist. Each disc has a tough, fibrous outer layer and a soft, central part that contains a lot of water.
The disc degeneration is simply the process of these cushions changing over time. As we age, the soft middle part of the disc begins to lose some of its water. As the disc loses water, it becomes thinner and less effective at keeping the bones of the spine separated. At the same time, the tough outer layer can develop small cracks. When the disc thins out, the space between your vertebrae gets smaller, which can cause the joints in your spine to rub together or put pressure on the nearby nerves. This overall process is what doctors refer to as degenerative spine disease. It is a mechanical change in how your back supports your weight and handles movement.
Causes of Degenerative Disc Disease
Degenerative disc disease is primarily a result of age-related wear and tear on the spinal discs. Over time, the discs that act as cushions between the vertebrae gradually lose their flexibility, elasticity, and ability to absorb shock. As people age, these discs begin to dry out due to loss of water content, making them thinner and less effective.
In addition to natural ageing, minor injuries and repeated stress on the spine can contribute to degeneration. Everyday movements, sports, or even small, unnoticed injuries may cause tiny tears in the outer layer of the disc. These tears can lead to inflammation or allow the disc to bulge or shift out of place, sometimes pressing on nearby nerves.
Other contributing factors include repetitive physical strain, heavy lifting, or long-term overuse, which accelerate the breakdown of discs. Lifestyle and health factors such as obesity, smoking, and physically demanding occupations may further increase the risk by placing additional stress on the spine.
Overall, while ageing remains the most common cause, degenerative disc disease often develops due to a combination of natural degeneration, mechanical stress, and lifestyle-related factors.
Recognising Degenerative Disc Disease Symptoms in Your Daily Life
Because this is a gradual process, the signs often show up slowly. You might not have one specific "injury" that you can point to. Instead, the degenerative disc disease symptoms often start as a dull ache that comes and goes. Below are some common symptoms:
-
Back or neck pain: Often the first sign, ranging from a dull ache to sharper discomfort
-
Pain with activity: May worsen with long sitting, bending, or lifting, and improve with rest or light movement
-
Radiating pain: Pain may spread to the arms or legs; these are common disc degeneration symptoms when nerves are involved
-
Numbness or tingling: A pins-and-needles sensation in the arms or legs
-
Muscle weakness: A more serious symptom that should not be ignored
-
Fluctuating symptoms: Pain may come and go, with flare-ups followed by relief
Mild symptoms may stay localised, while more severe cases can involve nerve pressure and affect movement or strength.
How Medical Professionals Check Your Spine?
If you decide to see a doctor for your back or neck pain, they will start with a conversation about your history. The tests below are also done:
-
Physical Examination: The doctor will likely ask you to move in certain ways to check your flexibility and see which positions trigger the discomfort. They will also check your reflexes and muscle strength.
-
Magnetic Resonance Imaging: This procedure is the most common tool used to see the discs. A scan provides an obvious picture of the soft tissues.
-
Computed Tomography Scan: This procedure is very helpful for seeing bone spurs or other structural changes in the vertebrae.
-
X-Rays: While an X-ray cannot see the discs themselves, it can show the doctor how much space is left between your bones.
Starting the Process: Initial Degenerative Disc Disease Treatment
The excellent news is that for about ninety per cent of people, degenerative disc disease treatment does not involve surgery. Most of the time, the body just needs some help to calm the inflammation and strengthen the muscles that support the back.
-
Focusing on Physical Therapy - Physical therapy is often the most effective tool we have. A therapist won't just give you exercises; they'll teach you how to move to protect your spine. The focus is usually on strengthening your "core" muscles, the ones in your abdomen and lower back. When these muscles are strong, they act like a natural brace for your spine, taking the pressure off the thinning discs.
-
Using Medications Carefully - To help you get through a flare-up, your doctor might suggest non-steroidal anti-inflammatory drugs. These medications help lower the swelling around the discs and joints. If your muscles are very tight or spasming, the doctor might prescribe a short course of muscle relaxants to help the area settle down.
-
Making Changes to Your Daily Routine - Small changes in how you live can greatly affect your spine. If you spend a lot of time sitting, the doctor will likely suggest that you get up and move every thirty minutes. Staying hydrated is also important for your general health, and maintaining a healthy body weight is one of the best things you can do for your back. Every extra pound you carry puts more mechanical pressure on those spinal discs. If you use tobacco, your doctor will likely encourage you to stop. Nicotine is known to reduce the blood flow to the discs, which can make degenerative spine disease progress much faster.
Advanced Options for Degenerative Disc Disease Treatment
If you have tried physical therapy and medication for several weeks and you are still in significant pain, your doctor might talk to you about more advanced options.
-
Injections: Sometimes, a doctor can inject an anti-inflammatory medication (a steroid) directly into the space near the irritated nerve. This can provide a period of significant relief, which gives the body time to heal and makes it easier for you to do your strengthening exercises.
-
Surgical Options: Surgery is usually a last resort, used only if there is a serious problem like a nerve being crushed or if the pain is so bad that you cannot live your life.
-
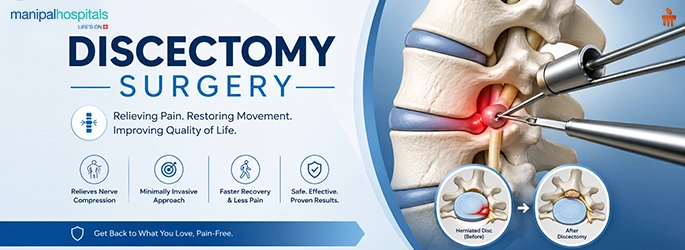
One option is a discectomy, where the part of the disc pressing on the nerve is removed.
-
Another is spinal fusion, where two vertebrae are joined together to stop the painful movement between them.
-
A more modern choice in degenerative disc disease treatment is artificial disc replacement, where the worn-out disc is replaced with a mechanical one that allows the spine to keep moving naturally.
-
When Should You See a Specialist?
While most back pain settles down on its own, there are some signs that you should not ignore. You should schedule a visit with a doctor if:

-
Your pain is so severe that you cannot perform your professional work or take care of your home.
-
You notice that your legs or feet feel weak, or you find yourself tripping more often.
-
The numbness or tingling in your limbs is getting worse or staying there all the time.
-
You have tried resting and using over-the-counter medication for three or four weeks, and the pain has not improved at all.
Getting an early evaluation is the best way to start a proper degenerative disc disease treatment plan before the problem becomes more difficult to manage.
Conclusion
Navigating life with degenerative spine disease can feel like a challenge, but it is one that you can meet with a proactive approach. If pain continues, starts spreading, or begins to affect daily activity, it is important to get it evaluated rather than waiting for it to settle on its own. A structured plan, guided by a specialist, helps avoid unnecessary delays and complications. At Manipal Institute of Robotic Spine Surgery (MIRSS), our spine care team looks at your symptoms, scans, and lifestyle together to guide the next steps of treatment.