
Noticing blood in the stool can be alarming. Even a faint streak on toilet paper or a reddish tinge in the toilet bowl is enough to make anyone pause and wonder what might be wrong. While the sight of blood naturally causes concern, it does not always point to a serious problem. In many cases, the reason is something common and treatable, such as haemorrhoids or minor irritation in the anal area. At other times, rectal bleeding may be linked to conditions affecting the stomach, intestines, or colon that require medical attention. The key lies in understanding what the bleeding looks like, where it may be coming from, and whether other symptoms are present.
This blog takes you through the possible reasons for blood in stool, what it could signify, and when to worry about the condition of blood in stool.
Synopsis
- What Does Blood in Stool (Rectal Bleeding) Actually Look Like?
- Common Blood in Stool Causes
- What Blood in Stool Without Pain May Indicate?
- When to Worry About Rectal Bleeding?
- How Do Doctors Identify the Source of Bleeding?
- Treatment Options for Blood in Stool
- Risk Factors That Increase the Risk of Rectal Bleeding
- Prevention and Long-Term Digestive Health
- Conclusion
What Does Blood in Stool (Rectal Bleeding) Actually Look Like?
The way blood appears in stool often provides useful information about where the bleeding may be occurring within the digestive tract. Because the digestive system stretches from the mouth to the rectum, the colour and texture of the blood can change depending on how long it has been in the body and where it originated.
You may notice:
-
Bright red blood coating the stool or seen on toilet paper
-
Maroon or dark red blood mixed within the stool
-
Black, tarry stools with a strong odour
-
Occult blood in stool, which is not visible but can be detected through laboratory testing
The following is the common appearance of rectal bleeding and what it might suggest:
|
Appearance of Blood |
Possible Source |
What It Means |
|
Bright red blood |
Rectum or anus |
It usually comes from the lower digestive tract. Because the blood hasn’t travelled far, it still looks fresh and bright red. |
|
Dark red or maroon blood |
Colon or small intestine |
Blood that moves through part of the digestive tract can darken as it mixes with stool. |
|
Black, tarry stools (melena) |
Stomach or upper small intestine |
Blood that has been digested turns stool black, sticky, and often foul-smelling. |
|
Occult blood (not visible) |
Anywhere in the digestive tract |
Blood that cannot be seen with the naked eye and is usually found through stool tests during screening. |
Common Blood in Stool Causes
Before jumping to serious conclusions, it is important to recognise that many cases of blood in stool arise from relatively common conditions. The digestive tract is lined with delicate tissue that can bleed for various reasons.
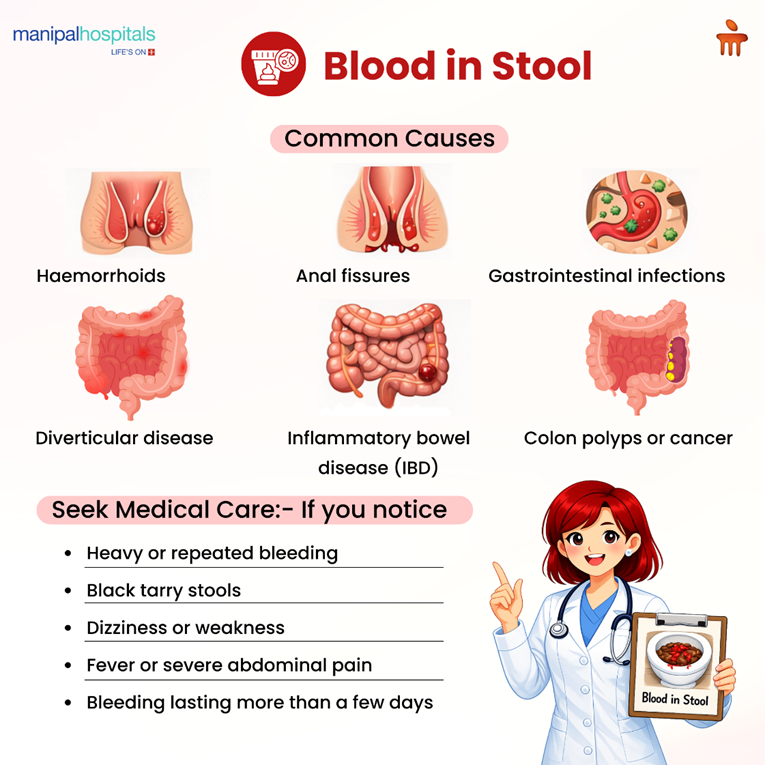
Here are some of the more common causes of blood in stool:
-
Haemorrhoids
Swollen veins in the rectum or anus can bleed during bowel movements, especially with straining or constipation. The bleeding is typically bright red and painless.
-
Anal Fissures
Small tears in the lining of the anus can cause streaks of blood, often accompanied by sharp pain during passing stools.
-
Gastrointestinal Infections
Certain bacterial infections can irritate the intestinal lining, leading to diarrhoea mixed with blood and mucus.
-
Inflammatory Bowel Disease (IBD)
Conditions such as ulcerative colitis and Crohn’s disease can cause chronic inflammation and recurrent bleeding.
-
Diverticular Disease
Small pouches in the colon wall can bleed suddenly and sometimes heavily.
-
Colorectal Polyps or Cancer
Abnormal growths in the colon may bleed slowly over time, often presenting as occult blood in stool.
Each of these reasons for blood in stool has distinct characteristics, and understanding the pattern helps narrow down the diagnosis.
What Blood in Stool Without Pain May Indicate?
Bleeding that occurs without discomfort often creates more anxiety because there is no obvious trigger like straining or fissure pain. Blood in stool without pain can be linked to haemorrhoids, but it may also signal more serious underlying causes.
Painless bleeding is particularly concerning in adults over 45, especially if accompanied by:
-
Unexplained weight loss
-
Changes in bowel habits
-
Fatigue or signs of anaemia
-
A family history of colorectal cancer
Painless bleeding from the colon may occur due to polyps, vascular malformations, or malignancy. This does not mean that cancer is the most likely cause, but it does warrant proper evaluation rather than watchful waiting.
When to Worry About Rectal Bleeding?
Not every episode requires emergency care, but some situations demand prompt medical attention. Recognising warning signs can prevent complications and ensure timely treatment. Seek urgent evaluation if you experience:
-
Heavy bleeding that fills the toilet bowl
-
Dizziness, fainting, or weakness
-
Black, tarry stools with abdominal pain
-
Persistent bleeding lasting more than a few days
-
Associated with fever or severe abdominal cramps
Understanding when to worry about blood in stool depends on the severity, frequency, and associated symptoms. A single streak after constipation may be minor. Ongoing or unexplained bleeding should never be ignored.
Understanding when to worry about blood in stool depends on the severity, frequency, and associated symptoms. A single streak after constipation may be minor. Ongoing or unexplained bleeding should never be ignored.
How Do Doctors Identify the Source of Bleeding?
Diagnosing the cause of blood in stool usually begins with a detailed medical history and physical examination. Doctors may ask about the colour of the blood, associated symptoms, medication use, and family history of digestive disorders. Based on this information, they may recommend specific diagnostic tests to locate the source of bleeding:
|
Diagnostic Test |
What It Detects |
When It Is Recommended |
Preparation Required |
Approximate Duration |
|
Faecal Occult Blood Test (FOBT) |
Hidden microscopic blood |
Routine screening or unexplained anaemia |
Stool sample collection at home |
A few minutes (lab processing required) |
|
Faecal Immunochemical Test (FIT) |
Detects hidden blood in stool |
Screening for colorectal cancer |
Stool sample collection |
A few minutes |
|
Colonoscopy |
Polyps, cancer, IBD, diverticula |
Persistent bleeding, positive FOBT, high-risk patients |
Bowel preparation with laxatives |
30–45 minutes |
|
Sigmoidoscopy |
Rectum and lower colon lesions |
Suspected distal bleeding |
Limited bowel prep |
15–20 minutes |
|
Upper GI Endoscopy |
Stomach and duodenal ulcers |
Black tarry stools or suspected upper GI bleeding |
Fasting for 6–8 hours |
15–30 minutes |
|
CT Angiography |
Active bleeding sites |
Severe or ongoing bleeding |
Contrast injection |
20–30 minutes |
These tests help doctor determine not only where the bleeding is coming from but also what treatment approach may be most effective.
Treatment Options for Blood in Stool
Management depends entirely on the underlying cause. Treating the symptom alone is not enough; the source of bleeding must be addressed.
For Haemorrhoids and Fissures
-
Increased fibre intake
-
Adequate hydration
-
Topical creams
-
Sitz baths
-
In selected cases, minor procedures
For Infections
-
Targeted antibiotics if bacterial
-
Oral rehydration
-
Temporary dietary adjustments
For Inflammatory Conditions
-
Anti-inflammatory medication
-
Immune-modulating therapy
-
Long-term monitoring
For Polyps
-
Removal during colonoscopy
For Ulcers
-
Acid-suppressing medication
-
Treatment for Helicobacter pylori if present
Treatment for blood in stool is tailored to individual findings. In some cases, surgical intervention may be necessary, especially if bleeding is severe or caused by structural disease.
Risk Factors That Increase the Risk of Rectal Bleeding
Certain lifestyle and medical factors increase susceptibility to bleeding. Being aware of them allows proactive screening and prevention.
-
Chronic constipation
-
Low-fibre diet
-
Smoking
-
Long-term use of NSAIDs
-
Family history of colorectal cancer
-
Chronic liver disease
-
Inflammatory bowel disorders
Regular screening becomes especially important for individuals with these risk factors, even if symptoms are mild.
Prevention and Long-Term Digestive Health
While not all causes can be prevented, many can be reduced with consistent habits. Protecting your digestive system involves daily choices rather than occasional fixes, especially since preventive care significantly lowers the chances of serious disease presenting late. Focus on:
-
A fibre-rich diet including fruits, vegetables, and whole grains
-
Drinking adequate water
-
Avoiding excessive straining during bowel movements
-
Limiting alcohol intake
-
Participating in age-appropriate colorectal screening
Conclusion
Seeing blood in stool can feel alarming, but clarity replaces fear when you understand the possibilities. From haemorrhoids to inflammatory conditions and, in rare cases, more serious disorders, the causes vary widely. The colour, frequency, associated symptoms, and your personal risk profile all help determine the urgency of evaluation. If you are uncertain about whether it is serious, it is always safer to seek medical advice rather than assume it will resolve on its own. Early diagnosis often leads to simpler treatment and better outcomes.
For those seeking specialised evaluation and treatment for blood in stool in Malleshwaram, Bangalore, visit our team of experienced gastroenterologists at Manipal Hospital Malleshwaram for thorough assessment and appropriate care.
FAQ's
Stress by itself does not directly cause bleeding in the digestive tract. However, it can worsen existing conditions such as irritable bowel syndrome or inflammatory bowel disease, which may increase the likelihood of symptoms. If bleeding occurs, it is important to rule out physical causes rather than attributing it purely to emotional strain.
No. Colon cancer is only one of several possible causes. In fact, most cases are linked to benign conditions such as haemorrhoids or minor tears. That said, persistent or unexplained bleeding should always be evaluated to exclude serious disease.
Yes. Foods such as beetroot, red gelatin, or artificial colouring can sometimes give stools a reddish tint. However, true bleeding usually appears as streaks, clots, or mixed blood rather than a uniform colour change. When in doubt, medical testing can confirm.
If the bleeding is minor and clearly linked to constipation or straining, short observation may be reasonable. However, repeated episodes, associated symptoms, or bleeding in individuals over 45 should not be delayed for assessment.
Yes. In children, common causes include constipation-related fissures, infections, or food allergies. Any persistent or unexplained bleeding in a child requires evaluation by a paediatrician to ensure appropriate treatment.





















 8 Min Read
8 Min Read

















