Progressive muscle weakness is more than just feeling tired; it is a gradual decline in muscle strength that can significantly affect daily life. While it can sometimes be a symptom of various conditions, understanding its underlying causes and recognising early warning signs is crucial for timely intervention and better management.
Synopsis
What is Progressive Muscle Weakness?
Progressive muscle weakness refers to a condition where muscle strength deteriorates slowly over time, making everyday tasks increasingly difficult. Unlike temporary fatigue or acute weakness from injury, this type of weakness is often chronic and can spread to different muscle groups. It can affect mobility, coordination, and even vital functions like breathing and swallowing. This kind of progressive muscle weakness is a common symptom of a condition called muscular dystrophy.
What is Muscular Dystrophy?
Muscular dystrophy refers to a group of more than 30 genetic disorders where the skeletal muscles weaken and degenerate over time. These disorders result in faulty or missing proteins needed for healthy muscle function. While rare, muscular dystrophy affects millions worldwide. However, early diagnosis and management can help individuals with certain types maintain mobility and a significantly improved quality of life for extended periods.
Muscular Dystrophy Types
Knowing the different types of muscular dystrophy helps to determine the treatment plan accurately:
-
Duchenne Muscular Dystrophy (DMD): The most common and severe childhood form, primarily affecting boys. Symptoms typically appear between ages 2-3.
-
Becker Muscular Dystrophy (BMD): Similar to DMD but less severe and progresses more slowly, with symptoms often appearing in adolescence or adulthood.
-
Myotonic Muscular Dystrophy: The most common type seen in adults, it is characterised by myotonia (prolonged muscle contractions) and often affects multiple body systems.
-
Limb-Girdle Muscular Dystrophy (LGMD): Affects muscles around the hips and shoulders, with varying severity and age of onset.
-
Facioscapulohumeral Muscular Dystrophy (FSHD): Primarily affects muscles of the face, shoulder blades, and upper arms.
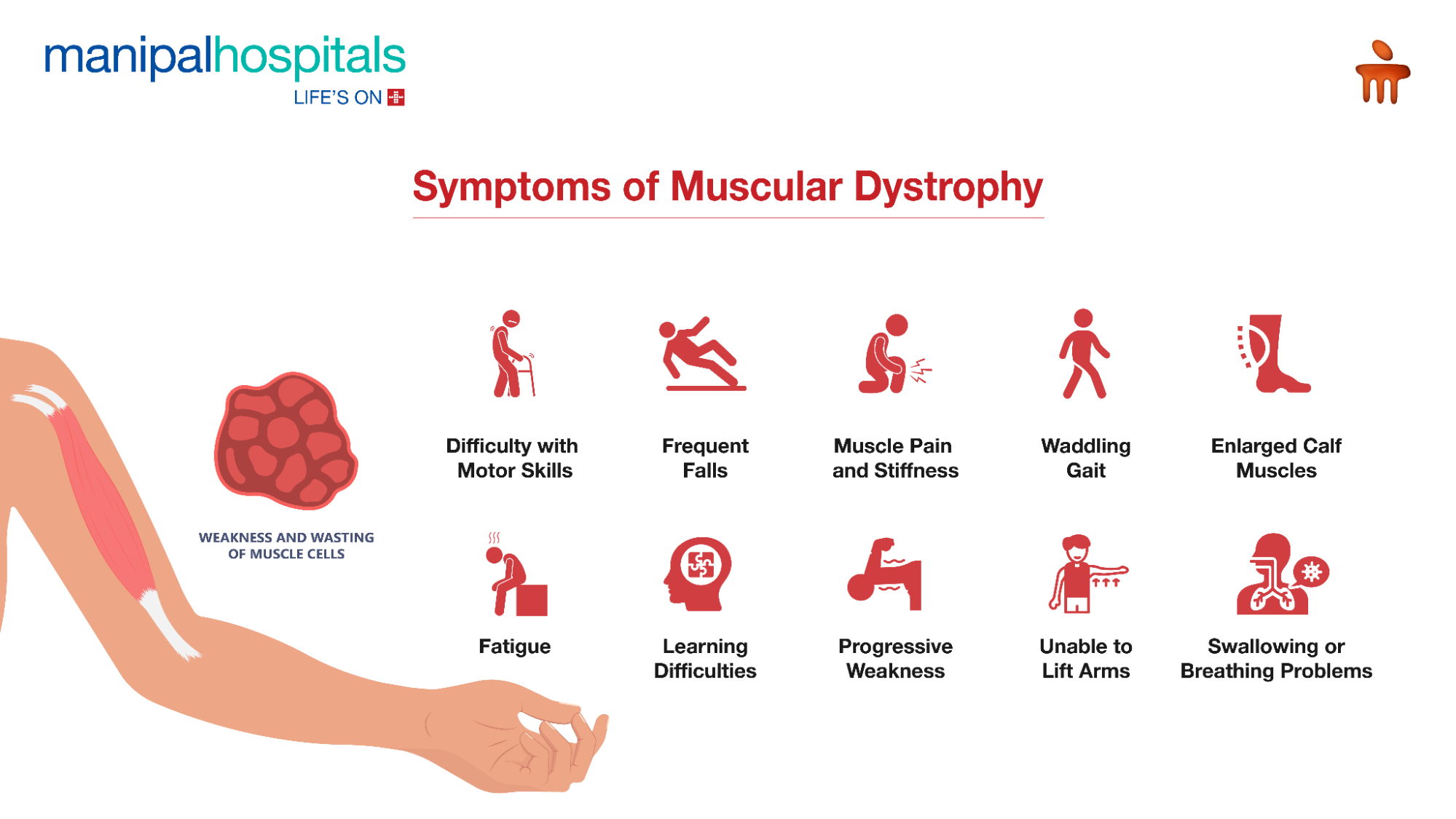
Muscular Dystrophy Symptoms
Common symptoms of muscular dystrophy include:
-
Trouble running, jumping, climbing stairs, or standing up from a sitting position.
-
Unexplained tripping or loss of balance.
-
Although weakness is the primary issue, some individuals experience muscle pain and stiffness.
-
An unstable and slow walking gait
-
Calf muscles appear larger (pseudohypertrophy) due to fat and connective tissue replacing muscle, rather than true muscle growth.
-
Persistent tiredness, even after rest.
-
Learning problems are present in some `muscular dystrophy types`, such as DMD, due to effects on the brain.
-
Noticeable decline in strength in specific muscle groups over time.
-
Struggling to raise arms above the head.
-
Problems with swallowing or breathing is often seen in advanced stages
Causes of Muscle Weakness
Genetic mutations are one of the main causes of muscle weakness. These mutations disrupt the protein production essential for healthy muscle structure and function. Without these proteins, muscle fibers are damaged and eventually replaced by fat and connective tissue, leading to progressive weakness:
-
Specific gene mutations lead to the absence or malfunction of proteins like dystrophin, which is vital for maintaining the integrity of muscle cells.
-
These genetic mutations causing muscle weakness are also passed on from one generation to the next through autosomal dominant, autosomal recessive, or X-linked (most common for DMD and BMD) patterns.
Genetic counselling and early diagnostic testing can identify specific genetic mutations, which can then provide families with critical information for navigating the condition.
Muscular Dystrophy Treatment and Management
While there is currently no cure for the different types of muscular dystrophy, the treatment focuses on managing symptoms, slowing progression, and improving the patient's quality of life. Some of the common therapeutic approaches include:
-
Physical Therapy: Essential for maintaining muscle flexibility, strength, and range of motion, and preventing contractures.
-
Occupational Therapy: Helps individuals adapt to daily activities, providing strategies and assistive devices to maintain independence.
-
Speech Therapy: Addresses difficulties with swallowing (dysphagia) and communication.
-
Respiratory Care: Monitoring and support, including breathing exercises and assistive ventilation, are crucial as respiratory muscles weaken.
-
Cardiac Monitoring: Regular checks and management of heart health are needed to track the progression of the condition.
-
Medications: Certain prescribed medications can help slow disease progression in some forms.
-
Nutritional Counselling: To maintain a healthy weight and ensure adequate nutrient intake to support overall health and energy levels.
-
Surgical Interventions: May be recommended for managing complications such as scoliosis or severe contractures, aiming to improve function and reduce pain.
Conclusion
If you or a loved one are experiencing `muscular dystrophy symptoms` or any form of progressive muscle weakness, prompt medical evaluation is crucial. At Manipal Hospitals, Goa, our experts at the Department of Neurology provide early diagnostic services and clinical support for managing muscle weakness, aiming to help you handle daily activities more effectively.
FAQ's
General muscle weakness can be temporary or acute due to various factors like illness, injury, or fatigue. Progressive muscle weakness, however, implies a gradual, ongoing, and often irreversible decline in muscle strength over time, typically characteristic of chronic conditions like muscular dystrophy.
For many underlying conditions causing progressive muscle weakness, such as muscular dystrophy, there is currently no cure. However, comprehensive muscular dystrophy treatment focuses on managing symptoms, slowing disease progression, and providing functional independence.
Diagnosis typically involves a thorough physical examination, review of muscular dystrophy symptoms and family history, blood tests (e.g., creatine kinase levels), electromyography (EMG), nerve conduction studies, muscle biopsy, and definitive genetic testing to identify specific mutations to identify the causes of muscular dystrophy.
Most forms of muscular dystrophy are indeed genetic and inherited, meaning they are passed down through families. However, some cases can arise from new, spontaneous gene mutations not inherited from either parent.
Treatment for muscular dystrophy is multidisciplinary and highly individualised. Key components include physical and occupational therapy, respiratory care, cardiac monitoring, nutritional support, assistive devices, and specific medications to manage symptoms and complications.





















 5 Min Read
5 Min Read