
Bringing a new life into the world is usually a time of excitement and careful planning. But when a baby arrives earlier than expected, sometimes weeks or even months before the due date, it can feel overwhelming and frightening for parents. You may wonder what went wrong, whether your baby will be healthy, and what the coming days or weeks will look like inside a hospital. This experience is known as premature birth, and it is more common than many people realise. While it is natural to feel anxious, it is important to remember that neonatal medicine has advanced remarkably. Today, the majority of babies born early go on to lead healthy, full lives.
This blog will walk you through the realities of early delivery, from recognising the first physical warning signs to understanding the sophisticated medical support systems available in modern hospitals. By learning about the triggers and the long-term care strategies, you can better navigate the complexities of a premature birth with clarity and hope.
Synopsis
- Understanding the Timeline: What is Premature Birth?
- Recognising the Early Warning Signs
- Identifying the Primary Triggers of Early Delivery
- Categorising Degrees of Prematurity
- Understanding the Risks and Short-Term Complications
- Long-Term Health and Developmental Considerations
- The Role of Modern Medical Treatment
- Practical Steps for Parents During a NICU Stay
- Conclusion
Understanding the Timeline: What is Premature Birth?
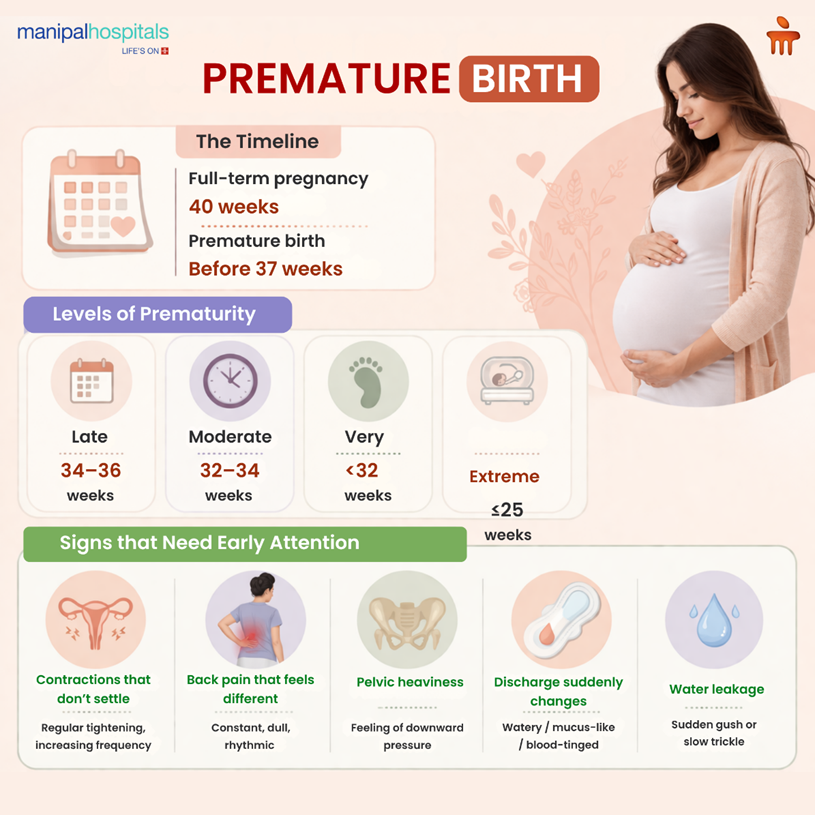
To understand the medical approach to early delivery, we must first define the parameters used by healthcare professionals. When a person asks, 'What is premature birth?' they are essentially asking about the completion of the developmental window. A standard pregnancy lasts about 40 weeks. A birth is considered premature if it occurs before 37 weeks of pregnancy are completed.
Because the final weeks of pregnancy are crucial for the development of vital organs, specifically the lungs, brain, and liver, babies born during this time are categorised based on how early they arrive.
-
Late preterm: Born between 34 and 36 completed weeks of pregnancy.
-
Moderately preterm: Born between 32 and 34 weeks of pregnancy.
-
Very preterm: Born at less than 32 weeks of pregnancy.
-
Extremely preterm: Born at or before 25 weeks of pregnancy.
Understanding premature birth in this tiered context helps doctors determine the level of intervention needed. The closer a baby is to the 40-week mark, the lower the likelihood of serious health complications.
Recognising the Early Warning Signs
Many people believe that labour is always an obvious, dramatic event involving intense pain. In reality, early labour can be subtle and easily mistaken for the general discomforts of the third trimester. Being able to identify premature labour signs and symptoms is the first step in potentially stopping or delaying the delivery to give the baby more time to grow.
If you experience any of the following, it is essential to contact your obstetrician immediately:
-
Consistent Contractions: This feels like a regular tightening of the abdomen. Unlike "false labour" (Braxton Hicks), these contractions do not go away when you change positions or rest; they become more frequent and rhythmic.
-
Persistent Dull Backache: A new or different type of low backache that is constant or rhythmic can be a sign that the body is preparing for delivery.
-
Pelvic Pressure: Feeling as though the baby is pushing down or a heavy sensation in the pelvic region can indicate that the cervix is starting to thin or open.
-
Changes in Vaginal Discharge: Any sudden increase in discharge, or discharge that becomes watery, mucus-like, or tinged with blood, requires medical evaluation.
-
Rupture of Membranes: Often referred to as ‘water breaking,' this event can be a sudden gush or a continuous trickle of fluid.
Ignoring these premature labour signs and symptoms can lead to a delivery occurring before the hospital can administer protective medications, such as steroids, to help the baby's lungs mature.
Identifying the Primary Triggers of Early Delivery
Medical science is still exploring the full range of reasons why a pregnancy might end early. In many cases, a premature birth occurs spontaneously without a single, clear trigger. However, researchers have identified several factors that significantly increase the likelihood of an early arrival.
When exploring what is the most common cause of premature birth is, we often find that a previous history of early delivery is the strongest predictor. If a mother has delivered early before, the risk of it happening again is higher. However, other biological and lifestyle factors play a role:
-
Infections: Certain infections, particularly those involving the urinary tract or the amniotic membranes, can trigger a hormonal response that starts labour.
-
Multiple Gestations: Carrying twins, triplets, or more puts physical strain on the uterus and often leads to early delivery.
-
Chronic Health Conditions: High blood pressure (preeclampsia), diabetes, and blood-clotting disorders can create an environment where the body decides it is safer for the baby to be delivered than to remain in the womb.
-
Placental Issues: Problems such as placenta previa or placental abruption can interfere with the baby’s oxygen and nutrient supply, necessitating an early birth.
Categorising Degrees of Prematurity
The following table outlines how different stages of prematurity typically affect the newborn's immediate needs and the medical focus of the care team:
|
Stage of Prematurity |
Gestational Age |
Common Physical Characteristics |
Primary Medical Focus |
|
Late Preterm |
34 to 36 weeks |
Looks like a small full-term baby; may have trouble staying warm. |
Monitoring feeding, breathing, and jaundice levels. |
|
Moderately Preterm |
32 to 34 weeks |
Thin skin; very little body fat; weak suckling reflex. |
Respiratory support and temperature regulation. |
|
Very Preterm |
Under 32 weeks |
Transparent skin; eyes may be fused shut initially; very fragile. |
Intensive respiratory care; IV nutrition; infection prevention. |
|
Extremely Preterm |
25 weeks or less |
Extremely small; organs are significantly underdeveloped. |
Critical life support; long-term NICU stay; multisystem monitoring. |
Understanding the Risks and Short-Term Complications
A baby develops according to a very specific timeline. When that timeline is interrupted, some organs may not yet be ready to work on their own. Understanding what are the risks of premature birth can help parents make sense of the machines, monitors, and tests they see in the Neonatal Intensive Care Unit (NICU).
Short-term complications often include:
-
Respiratory distress syndrome: Premature babies may struggle to breathe because their lungs have not produced enough surfactant, which helps keep the air sacs open.
-
Heart problems: One common issue is a persistent ductus arteriosus (PDA), where a blood vessel that should close after birth stays open for longer than expected.
-
Temperature regulation problems: Preterm babies often have very little body fat and may not be able to maintain their temperature without help, which is why incubators are crucial.
-
Digestive difficulties: The digestive system may still be immature, making feeding harder and sometimes increasing the risk of necrotising enterocolitis (NEC).
These complications can sound frightening, but they are also familiar to NICU teams. Early recognition and close monitoring make a major difference in outcomes.
Long-Term Health and Developmental Considerations
As the baby grows and leaves the hospital, attention gradually shifts from immediate survival to long-term development. Many premature babies grow and develop well, but some may need ongoing support as they get older.
Possible long-term concerns include:
-
Vision and hearing: Premature infants may have a higher risk of retinopathy of prematurity, which affects blood vessel development in the eyes. Hearing assessments are also important.
-
Neurological development: Some children born very early may later face conditions such as cerebral palsy or learning difficulties.
-
Behavioural concerns: Research shows that some children born prematurely may have a higher chance of ADHD or anxiety later in life.
-
Growth tracking: Doctors often use corrected age rather than birth age to assess milestones, since premature babies follow a different growth pattern.
Not very premature baby will have long-term complications, but regular follow-up helps doctors spot concerns early and support development in a timely way.
The Role of Modern Medical Treatment
Treatment for early delivery may begin even before birth. If a mother is at risk for premature birth, doctors may give corticosteroids to help the baby’s lungs mature faster. Magnesium sulfate may be used in certain circumstances to help shield the infant's brain.
After birth, the NICU becomes the centre of care. Treatment may include:
-
Ventilation support: This may range from supplemental oxygen to a ventilator that assists with breathing.
-
Nutritional support: Babies may receive nutrition through an IV or a feeding tube until they are strong enough to feed normally.
-
Controlled environment: Incubators help maintain the right temperature and humidity while also reducing exposure to noise and bright lights.
This kind of care is designed to support the baby while the body continues to mature.
Practical Steps for Parents During a NICU Stay
A hospital stay after an early delivery can feel long and emotionally demanding. There are often many small ups and downs along the way, and parents may feel unsure about what they can do to help.
A few helpful steps include:
-
Ask questions: If something is unclear, ask the team to explain it. Understanding the purpose of a medicine or monitor often reduces stress.
-
Prioritise self-care: Eating regularly, resting when possible, and taking breaks are important.
-
Focus on bonding: If holding the baby is not yet possible, talking, singing, or spending quiet time nearby can still help create connection.
-
Seek support: Many hospitals offer NICU parent support groups, and speaking with other families can be reassuring.
Conclusion
A premature birth is rarely expected, and it can be one of the most difficult experiences a family goes through. Still, early recognition, specialised care, and a well-equipped NICU give these babies a strong chance to grow and improve. By understanding the causes, learning the warning signs, and accessing specialised premature birth care in Bangalore, families can feel more prepared and supported. At Manipal Hospitals, care is designed to help both the baby and the family through each stage of this journey.
FAQ's
Sometimes, yes. If premature labor signs and symptoms are noticed early, doctors may use medicines called tocolytics to delay delivery for a short time. That delay can allow steroids to work and improve the baby’s lung development.
Usually, yes, because they miss the final weeks of growth in the womb. Many babies born early catch up over time, often by the age of two or three.
Medical care matters greatly, but breast milk and skin-to-skin contact are also essential. Breast milk offers protective antibodies, and skin-to-skin contact can help stabilise breathing and heart rate.
Most babies go home once they can breathe without support, keep their body temperature steady in an open crib, and take all feeds by mouth. This often happens close to the original due date.
Some causes cannot be prevented, but regular prenatal visits, control of conditions like diabetes or high blood pressure, and avoiding smoking and alcohol can lower the risk. Good follow-up is an important part of premature birth prevention.






















 8 Min Read
8 Min Read













