A slight tremor in the hand, slowness while buttoning a shirt, or stiffness that doesn’t quite feel like ordinary ageing. For many people, these small changes quietly build anxiety long before a diagnosis is ever made. Parkinson’s disease is often misunderstood, and the uncertainty surrounding it can feel overwhelming.
Parkinson’s disease is a progressive neurological condition that affects movement, balance, and several non-motor functions. It develops gradually, and its symptoms vary from person to person. In this blog, we provide expert clinical insights from a top neurologist in Yeshwanthpur on what Parkinson’s disease means, how and why it develops, the full spectrum of Parkinson's disease symptoms, the science behind its progression, available Parkinson's disease treatment approaches, and how long-term care is structured to maintain quality of life.
Synopsis
- What is Parkinson’s disease?
- The Early and Progressive Symptoms
- Parkinson’s Disease Causes: Why Does It Happen?
- The Pathophysiology of Parkinson’s Disease
- How is Parkinson’s Disease Diagnosed?
- Parkinson’s Disease Treatment: A Structured Approach
- Stages of Parkinson’s Disease
- Living Well with Parkinson’s Disease
- Conclusion
What is Parkinson’s disease?
When people first hear the diagnosis, they often ask, "What is Parkinson’s disease?” in easy terms. At its core, Parkinson's disease is a progressive brain disorder that mainly affects movement due to the loss of dopamine-producing cells in an area called the substantia nigra. As dopamine levels fall, movements become slower, stiffer, and less automatic. The Parkinson's disease meaning, therefore, is not simply tremor; it reflects a complex neurological process affecting multiple body systems over time.
The Early and Progressive Symptoms
Symptoms often begin subtly. Many patients recall changes months or even years before seeking medical advice. Recognising early Parkinson's disease symptoms can allow for earlier intervention and better long-term planning.
Motor Symptoms
The hallmark symptoms related to motor functions include:
-
Resting tremor, often starting in one hand
-
Slowness of movement (bradykinesia)
-
Muscle rigidity
-
Postural instability in later stages
Tremor typically appears when the limb is at rest and may reduce during purposeful activity. Slowness is often more disabling than tremor, making everyday tasks such as writing or walking increasingly effortful.
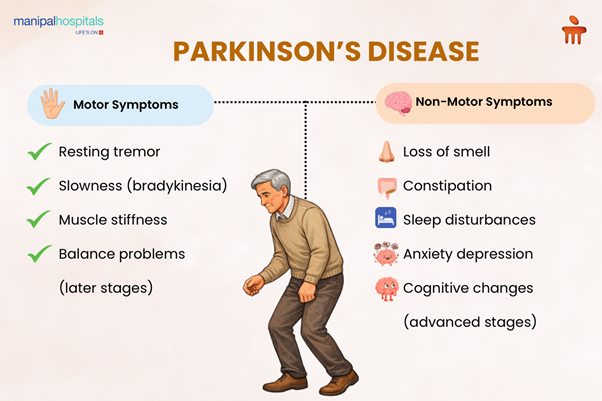
Non-Motor Symptoms
Less visible but equally important are the following non-motor symptoms:
-
Reduced sense of smell
-
Sleep disturbances
-
Mood changes such as anxiety or depression
-
Cognitive changes in advanced stages
These symptoms may precede movement changes and significantly affect well-being. Parkinson’s disease is therefore not purely a movement disorder; it is a whole-body neurological condition.
Parkinson’s Disease Causes: Why Does It Happen?
Understanding Parkinson's disease causes requires looking at a combination of biological vulnerability and environmental influences. In most cases, there is no single identifiable trigger. Key contributing factors include:
-
Ageing: Risk increases after 60 years.
-
Genes: Genetic mutations in specific genes (such as LRRK2 or PARK genes).
-
Environment: Environmental toxin exposure, particularly certain pesticides.
-
Brain Function: Oxidative stress and mitochondrial dysfunction within brain cells.
Most individuals diagnosed with Parkinson’s disease do not have a strong family history. The condition is typically sporadic, arising from a complex interaction between genes and environment rather than one direct cause.
The Pathophysiology of Parkinson’s Disease
To truly understand progression, one must explore the pathophysiology of Parkinson's disease. This refers to the biological processes occurring inside the brain.
At a microscopic level, abnormal protein deposits known as Lewy bodies accumulate within neurons. These contain alpha-synuclein, a protein that becomes misfolded and toxic. As dopamine-producing cells gradually die, communication between brain regions responsible for movement becomes impaired.
Interestingly, dopamine loss begins long before visible symptoms appear. By the time classic motor signs develop, nearly 50–60% of dopamine neurons may already be lost. This finding explains why Parkinson’s disease is progressive and why early non-motor symptoms can precede diagnosis by years.
How is Parkinson’s Disease Diagnosed?
Diagnosis remains primarily clinical. There is no single blood test or scan that confirms Parkinson’s disease with certainty. Instead, neurologists rely on:
-
Detailed symptom history
-
Neurological examination
-
Observation of response to dopamine-based medication
Imaging, such as an MRI, is usually performed to rule out other conditions rather than confirm Parkinson’s disease itself. Specialised scans like DAT-SPECT may be used in uncertain cases, but they are not routine for every patient.
Early and accurate diagnosis is crucial because treatment strategies differ significantly between various movement disorders.
Parkinson’s Disease Treatment: A Structured Approach
There is currently no cure for Parkinson’s disease, but Parkinson's disease treatment is highly effective in controlling symptoms and preserving independence for many years. Treatment plans are individualised and evolve as the condition progresses.
1. Medication Therapy
The cornerstone of treatment is levodopa, which converts into dopamine in the brain. Other medication classes include:
-
Dopamine agonists
-
MAO-B inhibitors
-
COMT inhibitors
-
Amantadine
Each medication works differently, and combinations are often required over time. Dose adjustments are carefully balanced to avoid side effects such as dyskinesias (involuntary movements).
2. Advanced Therapies
When medications alone become insufficient, advanced interventions may be considered:
-
Deep brain stimulation (DBS)
-
Levodopa-carbidopa intestinal gel infusion
-
Continuous apomorphine infusion
These therapies aim to smooth motor fluctuations and improve daily function in carefully selected patients.
3. Multidisciplinary Support
Long-term management involves:
-
Physiotherapy for gait and balance
-
Speech therapy for voice and swallowing changes
-
Occupational therapy to assist with daily activities
-
Psychological counselling
Effective Parkinson's disease treatment is never limited to tablets alone; it is a coordinated care strategy.
Stages of Parkinson’s Disease
Progression varies widely. The following table outlines recognised clinical stages and associated functional changes:
|
Stage |
Functional Characteristics |
Mobility Status |
Independence Level |
|
Stage 1 |
Symptoms affect one side of the body only |
Independent walking |
Fully independent |
|
Stage 2 |
Bilateral involvement without balance loss |
Slight gait slowing |
Independent but slower |
|
Stage 3 |
Balance impairment begins |
Increased fall risk |
Independent with caution |
|
Stage 4 |
Severe motor symptoms |
Requires assistance for walking |
Limited independence |
|
Stage 5 |
Wheelchair-bound or bedridden |
Unable to stand unaided |
Dependent on caregiver |
It is essential to note that while this is the standard progression of the disease, not every patient progresses through all stages. Additionally, the timelines of each stage may differ significantly between individuals, owing to unique health factors.
Living Well with Parkinson’s Disease
A diagnosis changes routines, but it does not remove purpose or possibility. Structured exercise has been shown to improve mobility and may even slow functional decline. Activities such as brisk walking, cycling, yoga, and strength training are strongly encouraged.
Nutrition also plays a role. Adequate fibre helps manage constipation, while protein timing may improve levodopa absorption. Emotional health deserves equal attention. Depression and anxiety are common but treatable components of Parkinson’s disease.
Caregiver education is another pillar of effective management. Families who understand the condition are better equipped to provide support while preserving dignity and independence.
Conclusion
Parkinson’s disease is a progressive neurological disorder rooted in dopamine depletion and complex brain changes. While it cannot yet be cured, timely diagnosis and structured Parkinson's disease treatment significantly improve function, comfort, and quality of life. With medical therapy, advanced interventions, rehabilitation, and emotional support, many individuals live active and meaningful lives for decades after diagnosis. For those seeking specialised Parkinson’s disease treatment options in Yeshwanthpur, multidisciplinary neurological care at Manipal Hospitals Yeshwanthpur ensures comprehensive evaluation and personalised long-term planning.
FAQ's
Yes. Parkinson’s disease can alter pain perception, and some patients may experience increased sensitivity to pain or changes in temperature perception. These symptoms occur because Parkinson’s disease affects not only dopamine pathways but also other neurotransmitter systems involved in sensory processing and pain modulation
Not all individuals develop dementia. Cognitive decline occurs in a subset, particularly in advanced stages, and varies widely. Early cognitive screening allows for proactive planning and management.
Handwriting often becomes smaller and cramped, a phenomenon called micrographia. With therapy and medication adjustments, some improvement can be achieved, though changes may persist.
Currently, no supplement has been conclusively proven to slow disease progression. Patients should consult their neurologist before starting antioxidants, herbal remedies, or alternative therapies.
Yes. Early-onset Parkinson’s disease occurs before the age of 50. It often has a stronger genetic component and may progress differently compared to later-onset forms.





















 7 Min Read
7 Min Read





.png)