Cervical cancer is one of the most common forms of cancer in women across the world, and it is caused due to infection from the human papillomavirus (HPV). HPV vaccine is one of the most effective ways to prevent cervical cancer, as well as other cancers caused by HPV, and early detection can significantly improve treatment outcomes. This blog talks about some of the most common cervical cancer symptoms to watch out for, while also highlighting the importance of vaccination and screenings.
Synopsis
Understanding Cervical Cancer
Understanding cervical cancer is an important step towards recognising cervical cancer symptoms.
Cervical cancer is caused by infection from Human Papillomavirus (HPV), which is typically transmitted from unprotected sexual contact. Normally, HPV infections develop slowly and are cleared out by body’s immune system. However, repeated infections of the pelvic floor from oncogenic HPV variants can cause cervical cancer. This disease progresses slowly, so symptoms may be undetected for a long time. Thus, regular cervical cancer screening, especially after a certain age, is essential for early detection of symptoms.
Top 10 Cervical Cancer Symptoms to Watch For
These warning signs could also be signs of other conditions; however, it is always advised to get them evaluated:
1. Abnormal Vaginal Bleeding
Abnormal vaginal bleeding is one of the most common and significant cervical cancer symptoms. It can manifest as:
-
Bleeding between periods (intermenstrual bleeding).
-
Bleeding after sexual intercourse (post-coital bleeding).
-
Bleeding after menopause.
-
Heavier or longer menstrual periods than usual.
Any unexpected bleeding should be promptly investigated.
2. Unusual Vaginal Discharge
Changes in vaginal discharge can be an early indicator. While many factors can cause changes in discharge, a persistent, abnormal discharge should not be ignored. Look for discharge that is:
-
Watery, pink, brown, or bloody.
-
Foul-smelling.
-
Unusually heavy or persistent.
3. Pelvic Pain
Pelvic pain, particularly during or after intercourse, can be a symptom. It may manifest as a dull ache or pressure.
4. Pain during Intercourse (Dyspareunia)
Experiencing pain or discomfort during sexual activity is often experienced by women, and several factors could be responsible for it. However, it can also be a symptom of cervical cancer. Dyspareunia can range from mild discomfort to sharp pain.
5. Changes in Menstrual Cycle
Several factors can be responsible for changes in menstrual cycle. An unexplained change in your menstrual cycle, such as significantly longer, heavier, or more painful periods must be evaluated urgently.
6. Unexplained Weight Loss
Like many cancers, unexplained and unintentional weight loss (losing a significant amount of weight without trying) can be a general symptom of advanced disease.
7. Fatigue
Persistent, overwhelming fatigue not relieved by rest can be a symptom, often related to the body fighting cancer or blood loss.
8. Swelling in Legs
If cervical cancer spreads, it can affect the lymph nodes or press on nerves and blood vessels, leading to swelling in one or both legs (lymphedema).
9. Urinary Problems
Advanced cervical cancer can affect the bladder, leading to symptoms such as:
-
Pain or discomfort during urination.
-
Blood in the urine (haematuria).
10. Bowel Changes
Similar to urinary issues, if the cancer spreads to the bowel, symptoms might include:
-
Pain during bowel movements.
-
Rectal bleeding.
-
Constipation or diarrhea.
The Power of Prevention and Early Detection
Cervical cancer is largely preventable and highly curable with early detection.
-
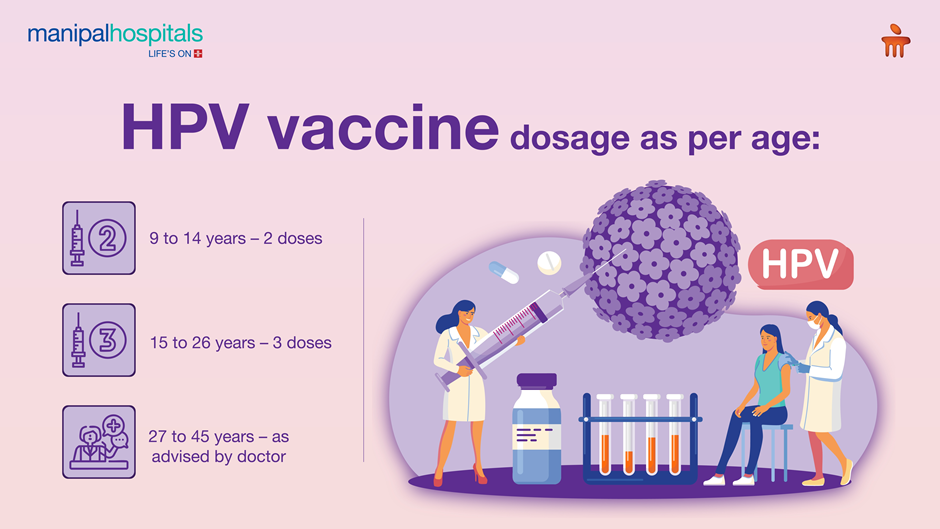
HPV Vaccination: The HPV vaccine is vital for prevention, protecting against common cancer-causing HPV types. It is highly effective in preventing HPV infections and related cancers. It is most effective when taken between ages 9 to 12 years. Those between ages 9 to 14 years of age should get 2 doses of the vaccine, and those aging between 15-26 years will need 3 doses. HPV vaccine can be taken up to 45 years of age if approved by your doctor.
-
Cervical Cancer Screening: Regular cervical cancer screening, including Pap smear and HPV tests, is crucial. A Pap smear detects precancerous cells, enabling early intervention and preventing progression to invasive cancer in nearly 100% of cases. Screenings have dramatically reduced cervical cancer deaths due to early detection of cervical cancer.
Care Essentials: Do's and Don'ts
Do's:
-
Do schedule regular cervical cancer screening. It is the most effective way to detect changes early.
-
Do get the HPV vaccine as medically recommended.
-
Do pay attention to your body and new cervical cancer symptoms.
-
Do maintain open communication with your healthcare provider about sexual health.
-
Do practice safe sex to reduce HPV risk.
Don'ts:
-
Don't ignore abnormal vaginal bleeding or discharge. These are critical signs that require medical attention.
-
Don't skip your routine Pap smears or HPV tests; they are your best defence.
-
Don't self-diagnose based on information found online. Always consult a medical professional.
-
Don't delay seeking medical advice if you experience persistent symptoms, even if they seem mild.
Conclusion
Knowledge about cervical cancer symptoms is key to proactive health. Early detection significantly increases treatment success. If you are experience symptoms or have cervical health concerns, seek timely medical advice. Book an appointment with our expert gynaecologist and oncologist at Manipal Hospitals Salt Lake for comprehensive care.
FAQ's
Almost all cervical cancers are caused by persistent infection with certain high-risk types of the human papillomavirus (HPV), a very common sexually transmitted infection.
Any woman who has been exposed to HPV is at risk. Other risk factors include multiple sexual partners, early age at first intercourse, a weakened immune system, and smoking.
Generally, women aged 21-65 need regular screenings. Your doctor will advise the best schedule.
Yes, cervical cancer is highly curable, especially when detected at an early stage. When diagnosed in its localized stage, the 5-year survival rate can be as high as 92%.
You should see a doctor immediately if you experience any abnormal vaginal bleeding (after sex, between periods, or after menopause), unusual vaginal discharge, or persistent pelvic pain.





















 5 Min Read
5 Min Read