What if numb toes, a burning sensation in the feet, or sudden dizziness were early clues that nerves are being affected by blood sugar? Diabetic neuropathy is a common complication of diabetes that quietly harms nerves over months to years. Early recognition of diabetic neuropathy symptoms, timely testing, and targeted care slow progression and reduce complications such as foot ulcers and falls. This article explains what diabetic neuropathy is, what typically causes it, the early warning signs to look for, how it is diagnosed, and realistic options for diabetic neuropathy treatment and ongoing care, including how to access diabetic neuropathy care in Millers Road, Bangalore.
Synopsis
- What is Diabetic Neuropathy?
- Types of Diabetic Neuropathy
- What Causes Nerve Damage in Diabetes?
- Early Warning Signs: What to Watch For
- How Is Diabetic Neuropathy Diagnosed?
- Can Diabetic Neuropathy Be Reversed?
- Diabetic Neuropathy Treatment: What Works Now
- Living With Diabetic Neuropathy: Practical Care Steps
- Conclusion
What is Diabetic Neuropathy?
At its simplest, diabetic neuropathy describes nerve damage caused by long-term high blood sugar and related metabolic changes. Nerves carry messages between the brain and the body for sensation, movement, and the control of internal organs. When these nerves are injured, signals become distorted: numbness, burning, weakness, or autonomic problems (like dizziness on standing or digestive changes) can follow. The condition often develops slowly and may affect different nerve groups, so patterns of symptoms vary between people.
Types of Diabetic Neuropathy
Diabetic neuropathy does not affect everyone in the same way. The symptoms depend on which group of nerves is damaged. Doctors classify neuropathy into different types based on the nerves involved.
Recognising the type helps shape diabetic neuropathy treatment.
-
Peripheral neuropathy (the common form): affects feet and hands, causing numbness, burning, tingling, and loss of protective sensation.
-
Autonomic neuropathy: affects internal controls, heart rate, blood pressure, digestion, bladder, and sexual function.
-
Proximal (amyotrophic) neuropathy: causes thigh and hip weakness, more common in older adults with type 2 diabetes.
-
Focal neuropathies: sudden single-nerve palsies causing wrist drop, double vision, or localized pain.
Most people first notice peripheral symptoms in the toes and feet; that common pattern is why foot checks and foot care for diabetic neuropathy are central to care. Some people may experience more than one type of neuropathy at the same time.
What Causes Nerve Damage in Diabetes?
High blood sugar affects the body in several ways. Over time, it can interfere with blood supply to nerves and disrupt how they function and repair themselves. Several mechanisms contribute to nerve injury in diabetes:
-
Chronic hyperglycemia damages small blood vessels that supply nerves and alters nerve metabolism.
-
High blood lipids, inflammation, and oxidative stress further injure nerve fibers.
-
Duration of diabetes: longer exposure to high glucose increases risk.
-
Other factors, such as kidney disease, smoking, high blood pressure, and vitamin deficiencies, can increase vulnerability.
Addressing these drivers, most importantly, blood sugar and blood pressure control, is the cornerstone of how to improve diabetic neuropathy outcomes.
Early Warning Signs: What to Watch For
Early recognition of diabetic neuropathy symptoms matters because treatment works best before extensive nerve loss. Common early signs include:
|
Symptom |
Likely Concern |
When To Seek Medical Help |
|
Mild tingling in toes |
Early peripheral neuropathy |
Book a diabetes review within 2 weeks |
|
Numbness or loss of feeling |
Loss of protective sensation |
Urgent assessment; foot care advice same week |
|
Sharp, burning night pain |
Painful diabetic neuropathy |
Discuss pain management promptly |
|
Dizziness on standing |
Autonomic neuropathy (BP changes) |
Seek advice within a few days |
|
Foot ulcer or blister |
Skin breakdown from a numb foot |
Immediate medical attention to prevent infection |
|
New bladder or digestive problems |
Autonomic involvement |
Early review to tailor treatment |
If any of these appear, simple tests can show whether nerves are affected and how severely.
How Is Diabetic Neuropathy Diagnosed?
Diagnosing diabetic neuropathy involves simple physical examinations combined with specialised tests when necessary. Diagnosis blends clinical checks and focused tests:
-
Clinical history and exam: sensory testing (monofilament, tuning fork), muscle strength checks, and reflexes.
-
Simple bedside tests: 10 g monofilament for protective sensation and vibration with a 128 Hz tuning fork.
-
Nerve conduction studies/EMG: assess large-fiber function and rule out other causes.
-
Autonomic testing: heart rate variability, tilt-table, or gastric emptying tests when autonomic symptoms exist.
-
Blood tests: to check glucose control (HbA1c), vitamin B12, thyroid, and kidney function.
A structured approach ensures the right problem is treated, and other causes of neuropathy are excluded.
Can Diabetic Neuropathy Be Reversed?
The question can diabetic neuropathy be reversed is common and important. Realistically:
-
Early nerve dysfunction (small-fiber symptoms, mild sensory change) can improve with strict glucose control and risk-factor management. Some patients report significant symptom reduction.
-
Established nerve loss (complete numbness, long-standing deficits) generally cannot be fully reversed, though progression often slows, and symptoms can be managed.
-
Painful neuropathy can be treated effectively, and pain reduction and improved sleep are achievable even if full nerve recovery is limited.
Early detection and sustained control of blood sugar, lipids, and blood pressure give the best chance that nerves recover function or at least stop worsening.
Diabetic Neuropathy Treatment: What Works Now
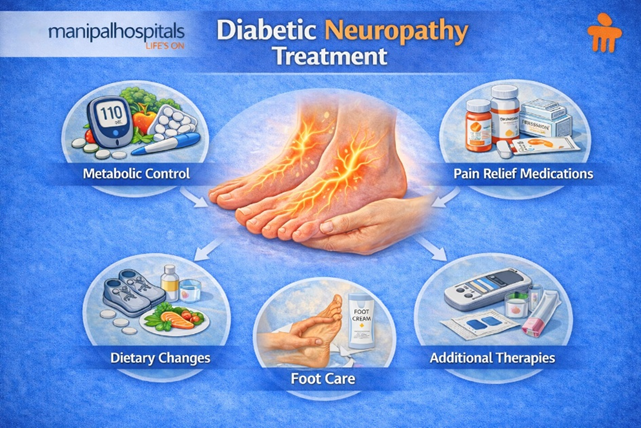
Diabetic neuropathy treatment aims to slow progression, relieve symptoms, and prevent complications. Key elements:
1. Metabolic control
-
Optimising HbA1c and protecting kidneys and blood pressure are foundational. Better control reduces new nerve damage.
2. Symptom relief for painful neuropathy
-
First-line drugs: duloxetine or pregabalin (or gabapentin) for neuropathic pain.
-
Older options: certain tricyclic antidepressants at low doses (with caution for heart issues).
-
Topical options: capsaicin or lidocaine patches for localized pain.
-
Non-drug measures: TENS, cognitive behavioural approaches, and graded exercise support pain control.
3. Foot protection and wound prevention
-
Regular foot exams, daily self-checks, proper footwear, and prompt treatment of cuts or blisters prevent ulcers and amputations.
4. Autonomic symptom management
-
Orthostatic hypotension, gastroparesis, or bladder dysfunction have specific treatments, from dietary changes to medications, tailored to the problem.
5. Emerging therapies and referral
-
Referral to pain specialists, neurology, or specialised diabetic foot clinics helps when symptoms are severe or refractory. For complex cases, device-based neuromodulation may be considered.
Combining metabolic, symptomatic, and preventive strategies forms effective diabetic neuropathy treatment plans.
To know More about diabetic neuropathy Click Here
Living With Diabetic Neuropathy: Practical Care Steps
Simple everyday steps reduce risk and improve life quality:
-
Check feet daily and keep skin moisturised (but not between toes).
-
Wear cushioned, well-fitting shoes, and avoid walking barefoot.
-
Keep blood sugar and blood pressure targets within agreed ranges.
-
Stop smoking and limit alcohol, both of which worsen nerve damage.
-
Keep active with balance and strength exercises to lower fall risk.
-
Inform the healthcare team about new numbness, pain, or wounds promptly.
These habits are central to long-term diabetic neuropathy care. For those searching for diabetic neuropathy care in Millers Road, Bangalore, choose a centre that offers structured foot clinics, pain management services, and regular screening programmes so problems are spotted early and treated comprehensively.
Conclusion
Diabetic neuropathy is common but not inevitable; early detection, strong blood sugar control, and sensible foot care change outcomes. A clear plan, screening, metabolic optimisation, pain management, and preventive foot strategies keep nerves healthier and life more active. For expert assessment and coordinated diabetic neuropathy care, contact Manipal Hospitals, Millers Road.
FAQ's
Nerve changes can begin within a few years of diabetes onset, and sometimes even before diabetes is diagnosed; regular screening is important.
Any foot ulcer, new blister, loss of protective sensation, or fainting/dizziness on standing requires prompt medical attention.
Improving blood sugar slows progression and can reduce some symptoms, but pain relief often also needs specific neuropathic pain medication.
Regular exercise, good sleep, and vitamin repletion when indicated support nerve health. Avoid unproven supplements without discussing them first.
At least annually for everyone with diabetes; those with numbness, prior ulcers, or high risk need checks every 3–6 months or as advised.





















 7 Min Read
7 Min Read