Osteoporosis is a skeletal disorder where bones become weak and brittle due to decreased bone mineral density (BMD), making them susceptible to fractures even from minor falls or stresses. Fractures, particularly in the hip, spine, and wrist, can lead to pain, disability, and reduced mobility. Globally, it's estimated that 1 in 3 women and 1 in 5 men over the age of 50 will experience an osteoporotic fracture. With early diagnosis and a tailored treatment plan, the risk of debilitating fractures can be significantly reduced to a great extent, allowing many patients to regain independence and strength. This blog serves as a handbook for identifying osteoporosis symptoms, understanding the condition and managing it in the best possible way.
Synopsis
What causes osteoporosis?
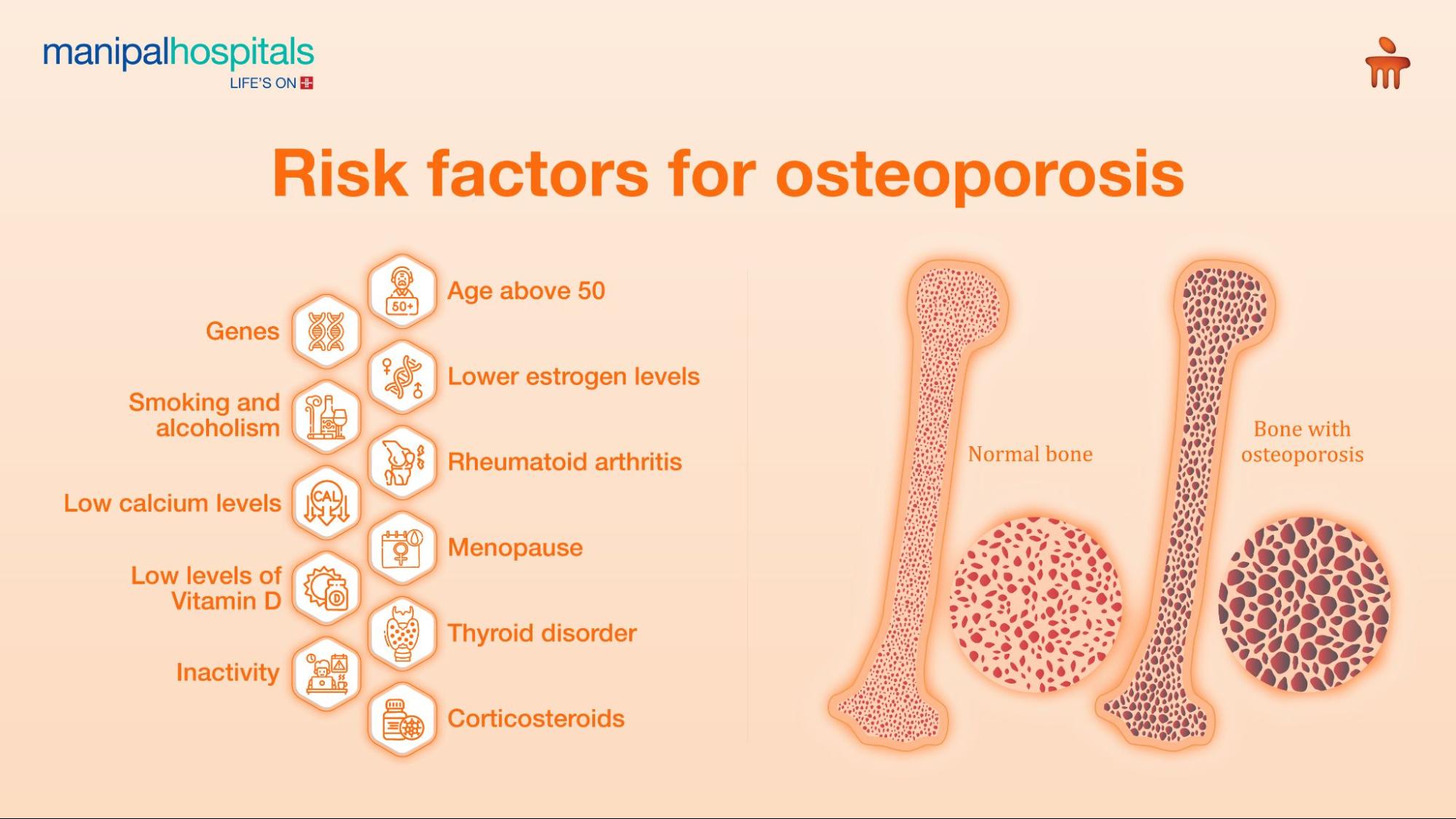
Osteoporosis often progresses slowly but has the potential to significantly impact the quality of life. It is characterised by a reduced bone density and quality, leading to weakened bones. It often exhibits no symptoms until a fracture occurs, earning it the tag of a ‘silent disease’. Understanding the causes is the first step towards effective osteoporosis treatment.
Age
With age, the natural process of bone breakdown begins to exceed bone formation. This gradual loss of bone density makes them fragile, thus increasing the risk of osteoporosis and fractures.
Hormonal changes
A sharp decline in estrogen levels after menopause accelerates bone loss in women. Since estrogen helps maintain bone density, its reduction significantly increases the risk of osteoporosis.
Certain medical conditions
Chronic illnesses such as thyroid disorders, rheumatoid arthritis, and gastrointestinal diseases can interfere with calcium absorption or bone metabolism, thereby weakening bones and contributing to osteoporosis.
Medications
Long-term use of certain drugs, like corticosteroids, anti-seizure medications, and hormonal medicines, can reduce bone formation or increase bone loss, and raise the risk of osteoporosis.
Genetics
Genetic factors influence bone mass, bone structure, and how the body regulates calcium and other minerals important for bone strength.
Lifestyle Factors
Poor nutrition (low calcium and vitamin D levels), lack of physical activity, smoking, and excessive alcohol consumption can negatively affect bone health over time.
What are the common osteoporosis symptoms?
Osteoporosis often progresses silently, and many people may not notice symptoms until bones become significantly weakened or a fracture occurs. Some common signs that may indicate osteoporosis includ:
-
Frequent fractures that occur even after minor falls, bumps, or everyday activities.
-
Gradual loss of height over time due to compression of the vertebrae in the spine.
-
Stooped or hunched posture that develops as spinal bones weaken and collapse.
-
Back pain persistently caused by small fractures or collapse of vertebrae in the spine.
-
Increased bone fragility, making bones more susceptible to injury and fractures
How is osteoporosis diagnosed?
Early and accurate diagnosis is paramount for effective osteoporosis treatment. The primary tool for this is the DEXA scan (Dual-energy X-ray Absorptiometry), also known as a bone density test. This is a quick, non-invasive, and low-radiation imaging test that measures bone mineral density in key areas like the hip and spine. It is the gold standard for diagnosing osteoporosis and assessing fracture risk and can detect bone loss long before a fracture occurs, allowing for timely intervention. A DEXA scan is typically recommended for women over 65, men over 70, or younger individuals with specific risk factors. Regular monitoring helps track treatment effectiveness.
What are the treatment options for osteoporosis?
Treatment for osteoporosis primarily focuses on slowing bone loss, strengthening existing bones, and reducing the risk of fractures. Management typically involves a combination of medications, calcium and vitamin D supplementation, lifestyle modifications, and regular weight-bearing exercise. Early and appropriate treatment can significantly improve bone health and help maintain mobility and independence. Treatment modalities involve:
Medical Therapy
Medical therapy for Osteoporosis focuses on medications that help slow bone loss, improve bone density, and reduce the risk of fractures. These are administered as:
1. Oral medications
They slow down the rate at which old bone is broken down, allowing new bone formation to catch up. Studies indicate consistent use of these medications can reduce vertebral and hip fractures in most cases. They work by inhibiting bone resorption, helping to maintain existing bone mass.
2. Injections
In individuals with severe osteoporosis and intolerance towards oral medications, or those requiring more potent bone-building effects, injectable medicines are highly effective.\
These include-
-
Bone-building injections are powerful agents that actively stimulate new bone formation, effectively reversing some of the bone loss. They are typically administered daily or weekly via self-injection. Some of them have shown remarkable results, reducing vertebral fractures and non-vertebral fractures over 18-24 months in majority cases.
-
Anti-resorptive injections are administered less frequently (e.g., every six months), and these injections are highly effective at preventing bone breakdown.
Lifestyle modification
While medical interventions are crucial, lifestyle modifications form the cornerstone of any effective treatment for osteoporosis. Combining them with medical therapy can significantly enhance outcomes.
1. Nutrition for bone health
A balanced diet with a regular exercise regimen can improve bone density considerably in adults at risk, complementing medical treatments effectively. What you eat directly impacts your bone strength.
-
Calcium- This is the essential building block for bones. Good sources include dairy products, leafy green vegetables (kale, spinach), fortified cereals, and salmon. Adults typically need 1000-1200 mg per day.
-
Vitamin D- It is crucial for calcium absorption. This is found in fatty fish (salmon, mackerel), fortified milk, and sunlight exposure.
-
Other nutrients- Magnesium, Vitamin K, and protein also play vital roles
2. Exercise for Stronger Bones
Regular physical activity stimulates bone formation and improves balance, reducing fall risk. You can opt for-
-
Weight-bearing exercises- Activities like walking, jogging, hiking, dancing, and stair climbing are excellent as they put stress on your bones, encouraging them to grow stronger.
-
Strength training- Using weights, resistance bands, or your own body weight helps build muscle mass, which supports bones and improves balance.
-
Balance exercises- Tai Chi and yoga can improve coordination and reduce the likelihood of falls.
3. Other lifestyle factors
Other than medications, diet and exercise, a few healthy and safety practices can support the treatment process, enhancing the outcomes. These include-
-
Avoid Smoking: Smoking is highly detrimental to bone health.
-
Moderate Alcohol Intake: Excessive alcohol consumption can impair bone formation.
-
Fall Prevention: Remove hazards at home, use assistive devices if needed, and ensure good lighting.
How to prevent osteoporosis?
Adopting healthy lifestyle habits and maintaining proper nutrition can play a key role in reducing the risk of developing Osteoporosis and supporting long-term bone health.]
Osteoporosis prevention is possible if you:
-
Ensure adequate calcium intake through dairy products, leafy greens, and fortified foods.
-
Maintain sufficient vitamin D levels to support proper calcium absorption and bone health.
-
Engage in regular weight-bearing exercise such as walking, jogging, or strength training.
-
Avoid smoking, as it accelerates bone loss and weakens bone structure.
-
Limit alcohol consumption, which can interfere with calcium balance and bone formation.
-
Maintain a balanced diet rich in protein, fruits, and vegetables for overall bone strength.
-
Maintain a healthy body weight, as being underweight can increase bone loss.
-
Get regular bone density screenings, especially if you have risk factors for osteoporosis.
Conclusion
Early diagnosis and timely treatment are key to effectively managing osteoporosis and protecting long-term bone health. Manipal Hospitals offers a spectrum of advanced osteoporosis treatment options designed to slow bone loss, improve bone density, and reduce fracture risk. Our specialists tailor treatment plans using the latest evidence-based approaches to suit each patient’s needs.
If you are concerned about your bone health or suspect you may be at risk for osteoporosis, seek timely medical advice for a comprehensive assessment and personalised treatment plan from our expert team of orthopaedics at Manipal Hospitals Salt Lake. We focus on proactive and personalised care to help manage osteoporosis and empower you to live a full, active, and independent life.
FAQ's
Generally, women over 65, men over 70, and younger individuals with risk factors like a family history of osteoporosis, certain medical conditions, or long-term steroid use should discuss a DEXA scan with their doctor.
While there's no complete "cure" in the sense of reversing all bone loss, osteoporosis treatment can significantly slow its progression, improve bone density, reduce fracture risk, and manage symptoms effectively. Many patients lead active, fracture-free lives with proper management.
The duration of medicines varies depending on the individual's condition, response to treatment, and fracture risk. It's a decision made in consultation with your doctor, often involving periodic reassessments and sometimes a ‘drug holiday’.
Side effects vary by type but can include gastrointestinal issues, flu-like symptoms, or rare but serious side effects. Your doctor will discuss potential risks and benefits with you, ensuring the chosen treatment is right for your health profile.
Absolutely not. Even after a fracture, starting osteoporosis treatment is crucial to prevent future fractures and improve bone health. Many patients see significant benefits from initiating treatment post-fracture, reducing the risk of subsequent fractures.





















 10 Min Read
10 Min Read