
The pancreas is a vital organ. It sits behind the stomach. It helps in digestion and controls blood sugar. When the pancreas becomes inflamed, the condition is called pancreatitis. Pancreatitis can be sudden or long-term. The symptoms and treatment depend on the type. Recognising pancreatitis symptoms early can help prevent serious complications.
Synopsis
- What is Pancreas Inflammation?
- What is Acute Pancreatitis?
- What is Chronic Pancreatitis?
- Key Differences Between Acute and Chronic Pancreatitis
- How is Pancreatitis Diagnosed?
- Pancreatitis Treatment
- Diet and Lifestyle in Pancreatitis
- Complications of Pancreatitis
- When Should You See a Doctor?
- Can Pancreatitis Be Prevented?
- Conclusion
What is Pancreas Inflammation?
Pancreas inflammation happens when the digestive enzymes of the pancreas start attacking itself. Normally, the pancreas releases digestive juices into the small intestine. These juices contain pancreatic enzymes. They help break down food.
In pancreatitis, these enzymes become active too early. They irritate and damage the pancreatic tissue. This leads to swelling, pain and other health problems.
Pancreatitis is mainly of two types:
-
Acute pancreatitis
-
Chronic pancreatitis
Both conditions need medical attention.
What is Acute Pancreatitis?
Acute pancreatitis is a sudden inflammation of the pancreas. It develops quickly. The pain can be severe. Most people need hospital care.
In many cases, acute pancreatitis improves with proper treatment. However, severe cases can lead to complications.
Common Causes of Acute Pancreatitis
-
Gallstones: Gallstones can block the pancreatic duct. This blockage traps digestive juices inside the pancreas. As a result, the pancreas becomes irritated and inflamed.
-
Heavy alcohol consumption: Excess alcohol can damage pancreatic cells. It also affects the normal flow of pancreatic enzymes. Over time, this can trigger sudden pancreas inflammation.
-
High triglyceride levels: Very high levels of triglycerides in the blood can increase the risk of acute pancreatitis. These fats may interfere with normal pancreatic function and lead to inflammation.
-
Certain medicines: Some medicines can irritate the pancreas as a side effect. Although rare, this reaction may cause sudden inflammation in certain individuals.
-
Abdominal injury: A direct injury to the abdomen, such as from an accident, can damage the pancreas. This damage may lead to swelling and acute pancreatitis.
-
Infections: Certain viral or bacterial infections can affect the pancreas. The infection may trigger inflammation and cause typical pancreatitis symptoms.
Gallstones are one of the most common causes. They can block the pancreatic duct. This causes digestive juices to build up inside the pancreas.
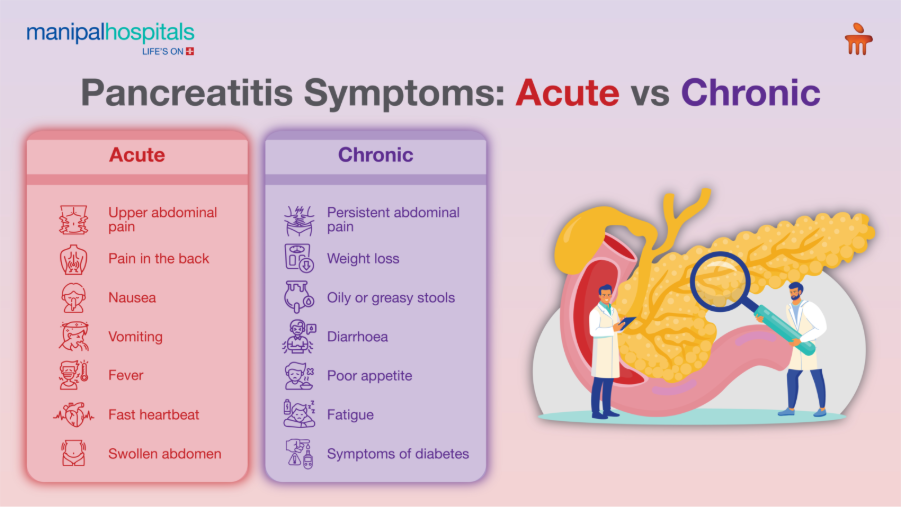
Acute Pancreatitis Symptoms
The symptoms usually start suddenly. They may include:
-
Severe upper abdominal pain radiating to the back
-
Nausea
-
Vomiting
-
Fever
-
Fast heartbeat
-
Swollen or tender abdomen
The abdominal pain may worsen after eating. The pain can last for hours or even days.
These are common pancreatitis symptoms that require urgent medical care.
What is Chronic Pancreatitis?
Chronic pancreatitis is long term inflammation of the pancreas. It develops slowly. Over time, it causes permanent damage.
In chronic pancreatitis, the pancreas loses its ability to function properly. It may not produce enough pancreatic enzymes. This affects digestion. It may also affect insulin production, leading to diabetes.
Common Causes of Chronic Pancreatitis
-
Long term alcohol use: Regular and heavy alcohol intake over many years can slowly damage the pancreas. This repeated injury leads to permanent scarring and long-term pancreas inflammation.
-
Repeated episodes of acute pancreatitis: When a person has several attacks of acute pancreatitis, the pancreas may not fully recover. Over time, this repeated inflammation can result in chronic pancreatitis.
-
Genetic disorders: Certain inherited conditions can affect how the pancreas works. These genetic changes may increase the risk of ongoing inflammation from a young age.
-
Autoimmune diseases: In some cases, the immune system mistakenly attacks the pancreas. This causes continuous inflammation and gradual damage.
-
Blockage in pancreatic ducts: Narrowing or obstruction of the pancreatic ducts can prevent digestive juices from flowing properly. The trapped enzymes can irritate the pancreas and lead to long term damage.
Chronic pancreatitis is more common in adults. However, it can also affect younger individuals, especially when genetic or autoimmune factors are involved.
Chronic Pancreatitis Symptoms
The symptoms may be mild at first. They may worsen over time.
Common signs include:
-
Persistent abdominal pain
-
Weight loss
-
Oily or greasy stools
-
Poor appetite
-
Fatigue
-
Symptoms of diabetes
The oily stools occur because the body cannot digest fats properly. This happens due to reduced production of pancreatic enzymes.
Recognising these pancreatitis symptoms early can help manage the condition better.
Key Differences Between Acute and Chronic Pancreatitis
|
Acute Pancreatitis |
Chronic Pancreatitis |
|
Sudden onset |
Develops slowly |
|
Often reversible |
Causes permanent damage |
|
Severe pain |
Pain may be recurrent, associated with weight loss, malnutrition and maldigestion |
|
Short-term illness |
Long-term condition |
|
May fully recover |
May lead to diabetes and digestive issues |
How is Pancreatitis Diagnosed?
Doctors use a combination of tests to confirm the diagnosis.
Common tests include:
-
Blood tests to check serum amylase and lipase levels
-
Ultrasound scan
-
CT scan
-
MRCP
-
Endoscopic procedures
Pancreatitis Treatment
Treatment depends on the severity and type of pancreatitis.
Treatment for Acute Pancreatitis
Most patients require hospital care. Treatment may include:
-
Intravenous fluids
-
Pain relief medicines
-
Nutritional support
-
Antibiotics if infection is present
If gallstones are the cause, obstructing the opening of the pancreatic duct, the patient requires a special endoscopic procedure called ERCP to remove the stone. Finally, the gallbladder also has to be removed to prevent recurrence in future. Most people recover within a few days to weeks with proper care.
Treatment for Chronic Pancreatitis
Chronic pancreatitis requires long-term management.
Treatment may include:
-
Pain management
-
Pancreatic enzyme supplements
-
Insulin therapy if diabetes develops
-
Dietary changes
-
Avoiding alcohol
Pancreatic enzyme supplements help improve digestion. They reduce symptoms such as oily stools and weight loss.
In severe cases, surgery may be required to relieve pain or remove damaged tissue.
Diet and Lifestyle in Pancreatitis
Diet plays a major role in recovery.
Patients are often advised to:
-
Eat small, frequent meals
-
Choose low-fat foods
-
Avoid fried and oily items
-
Drink plenty of water
-
Stop alcohol completely
-
Avoid smoking
A healthy lifestyle helps reduce inflammation and prevent further damage.
Complications of Pancreatitis
If left untreated, pancreatitis can cause serious problems. Possible complications include:
Acute Pancreatitis
-
Sepsis
-
Overall failure, such as respiratory and kidney failure
Chronic Pancreatitis
-
Malnutrition
-
Diabetes
-
Pancreatic cancer in long-term cases
Early medical care reduces these risks.
When Should You See a Doctor?
You should seek medical help if you experience:
-
Severe abdominal pain spreading to the back
-
Persistent vomiting
-
Fever with abdominal pain
-
Oily stools
Do not ignore persistent pancreatitis symptoms. Delayed treatment can worsen the condition.
Can Pancreatitis Be Prevented?
Not all cases can be prevented. However, certain steps lower the risk.
-
Limit alcohol intake
-
Maintain a healthy weight
-
Control cholesterol and triglyceride levels
-
Eat a balanced diet
-
Treat gallstones early
Regular health check-ups help detect problems early.
Chronic pancreatitis needs long-term care. Regular follow-up is important. Doctors monitor nutrition, blood sugar and pain levels. With proper treatment and lifestyle changes, many people manage the condition well. Early attention to pancreatitis symptoms helps prevent severe damage.
Conclusion
Pancreatitis is a serious condition that may be life-threatening if acute and may affect digestion and overall health in chronic condition. It may appear suddenly as acute pancreatitis or develop slowly as chronic pancreatitis. In both cases, early diagnosis and the right treatment are important. Do not ignore warning signs such as severe abdominal pain, repeated vomiting or unexplained weight loss. These symptoms need timely medical attention. At Manipal Hospitals, Kolkata, our experienced gastroenterologists focus on careful evaluation and personalised care for pancreatic inflammation. We support patients through every stage, from managing acute episodes to providing long-term care for chronic pancreatitis. With the right guidance, monitoring and treatment, many people are able to manage the condition well.
FAQ's
Yes, pancreatitis symptoms can sometimes improve and then return, especially in chronic/recurrent acute pancreatitis. Some people experience repeated abdominal pain for months or years. Even if the pain reduces, the underlying pancreatic inflammation may still be present and needs medical monitoring.
Yes, long-term pancreas inflammation can damage the cells that produce insulin. This may lead to diabetes, especially in chronic pancreatitis. Regular blood sugar monitoring is important for people with ongoing pancreatic problems.
Severe acute pancreatitis can become life-threatening if not treated early. Complications such as sepsis or organ failure may occur. Early recognition of pancreatitis symptoms and prompt medical care greatly reduces these risks.
People with pancreatitis are usually advised to avoid fried foods, fatty meals, processed snacks and alcohol. These foods can increase strain on the pancreas. A low fat and balanced diet supports recovery and reduces flare ups.
Chronic pancreatitis may slightly increase the risk of pancreatic cancer over time. This risk is higher in people who smoke or continue alcohol use. Regular medical follow up helps in early detection of any serious complications.
Mild acute pancreatitis may improve within a few days with proper care. Severe cases may take several weeks and may require hospital stay. Recovery time depends on the cause, overall health and how quickly treatment is started.






















 6 Min Read
6 Min Read














