Irritable Bowel Syndrome (IBS) affects millions worldwide and causes debilitating symptoms, including chronic abdominal pain, bloating, and unpredictable bowel habits. IBS can significantly impact the quality of life. Research shows 10-15% of the world population experiences IBS, yet most of them remain undiagnosed. Ongoing scientific breakthroughs are paving the way for innovative therapies that focus on gut-brain interaction, novel medications, and advanced dietary strategies. The outlook for managing IBS is brighter than ever, promising significant symptom reduction for many. This blog shares the promising landscape of IBS treatments evolving for 2026. The future holds significant hope in a better understanding of IBS symptoms and treatment strategies, with advancements offering more targeted and personalised care.
Synopsis
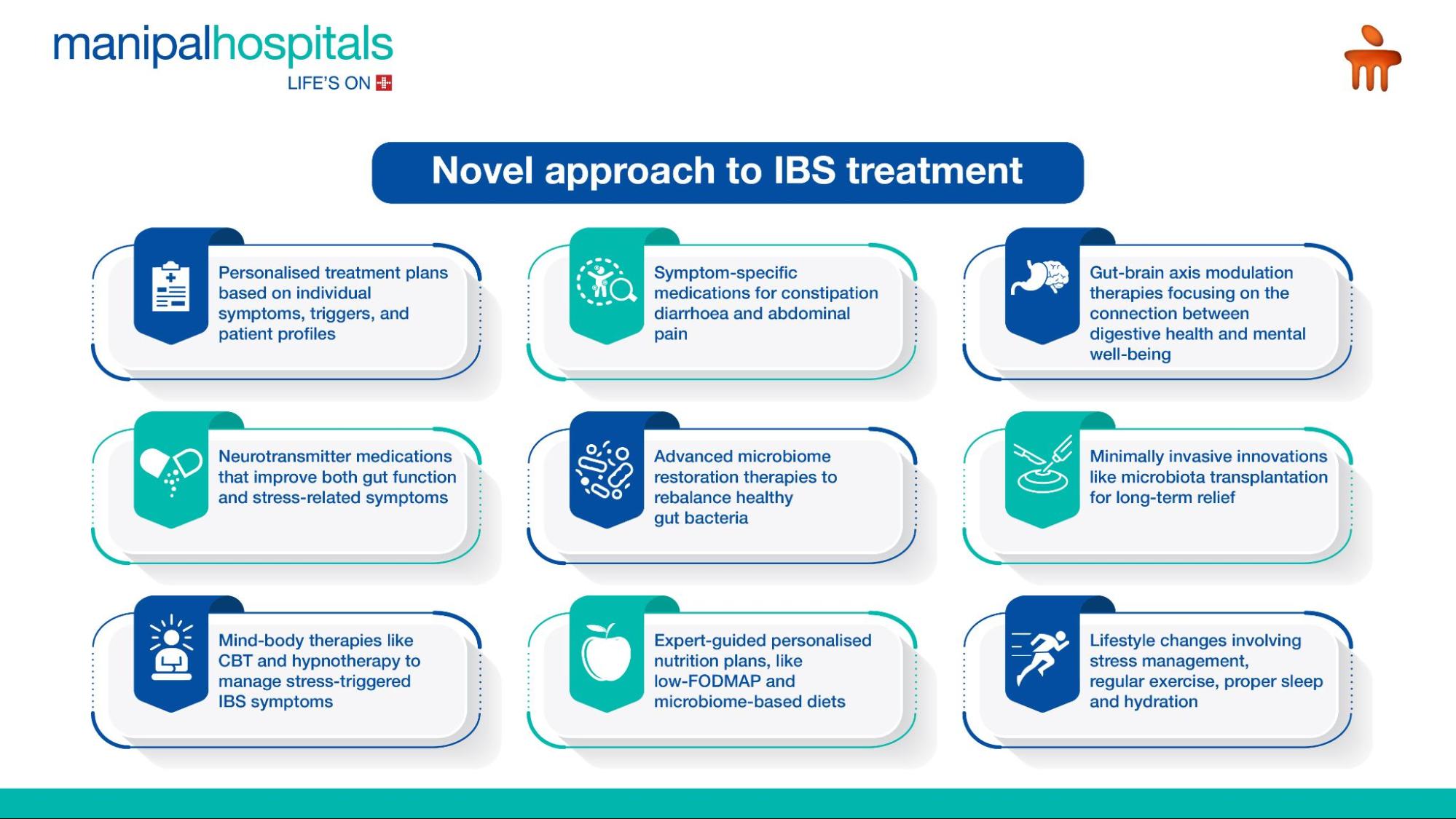
Advanced medications for IBS in 2026
The pharmaceutical scenario for IBS is expanding, making a shift towards targeted therapies. The goal is to provide the best treatment for IBS to individual patients that is tailored to their profiles, moving beyond a generalised approach.
Targeting specific IBS symptoms
Advancements in 2026 are transforming Irritable Bowel Syndrome (IBS) care by introducing targeted therapies that address specific symptoms, offering more precise, effective, and patient-friendly treatment outcomes.
-
Novel agents for bowel function- New medications are designed to alleviate chronic constipation or diarrhoea, influencing gut motility or fluid secretion for precise control over bowel habits.
-
Pain modulators- Advanced pain modulators target visceral hypersensitivity by affecting gut nerve pathways, reducing pain without traditional side effects.
Exploring gut-brain axis modulators
Emerging therapies focused on the gut-brain axis are redefining IBS management by targeting the underlying neurological and microbial interactions that influence both digestive health and emotional well-being.
-
Neurotransmitter regulators- New medications modulate neurotransmitters in the gut-brain axis, offering dual benefits for gut function and mood, especially when IBS is exacerbated by stress.
-
Microbiome-Targeted therapies- Future treatments aim to restore healthy gut bacteria balance through specialised oral therapies or advanced fecal microbiota transplantation, showing promise in regulating immunity and reducing inflammation.
Therapeutic approaches beyond medication
Effective IBS treatments often involve a multi-faceted approach addressing psychological and lifestyle aspects.
Mind-body therapies and diet
A holistic approach to IBS management combines mind-body therapies and personalised dietary strategies to address both the psychological and physiological factors driving symptoms, leading to more sustainable and effective relief.
-
CBT and Hypnotherapy- These therapies help manage IBS by changing negative thought patterns (CBT) and retraining the gut-brain connection (hypnotherapy), offering significant symptom improvement.
-
Dietary interventions- Personalised dietary approaches, including the low-FODMAP diet and tailored plans based on microbiome profiles, are crucial. Working with a dietitian helps identify triggers and optimise nutrient intake.
Gut-healthy lifestyle
Lifestyle practices to help the gut in the long-term management of IBS can complement medical therapies to provide the best treatment for IBS and improve overall gut health.
-
Using probiotics- Discuss specific probiotic strains with your doctor to balance gut flora.
-
Stress management- Techniques like meditation, yoga, and deep breathing reduce stress, a known IBS trigger.
-
Regular exercise- Moderate physical activity regulates bowel function and reduces stress.
-
Adequate hydration and sleep- This is essential for healthy digestion and reducing symptom severity.
Guidelines to aid your treatment outcomes
Following structured, evidence-based guidelines can significantly improve IBS treatment outcomes by ensuring a balanced approach that addresses symptoms, triggers, and long-term gut health.
Practice
-
Keeping a symptom and food diary
-
Following a balanced diet as advised by your healthcare provider
-
Engaging in regular, moderate physical activity
-
Practising stress-reduction techniques
-
Staying hydrated
Avoid
-
Self-diagnosis or self-medication
-
Ignoring persistent or worsening symptoms
-
Cutting out food groups drastically without professional guidance
-
Relying solely on quick fixes.
Conclusion
The prospects of IBS treatments are continuously evolving, offering renewed hope for individuals seeking long-term relief and improved quality of life. At Manipal Hospitals, our experienced gastroenterologists deliver comprehensive, personalised care tailored to your unique symptoms and lifestyle needs. If you are experiencing IBS symptoms or struggling to find effective relief, do not delay seeking expert medical advice—book a consultation with our specialists at Manipal Hospitals EM Bypass today for an accurate diagnosis, advanced treatment, and ongoing support for better digestive health.
FAQ's
The primary goal is to provide more targeted, personalised, and effective relief for IBS symptoms, addressing both the gut and brain aspects of the condition for long-term management and improved quality of life.
Absolutely. Lifestyle changes, including diet modification, stress management, regular exercise, and adequate sleep, are fundamental to managing IBS and can significantly reduce symptom severity for many individuals, often by 30-50%.
The timeline varies greatly depending on the individual, the specific treatment, and the severity of symptoms. Some people may experience relief within weeks, while others might need several months to find an optimal treatment plan and see significant improvement.
IBS is often a chronic condition, meaning it can be long-lasting. However, with effective management strategies, including medications, therapy, and lifestyle adjustments, many individuals can achieve significant symptom control and lead full, active lives.
You should consult a doctor if you experience persistent changes in bowel habits, abdominal pain, bloating, or any new or worsening gastrointestinal symptoms. Early diagnosis and intervention are key to effective management.






















 7 Min Read
7 Min Read







.png)