Irritable Bowel Syndrome (IBS) is a common gastrointestinal disorder affecting millions (approximately 10-15% of the population) worldwide, with many individuals living with symptoms without a formal diagnosis. It brings along several uncomfortable and disruptive symptoms that can significantly impact daily life. While it's more common in women and people under 50, it can affect anyone.
The first step towards irritable bowel syndrome treatment is understanding the condition, identifying the symptoms and knowing the causes or risk factors. This blog gives you an insight into this debilitating condition and explains how to manage it effectively.
Synopsis
Understanding IBS
IBS is a chronic gastrointestinal disorder characterised by abdominal pain or discomfort and changes in bowel habits. It is caused by a disorder in the gut-brain interaction. When the coordination between the gut and the brain is disrupted, it leads to increased sensitivity and changes in the bowel muscle contractions. Unlike other digestive diseases, IBS does not cause visible inflammation or damage to the digestive tract.
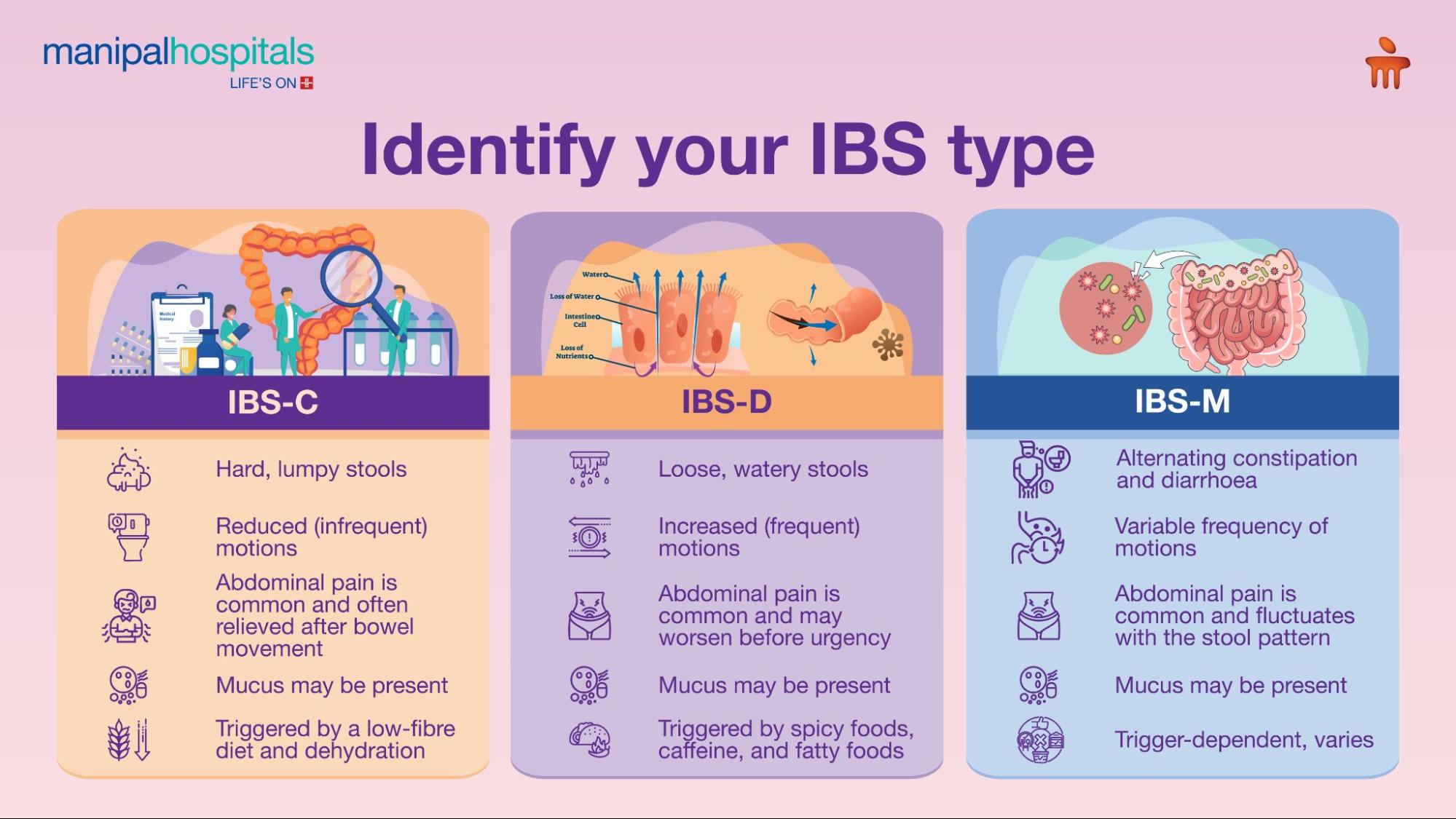
There are predominantly three categories of IBS:
-
IBS-C: Constipation-predominant IBS is characterised by hard, infrequent stools, often accompanied by bloating, abdominal discomfort, and a feeling of incomplete evacuation.
-
IBS-D: Diarrhoea-predominant IBS is marked by frequent loose or watery stools, urgency, and abdominal pain that may improve after bowel movements.
-
IBS-M: Mixed type IBS involves alternating episodes of constipation and diarrhoea, with symptoms varying over time, making it less predictable.
Irritable bowel syndrome causes
The exact causes of irritable bowel syndrome are not fully understood, but it can rarely be attributed to a single cause. According to research, IBS is an interplay of a combination of factors causing sensitivities and disruptions within the gut-brain axis. These factors are:
-
Altered gut motility- Some people with IBS experience faster or slower movement of food through their digestive tract, which leads to diarrhoea or constipation accordingly.
-
Visceral hypersensitivity- There can be an increased sensitivity to pain and discomfort from the bowel, even with normal amounts of gas or stool.
-
Gut microbiome imbalance- Changes in the types or amounts of bacteria in the gut can play a significant role. Restoring the microbiome balance can offer relief for many.
-
Nervous system issues- Problems with the nerves in the gut can cause more discomfort when the abdomen stretches from gas or stool.
-
Severe infection- IBS can sometimes develop after a severe bout of gastroenteritis. This is known as ‘post-infectious IBS’ that can develop in about 10% of such patients.
-
Stress and psychological factors- Stress itself does not cause IBS, but can trigger or worsen the symptoms due to a close connection between the gut and brain.
Irritable bowel syndrome symptoms
Irritable bowel syndrome symptoms can vary widely among individuals, both in type and severity. They often come and go, with periods of remission and flare-ups. Common symptoms of IBS include:
-
Abdominal pain or cramping- This is a hallmark symptom that is often relieved after a bowel movement.
-
Changes in bowel habits- This can manifest as diarrhoea (IBS-D), constipation (IBS-C), or a mix of both (IBS-M).
-
Bloating and gas- A feeling of fullness or visible distension of the abdomen, often accompanied by increased flatulence is common.
-
Mucus in stool- While not always present, some individuals may notice mucus in their stool.
-
Feeling of incomplete evacuation- Some may experience a sensation of incomplete emptying of the bowels after a movement.
-
Food intolerances- Certain foods may trigger symptoms for some individuals.
-
Fatigue and anxiety/depression- The chronic nature of IBS can lead to a vicious cycle of associated symptoms like fatigue, anxiety, or depression. It is observed that over 38% of IBS patients experience anxiety, and over 27% experience depression.
Managing irritable bowel syndrome effectively
While there is currently no definitive answer to ‘how to cure irritable bowel syndrome?’, effective management strategies can significantly reduce symptoms and improve quality of life. The goal of irritable bowel syndrome treatment is to reduce symptoms and address the underlying factors. There are different approaches to it:
Lifestyle and dietary modifications
-
Avoiding triggers- Identifying and avoiding trigger foods, as guided by a dietitian, can reduce symptoms in most patients, including a lowFODMAP (Fermentable Oligo-, Di-, Monosaccharides and Polyols) diet.
-
Fibre intake- Gradually increasing soluble fibre can help regulate bowel movements, especially for IBS-C.
-
Sufficient hydration- Drinking plenty of water is essential for digestive health and optimal gut motility.
-
Regular exercise- Physical activity can help reduce stress and improve gut motility.
-
Stress management- Techniques like meditation, yoga, or deep breathing can be highly beneficial.
Medical management
-
The treating doctor may advise specific interventions to treat symptoms, such as constipation or diarrhoea.
-
Certain medications can help with abdominal pain and spasms.
-
In some cases, specific therapies that target gut flora or nerve sensitivity might be prescribed.
Mind-body therapies
-
Cognitive behavioural therapy (CBT)- This helps change negative thought patterns associated with IBS and teaches coping mechanisms.
-
Hypnotherapy- Gut-directed hypnotherapy is effective for managing IBS symptoms in a large number of patients.
Points to consider
Besides treating or managing the condition, a few proactive considerations in your daily routine can ensure sound gut-health:
-
Maintain a food diary to track what you eat and your symptoms to identify personal triggers.
-
Eat food at regular times every day and avoid skipping meals.
-
Manage stress by incorporating stress-reducing activities into your routine.
-
Consult a gastroenterologist and a dietitian for professional and personalised guidance.
-
IBS symptoms can overlap with other conditions, making a proper diagnosis crucial. Therefore, do not rely on self-diagnosis.
-
Untreated IBS can severely impact quality of life, so do not ignore your symptoms.
-
Use laxatives/antidiarrheals only as directed by your doctor, to avoid overuse.
-
Eliminating foods drastically from your diet without expert guidance can lead to nutritional deficiencies. Abstain from this.
-
Do not hold in your stress; try to find healthy outlets for emotional well-being.
Conclusion
Living with IBS can be challenging, but with the right support and strategies, effective management is possible. If you experience the debilitating symptoms of IBS or have concerns about your digestive health, do not wait. Consult the team of experienced specialists at the gastroenterology department of Manipal Hospitals for timely medical advice.
At Manipal Hospitals Dhakuria, the approach is personalised, focusing on a multi-faceted plan tailored to your specific needs. Here, expert gastroenterologists collaborate with dietitians and mental health professionals to provide comprehensive care, helping you understand your condition and find lasting relief.
FAQ's
While there is no definitive cure for IBS, it can be effectively managed with the right treatment plan. Many individuals achieve significant symptom reduction and lead full, active lives.
IBS is not considered life-threatening and does not lead to more serious conditions like colon cancer or inflammatory bowel disease (IBD). However, it can significantly impact quality of life due to chronic discomfort and disruption.
Common triggers for IBS include certain foods (e.g., high-FODMAP foods, fatty foods, caffeine), stress, hormonal changes (especially in women), and sometimes specific types of medication.
Diagnosis of IBS is typically based on a careful review of your symptoms, medical history, and a physical examination. Your doctor may also perform tests to rule out other conditions that have similar symptoms.
With proper management, most people with IBS can achieve good symptom control and maintain a good quality of life. The condition is chronic but typically does not worsen over time or cause permanent damage to the intestines.






















 7 Min Read
7 Min Read