
When someone you care about is told they need a Whipple’s procedure, the first feeling is usually a mix of fright, urgency, and a hundred unanswered thoughts. The surgery itself is complex. It involves removing and reconstructing delicate structures deep inside the abdomen. But what often goes unseen is the quiet work that happens before a single incision is made.
This is where precision imaging & surgical planning step in. Long before the operating theatre lights are switched on, surgeons are studying detailed scans. They are tracing blood vessels, mapping tumour borders, and anticipating challenges. Modern imaging for the Whipple procedure has transformed this preparation stage into something remarkably exact. And that preparation changes everything.
This blog explores how advanced imaging improves surgical safety, supports accurate decision-making, reduces intraoperative risks, and influences recovery.
Synopsis
- Why Imaging Matters in a Whipple’s Procedure
- The Imaging Tools That Shape Surgical Strategy
- From Pictures to a Surgical Blueprint
- Determining Whether Surgery is Possible
- How Advanced Imaging Reduces Surgical Risk
- The Role of 3D Reconstruction and Digital Planning
- Impact on Recovery and Long-Term Outcomes
- Conclusion
Why Imaging Matters in a Whipple’s Procedure
The Whipple’s procedure, also known as pancreaticoduodenectomy, is most commonly performed for cancers of the pancreas, bile duct, or duodenum. These organs sit in one of the most crowded and complex areas of the body. Major blood vessels run just millimetres away from the pancreas. Even small variations in anatomy can make a difference.
Today, advanced imaging provides a detailed roadmap beforehand. That means fewer surprises, better decision-making, and more confidence when navigating tight spaces. With advanced scans, surgeons can evaluate tumour size, vessel involvement, lymph node status, and even subtle anatomical differences unique to each patient.
The Imaging Tools That Shape Surgical Strategy
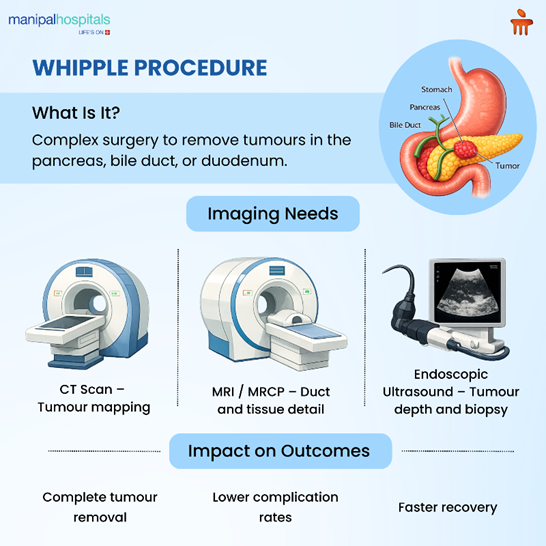
Modern imaging for Whipple procedure involves a combination of technologies. Each serves a specific purpose.
Contrast-Enhanced CT Scans
A high-quality, multi-phase CT scan is often the foundation. It helps identify:
-
Tumour location
-
Size and boundaries
-
Involvement of nearby arteries and veins
-
Possible spread to other organs
The timing of contrast injection allows doctors to see blood vessels clearly. This is critical when deciding whether the tumour can be safely removed.
MRI and MRCP
MRI provides more detailed soft tissue contrast. It is particularly helpful when assessing bile ducts and subtle tumour spread. MRCP images the pancreatic and bile ducts clearly, helping surgeons understand blockages and anatomical variations.
Endoscopic Ultrasound (EUS)
EUS allows close-up imaging from inside the digestive tract. It is often used to confirm tumour size and obtain biopsies. It also gives insight into the depth of invasion.
Each of these tools contributes to precision imaging & surgical planning in a slightly different way. Together, they form a layered, three-dimensional understanding of the disease.
From Pictures to a Surgical Blueprint
A scan by itself is just data. What makes a difference is interpretation. Surgeons review imaging in multidisciplinary meetings. Radiologists highlight vascular involvement. Oncologists weigh in on tumour biology. Surgeons visualise how they will approach dissection and reconstruction.
With advanced imaging, surgeons can:
-
Plan vascular reconstruction if needed
-
Anticipate anatomical variations
-
Estimate operative time
-
Reduce intraoperative uncertainty
Determining Whether Surgery is Possible
Not every pancreatic tumour can be safely removed. Advanced imaging plays a decisive role in determining whether surgery is feasible. Surgeons assess:
-
Whether the tumour encases major blood vessels
-
Whether distant metastasis is present
-
Whether nearby organs are significantly involved
If vessels are partially involved, reconstruction might still be possible. If there is widespread spread, chemotherapy may be recommended first. This step is crucial. Operating without complete information can lead to incomplete tumour removal or unexpected complications. Proper imaging for Whipple procedure reduces those risks.
How Advanced Imaging Reduces Surgical Risk
Complications after a Whipple’s procedure can include bleeding, pancreatic leaks, infections, and delayed gastric emptying. While not all complications are preventable, careful planning significantly lowers risk. The table below summarises some of the ways detailed imaging helps guide the operation:
|
Imaging Contribution |
Surgical Impact |
Outcome Benefit |
|
Clear vascular mapping |
Accurate dissection around arteries and veins |
Reduced bleeding risk |
|
Tumour boundary definition |
Higher chance of complete tumour removal |
Improved long-term survival |
|
Identification of anatomical variations |
Fewer intraoperative surprises |
Lower complication rates |
|
Preoperative 3D reconstruction |
Better orientation in complex anatomy |
Shorter operative time |
|
Multidisciplinary review |
Well-coordinated surgical strategy |
Improved overall safety |
When imaging clearly defines vascular involvement, surgeons can avoid incomplete resections. When anatomical variations are recognised beforehand, there is less likelihood of accidental injury. Better planning also reduces operative time. And shorter operative time often correlates with lower infection risk and faster recovery.
The Role of 3D Reconstruction and Digital Planning
One of the most exciting developments in imaging for whipple procedure is 3D reconstruction. Instead of viewing flat slices on a screen, surgeons can now see a three-dimensional model of the pancreas and surrounding vessels.
This technology can:
-
Clarify spatial relationships
-
Assist in planning incision placement
-
Improve confidence in complex dissections
In particularly complex cases, it can even determine whether surgery is feasible or whether another treatment approach would be safer. It also improves communication. Surgeons can show patients exactly where the tumour sits and explain the surgical plan more clearly. For families trying to understand a complicated diagnosis, that visual clarity brings reassurance
Impact on Recovery and Long-Term Outcomes
Patients often focus on getting through surgery. But recovery matters just as much. When surgery is precise and margins are clear, there is a lower likelihood of needing additional corrective procedures. When blood loss is minimised, patients regain strength more quickly.
Studies consistently show that better preoperative imaging correlates with:
-
Higher rates of complete tumour removal
-
Reduced need for reoperation
-
Improved postoperative stability
-
Better long-term survival in selected patients
The effects ripple far beyond the operating theatre.
Conclusion
Behind every scan is a family trying to make sense of uncertainty. You are not just looking at numbers and measurements. You are trying to understand what lies ahead. Advanced imaging offers something subtle but powerful: preparedness. When your surgical team walks into the operating theatre with a detailed roadmap, that preparation reflects respect for the complexity of your situation. It reflects effort and care. And sometimes, knowing that your team has studied every angle brings a sense of steadiness in an otherwise overwhelming time. At Manipal Hospitals Bangalore, we use the same advanced imaging techniques and explain each scan, so you can rest assured.
FAQ's
Imaging defines tumour size, vessel involvement, and spread. It helps surgeons decide if surgery is safe and feasible, reducing unexpected complications during the operation and improving overall outcomes.
Yes. Advanced scans assess whether major arteries or veins are involved. This helps predict whether complete tumour removal is possible before proceeding to surgery.
In many cases, yes. Detailed preoperative planning reduces intraoperative surprises, which can shorten surgical time and lower complication risk.
Not always. It is particularly useful in complex or borderline cases where vascular involvement is unclear or reconstruction may be required.
It contributes significantly by ensuring complete tumour removal when possible and selecting appropriate candidates for surgery, both of which influence long-term outcomes.






















 7 Min Read
7 Min Read













