- Stroke-Ready Hospital
-
Centre of
Excellence
Centre of Excellence
- Bariatric Surgery - MIBS
- Women's Cancer Care
- Cardiology
- Cardiothoracic Vascular Surgery
- Clinical Haematology and Hemato-Oncology
- Comprehensive Cancer Care
- Gastrointestinal Science
- Interventional Neuroradiology
- Liver Transplantation Surgery
- Nephrology
- Neurology
- Neurosurgery
- Obstetrics and Gynaecology
- Orthopaedics and Joint Replacement
- Spine Care
- Stroke Care
- Urology
Other Specialities
- Anesthesiology
- Bariatric Surgery | Weight loss surgery
- Clinical Psychology
- Dental Medicine
- Dermatology
- Diabetes and Endocrinology
- Electrophysiology
- ENT – Head and Neck Surgery
- Fetal Medicine
- General Medicine
- General Surgery
- Genetics
- Geriatric Medicine
- GI Surgery
- Gynaec Oncology
- Hepatobiliary Surgery
- ICU and Critical Care
- Internal Medicine
- Interventional Pulmonology
- Laboratory Medicine
- Medical Gastro
- Medical Oncology
- Microbiology
- Minimal Access Surgery
- Neonatology & NICU
- Nocturnal Dialysis
- Nuclear Medicine
- Nutrition And Dietetics
- Ophthalmology
- Oral Maxillo Facial Surgery
- Orthopaedic Oncology
- Paediatric And Child Care
- Paediatric Cardiology
- Paediatric Endocrinology
- Paediatric Pulmonology
- Paediatric Surgery
- Pain Management
- Pathology
- Pharmacy
- Physiotherapy
- Plastic And Cosmetic Surgery
- Psychiatry
- Psychology
- Radiology
- Radiotherapy (Oncology Radiation)
- Renal Sciences
- Rheumatology
- Robotic Assisted Surgery
- Sports Medicine
- Surgical Gastro
- Surgical Oncology
- Transfusion Medicine
- Vascular and Endovascular Surgery
Speciality Clinics
- Adolescent & Teen Health Clinic (Physical, Emotional, and Social Well-being)
- Cholesterol Management Clinic
- Geriatric Care Clinic
- Heart Failure Clinic
- Liver Clinic
- Metabolic Clinic
- Onco-Dermatology Clinic
- Psychology & Behavioural Health Clinic
- Thyroid Management Centre/Clinic
- Uro-Gynaecology Clinic
- Weight & Metabolic Health Clinic
- Doctors
- Kanakapura Road
-

Bengaluru

-
-

Bhubaneswar

-

Bhubaneswar
-
-

Delhi - NCR

-

Goa

-

Goa
-
-

Jaipur
-

Kolkata

-

Mangaluru
-

Mysuru
-

Patiala
-

Pune

-

Ranchi
-

Salem
-

Siliguri City

-

Vijayawada
- International Patients



Clinics







- Self Registration
- In-Patient Deposit
- Mars - Ambulance
- Home Care
- Organ Donation
- Corporate & PSU
- Awards And Achievements
- Manipal Insider
- Careers
- Contact Us
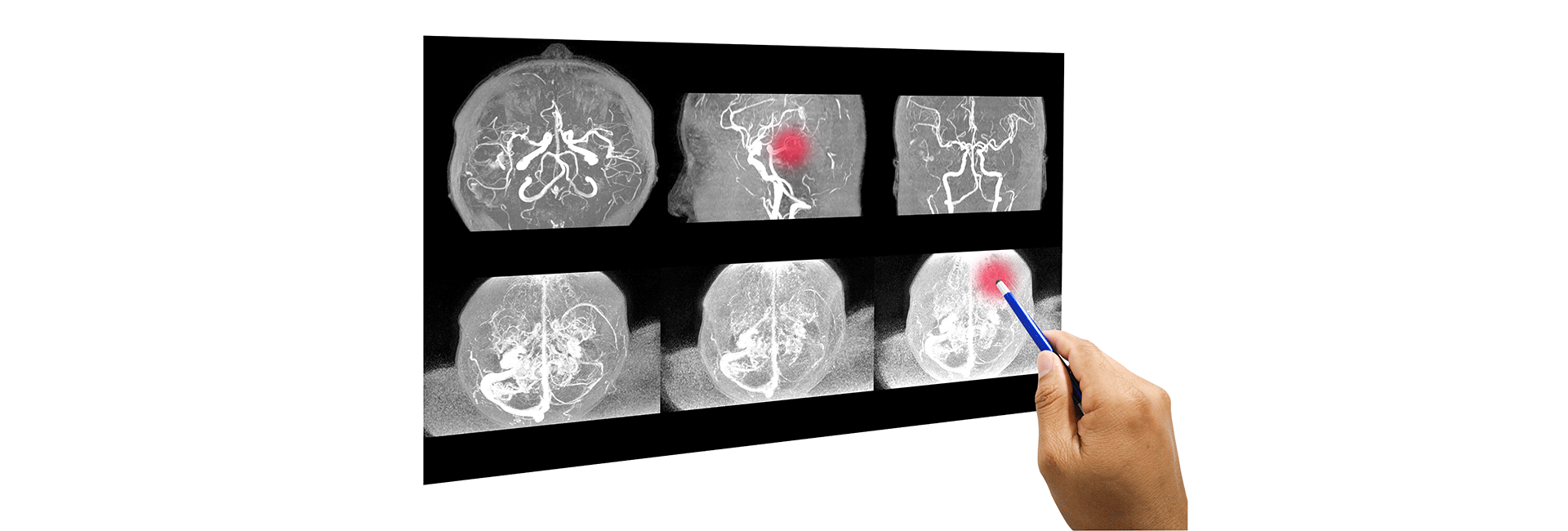
Preoperative Tumor Embolization
Preoperative Tumour Embolisation in Kanakapura Road
Facing tumour surgery can feel overwhelming, especially when the unknowns seem larger than the diagnosis itself. One of the most common concerns is how safely the tumour can be removed, particularly when it is surrounded by a dense network of blood vessels. At Manipal Hospitals, this is addressed early through careful planning, including preoperative tumour embolisation in Kanakapura Road, Bangalore. Rather than being a standalone treatment, it prepares the body for surgery by reducing the tumour’s blood supply, helping create a more controlled surgical environment and allowing the team to operate with greater precision and confidence.
How It Works
Preoperative tumour embolisation is used when a brain or spinal tumour is fed by many tiny blood vessels and would likely bleed heavily during surgery. The aim is not to remove the tumour itself, but to reduce its blood supply before the neurosurgeon operates. That preparation can make the surgical field clearer, the procedure more controlled, and blood loss significantly lower.
The process begins with detailed angiographic imaging. This maps the vessels feeding the tumour and shows which arteries can be safely targeted. The interventional radiology team studies the anatomy carefully because vascular tumours can be supplied by several small branches, and each one may behave differently. Good planning here matters just as much as the embolisation itself.
On the procedure day, the patient is placed under monitored anaesthesia or sedation. A thin catheter is advanced through a blood vessel, usually from the groin or wrist, and guided into the arteries supplying the tumour. Once the catheter is in position, the specialist injects tiny particles such as PVA or microspheres, or sometimes a liquid embolic agent, to block the blood flow feeding the mass.
Over time, the devascularised part of the tumour begins to soften or necrose, which reduces bleeding risk during the next surgery. In many cases, the neurosurgeon can remove the tumour more safely and efficiently after embolisation. That is why tumour embolisation in Kanakapura Road, Bangalore is often considered an important bridge between diagnosis and definitive surgical treatment, especially for highly vascular lesions like meningiomas or paragangliomas.
After the procedure, the patient is monitored for neurological changes, headache, pain, or any sign that the embolisation has affected nearby tissue. The team then reviews the response and coordinates the timing of surgery. Sometimes surgery follows soon after embolisation, while in other cases the plan is adjusted based on tumour type, location, and how much of the blood supply has been successfully closed.
Benefits
Key benefits include:
-
Reduces blood flow to highly vascular tumours before surgery
-
Helps lower blood loss during the open operation
-
Can make tumour removal safer and more controlled
-
Improves surgical visibility for the operating team
-
May reduce operative time in selected cases
-
Supports better planning for complex brain and spinal tumour surgery
What to Expect
From the first imaging review to the final surgical plan, the experience is designed to feel organised and transparent.
Initial Evaluation and Planning
The process starts with angiographic studies and a careful review of the tumour’s vascular supply. The team decides whether embolisation will help reduce bleeding and how much of the blood flow can be targeted safely.
Procedure Preparation
Before embolisation, the patient is evaluated for anaesthesia readiness, neurological status, and overall medical stability. The procedure is explained clearly so the patient and family know what the goal is and how it fits into the larger treatment plan.
Catheter-Based Embolisation
During the procedure, the catheter is advanced to the arteries feeding the tumour. Tiny embolic particles or liquid material are delivered to block those vessels and decrease blood flow to the mass.
Observation After the Procedure
Once embolisation is complete, the patient is monitored closely for headache, neurological symptoms, or blood pressure changes. This period helps the team identify whether the embolisation has been well tolerated.
Surgery Planning and Follow-Up
The final step is coordination with the neurosurgical team. The surgeon reviews the embolisation result and plans the timing of tumour removal, often with less bleeding risk than before.
Why Manipal Hospital
At Manipal Hospital Kanakapura Road, the focus is on making complex tumour surgery safer before the first incision is ever made. That means the work begins well before the operating theatre. Careful imaging review, procedural planning, and close coordination between teams help ensure embolisation is used only when it will genuinely improve the next stage of treatment. Patients often value that kind of thoughtful approach when they are facing surgery for a vascular tumour. It is part of what makes tumour embolisation treatment in Kanakapura Road feel more controlled, less overwhelming, and better linked to the larger surgical plan. To keep that process smooth, the care pathway includes:
-
Advanced angiographic planning for tumour blood supply mapping
-
Image-guided catheter navigation for precise vessel targeting
-
Coordination between neurointerventional specialists and neurosurgeons
-
Careful post-procedure monitoring before definitive tumour surgery
-
Individualised timing of surgery based on embolisation response
-
Clear family communication before, during, and after treatment
-
Structured follow-up to review safety and surgical readiness
-
Hospital-based support for complex brain and spinal tumour cases
Speciality - Interventional Neuroradiology
Interventional Neuroradiology is the speciality that uses image-guided, minimally invasive techniques to treat vascular conditions inside the brain and spine. Preoperative tumour embolisation helps reduce blood flow to highly vascular tumours before surgery, improving safety, control, and overall surgical planning.
Services Offered
Our service includes angiographic evaluation, embolisation planning, catheter-based vessel occlusion, and coordination with neurosurgery for the next stage of treatment. It also covers post-procedure observation, neurological monitoring, and review of imaging to determine how much of the tumour blood supply has been successfully reduced.
Facilities and Services
For preoperative tumour embolisation in Kanakapura Road, Bangalore, the care environment is built for precision, timing, and safe transition into surgery. Every step is supported by imaging, monitoring, and multidisciplinary review, so the patient moves through treatment with as little uncertainty as possible.
-
Advanced angiography suite for detailed tumour vessel mapping
-
High-precision catheter systems for selective arterial access
-
Embolic particle and liquid delivery setup for targeted devascularisation
-
Monitored recovery space for post-procedure observation
-
Anaesthesia support for complex neurovascular interventions
-
On-site imaging for preoperative planning and post-embolisation review
-
Coordination with neurosurgery for surgery timing and readiness
-
Access to critical care if higher-level observation is needed
FAQ's
No, it is used when a tumour has a very rich blood supply, and removing it without embolisation would carry a higher risk of heavy bleeding. The decision is made individually based on imaging and surgical planning.
No, the goal is to block the blood vessels feeding the tumour, not to remove the mass. This makes the subsequent surgery safer by reducing blood loss and improving visibility for the neurosurgeon.
Most patients experience mild headache or groin discomfort for a day or two. You will be monitored closely for any neurological changes before being cleared for the planned surgery.
Surgery is usually scheduled within 24 to 72 hours after embolisation. This timing ensures the tumour remains devascularized before new collateral vessels can form.
Yes, this is a standard pre-surgical procedure for vascular tumours and is typically covered. Our team can help verify your insurance coverage and explain any costs before scheduling.
Home Kanakapuraroad Specialities Interventional-neuroradiology Preoperative-tumor-embolization

You’re on Our Indian Website
Visit the Global site for International patient services





