- Stroke-Ready Hospital
-
Centre of
Excellence
Centre of Excellence
- Bariatric Surgery - MIBS
- Women's Cancer Care
- Cardiology
- Cardiothoracic Vascular Surgery
- Clinical Haematology and Hemato-Oncology
- Comprehensive Cancer Care
- Gastrointestinal Science
- Interventional Neuroradiology
- Liver Transplantation Surgery
- Nephrology
- Neurology
- Neurosurgery
- Obstetrics and Gynaecology
- Orthopaedics and Joint Replacement
- Spine Care
- Stroke Care
- Urology
Other Specialities
- Anesthesiology
- Bariatric Surgery | Weight loss surgery
- Clinical Psychology
- Dental Medicine
- Dermatology
- Diabetes and Endocrinology
- Electrophysiology
- ENT – Head and Neck Surgery
- Fetal Medicine
- General Medicine
- General Surgery
- Genetics
- Geriatric Medicine
- GI Surgery
- Gynaec Oncology
- Hepatobiliary Surgery
- ICU and Critical Care
- Internal Medicine
- Interventional Pulmonology
- Laboratory Medicine
- Medical Gastro
- Medical Oncology
- Microbiology
- Minimal Access Surgery
- Neonatology & NICU
- Nocturnal Dialysis
- Nuclear Medicine
- Nutrition And Dietetics
- Ophthalmology
- Oral Maxillo Facial Surgery
- Orthopaedic Oncology
- Paediatric And Child Care
- Paediatric Cardiology
- Paediatric Endocrinology
- Paediatric Pulmonology
- Paediatric Surgery
- Pain Management
- Pathology
- Pharmacy
- Physiotherapy
- Plastic And Cosmetic Surgery
- Psychiatry
- Psychology
- Radiology
- Radiotherapy (Oncology Radiation)
- Renal Sciences
- Rheumatology
- Robotic Assisted Surgery
- Sports Medicine
- Surgical Gastro
- Surgical Oncology
- Transfusion Medicine
- Vascular and Endovascular Surgery
Speciality Clinics
- Adolescent & Teen Health Clinic (Physical, Emotional, and Social Well-being)
- Cholesterol Management Clinic
- Geriatric Care Clinic
- Heart Failure Clinic
- Liver Clinic
- Metabolic Clinic
- Onco-Dermatology Clinic
- Psychology & Behavioural Health Clinic
- Thyroid Management Centre/Clinic
- Uro-Gynaecology Clinic
- Weight & Metabolic Health Clinic
- Doctors
- Kanakapura Road
-

Bengaluru

-
-

Bhubaneswar

-

Bhubaneswar
-
-

Delhi - NCR

-

Goa

-

Goa
-
-

Jaipur
-

Kolkata

-

Mangaluru
-

Mysuru
-

Patiala
-

Pune

-

Ranchi
-

Salem
-

Siliguri City

-

Vijayawada
- International Patients



Clinics







- Self Registration
- In-Patient Deposit
- Mars - Ambulance
- Home Care
- Organ Donation
- Corporate & PSU
- Awards And Achievements
- Manipal Insider
- Careers
- Contact Us
Mechanical Thrombectomy
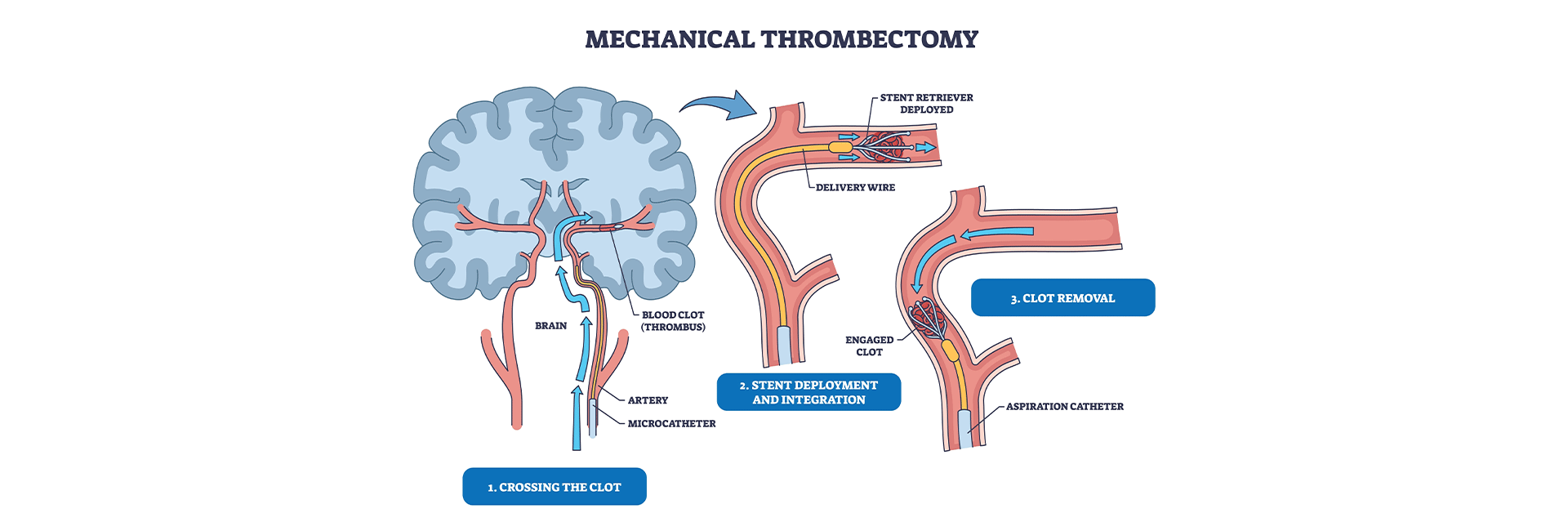
Mechanical Thrombectomy Procedure in Kanakapura Road
A stroke does not always come with a warning. Sometimes it is a sudden weakness, slurred speech, or a moment where the body simply does not respond the way it should. In those first few minutes, what happens next can shape recovery in a very real way. At Manipal Hospital Kanakapura Road, stroke care is built around urgency, clarity, and precision. Every second matters, but so does doing the right thing at the right time. Using advanced imaging and rapid intervention pathways, our team focuses on restoring blood flow to the brain as quickly and safely as possible. For patients with large vessel blockages, the mechanical thrombectomy procedure in Kanakapura Road, Bangalore offers a targeted way to remove the clot and limit long-term damage.
How It Works
Mechanical thrombectomy is a minimally invasive procedure used to treat acute ischaemic strokes caused by a blocked artery in the brain. Instead of relying only on medication to dissolve the clot, this technique physically removes it, which can significantly improve outcomes in selected patients.
The procedure begins with a small puncture, usually in the groin or wrist. Through this access point, a catheter is carefully guided through the blood vessels up to the blocked artery in the brain. Real-time imaging allows the neurointerventional specialist to navigate with precision, ensuring the surrounding vessels remain protected.
Once the catheter reaches the clot, specialised devices are used to remove it. A stent retriever may be used to trap and remove the clot, or an aspiration catheter may gently suction it. In some cases, both techniques are combined for better results. The goal is simple but critical: restore blood flow quickly to the affected brain tissue.
At Manipal Hospital Kanakapura Road, this entire process is coordinated within a structured stroke response system, ensuring rapid decision-making, continuous monitoring, and seamless transition to post-procedure care.
Benefits
For patients with large vessel occlusion stroke, mechanical thrombectomy offers a chance at recovery that was not possible a generation ago. Key benefits include:
-
Rapid restoration of blood flow to affected brain regions.
-
Reduced risk of long-term disability when performed in time.
-
A minimally invasive approach with controlled vascular access.
-
Effective treatment for large vessel occlusions not responsive to medication alone.
-
Structured stroke care with close neurological monitoring during recovery.
What to Expect
From the moment a stroke is suspected to the recovery phase, care is designed to move quickly while keeping patients and families informed.
-
Emergency Evaluation
-
When a patient with suspected stroke arrives, imaging is performed immediately. CT angiography shows whether there is a large vessel occlusion. Perfusion imaging shows how much brain tissue is still salvageable. If the patient is a candidate, the team is activated.
-
-
The Thrombectomy Procedure
-
The patient is taken to the angiography suite. Access is obtained, and the catheter is navigated to the clot. The removal takes minutes to an hour, depending on the complexity. Families receive updates throughout.
-
-
Post-Procedural Monitoring
-
After the procedure, the patient is moved to the intensive care unit. Blood pressure is tightly controlled. Neurological checks are performed frequently. The team watches for signs of reperfusion injury or haemorrhage.
-
-
Ongoing Monitoring and Recovery
-
After the procedure, patients are closely observed for neurological improvement, blood pressure stability, and any complications. Recovery varies, but early improvement is often a positive sign.
-
-
Family Communication and Rehabilitation Planning
-
Families are updated regularly. Once stable, rehabilitation planning begins, focusing on regaining movement, speech, and independence through structured therapy.
-
Why Manipal Hospitals
At Manipal Hospital Kanakapura Road, stroke treatment is delivered through a tightly coordinated system where every minute is accounted for. The team combines speed with clinical precision, ensuring that decisions are both timely and appropriate. Access to a mechanical thrombectomy procedure for stroke in Kanakapura Road within this integrated setup makes a measurable difference in outcomes and recovery. To support this level of care, our hospital brings together expertise, infrastructure, and real-time coordination:
-
24/7 stroke response teams trained for rapid assessment and intervention
-
Immediate access to advanced CT and vascular imaging
-
Dedicated neurointerventional suites for emergency procedures
-
Continuous neurological monitoring in specialised critical care units
-
Collaboration between neurology, radiology, anaesthesia, and rehabilitation teams
-
Early initiation of physiotherapy and speech therapy after stabilisation
-
Clear, consistent updates provided to families during treatment decisions
Specialty – Neurointerventional Radiology
Neurointerventional radiology at Manipal Hospital Kanakapura Road specialises in minimally invasive, image-guided treatments for acute ischaemic stroke. For mechanical thrombectomy, the team navigates catheters to large vessel occlusions, uses stent retrievers and aspiration catheters to remove clots, and restores blood flow to brain tissue, significantly reducing the risk of long-term disability.
Services Offered
Our mechanical thrombectomy services include 24/7 stroke team activation, rapid CT angiography and perfusion imaging to identify large vessel occlusions and salvageable brain tissue, femoral and radial artery access, stent retriever and aspiration thrombectomy, combined SOLUMBRA technique for complex clots, post-procedural intensive care monitoring, and early integration with rehabilitation services.
Facilities and Services
Delivering effective stroke care requires more than speed; it depends on having the right systems in place at every step. At Manipal Hospital Kanakapura Road, the infrastructure is built to support advanced thrombectomy surgery in Kanakapura Road, Bangalore, with accuracy and reliability:
-
High-resolution brain and vascular imaging for immediate diagnosis
-
Fully equipped neurointerventional labs for catheter-based stroke procedures
-
Continuous cardiac and neurological monitoring systems
-
Specialised stroke care units for post-procedure observation
-
On-site anaesthesia and critical care support for complex cases
-
Rehabilitation services, including physiotherapy and speech therapy
-
Integrated lab and imaging support for ongoing evaluation
-
Long-term follow-up protocols that include risk factor modification, medication management, and ongoing rehabilitation planning
FAQ's
Patients with acute ischaemic stroke caused by a large vessel occlusion, within 6 to 24 hours of symptom onset, with salvageable brain tissue on imaging, are candidates. The decision is made quickly after arrival.
Time is critical. The goal is to have the patient in the angiography suite within 60 to 90 minutes of arrival. Every minute saved increases the chance of a good outcome.
You will be under sedation or general anesthesia, so you will not feel pain. The team monitors you closely throughout, and for some patients, improvement can be seen immediately after the clot is removed.
Recovery varies. Some patients show dramatic improvement immediately. Others improve more slowly over weeks. Rehabilitation begins early and continues after discharge. Outcomes are significantly better than with medical therapy alone.
Risks include vessel injury, haemorrhage, and reperfusion injury. Our team minimises these through careful technique, patient selection, and meticulous post-procedural management.
Patients are monitored in a specialised unit for neurological changes and recovery progress. Rehabilitation begins early, focusing on movement, speech, and daily function, with ongoing follow-up to track long-term improvement.
Home Kanakapuraroad Specialities Interventional-neuroradiology Mechanical-thrombectomy

You’re on Our Indian Website
Visit the Global site for International patient services





