Can a single pale patch on the skin trigger a lasting shift in appearance and confidence?
Vitiligo is a condition where the skin loses pigment, leading to white spots on the skin that can grow or appear in new places. Knowing the vitiligo meaning, its common presentations, the likely vitiligo causes, and treatment options helps make timely, practical choices. Early diagnosis and a clear plan reduce uncertainty and give a person control over symptoms, appearance strategies, and medical choices. This blog explains types of vitiligo, how it develops, how doctors confirm the condition, and the full range of effective treatments available today.
Synopsis
What is Vitiligo?
Understanding vitiligo is easier when you know what it means in simple terms. Vitiligo is a long-lasting skin condition where some areas lose their natural colour and turn white. This happens when melanocytes, the cells that produce melanin, stop working or die. Melanin gives colour to your skin, hair, and eyes. When melanin is missing, white spots appear on the skin. These patches can stay the same size or grow over time. Vitiligo can have an effect on skin, hair, mouth, or eyes. Anyone can develop vitiligo, but it is more noticeable on people with darker skin.
Common Signs of Vitiligo
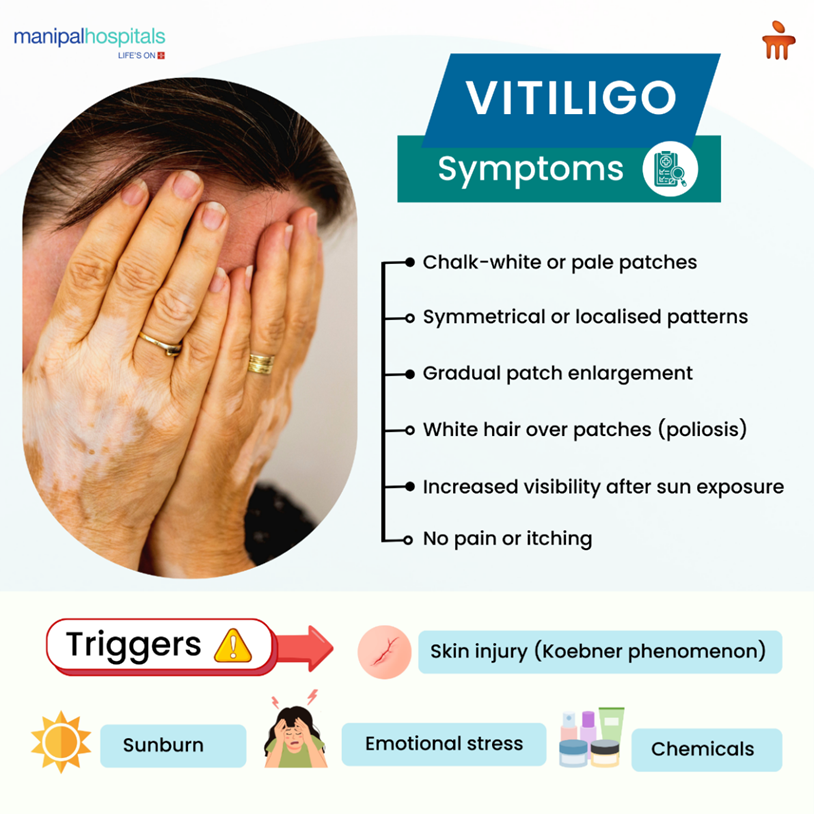
Vitiligo usually doesn’t cause itching, pain, or other physical vitiligo symptoms. However, it can have a strong impact on mental and emotional health, especially for children and young adults. Some common symptoms of vitiligo include:
-
Well-demarcated pale or chalky patches on the skin.
-
Symmetry in some patterns (both hands, around the eyes) or isolated patches.
-
Early signs may include small spots that gradually enlarge.
-
Hair in affected areas may turn white (poliosis).
-
Prominent patches appear after prolonged sun exposure.
Different Types of Vitiligo
Vitiligo doesn’t look the same for everyone. Doctors group types of vitiligo based on how the white spots appear and spread. The following are its types:
|
Types |
Definition |
Features |
Progression |
|
Non-Segmental Vitiligo |
The most common form is where white patches appear on both sides of the body in a fairly similar pattern. |
Patches develop on the hands, face, knees, elbows, and around the eyes or mouth. Hair in affected areas may also turn white. |
It usually develops slowly over time and may spread to different parts of the body. Periods of stability and change are common. |
|
Segmental Vitiligo |
A less common type that affects only one side or one specific area of the body. |
Patches appear in a smaller, clearly defined area like one arm/leg or one side of the face. It usually begins at a younger age. |
This type often spreads quickly in the early stages and then becomes stable after some time. |
|
Focal Vitiligo |
A mild form where depigmented patches appear in one or a few small areas. |
The patches remain limited and don’t follow a clear pattern. They may appear anywhere on the body. |
It may stay localised for years, and in some cases, it may develop into another type of vitiligo. |
|
Acrofacial Vitiligo |
A type that mainly affects areas away from the centre of the body. |
White patches appear on fingers, toes, lips, ears, and facial openings like the eyes and nose. |
It may gradually spread but often remains focused on these specific areas. |
|
Universal Vitiligo |
A rare and advanced type where most of the skin loses its natural colour. |
Large areas of depigmentation appear across the body, affecting almost all skin surfaces. |
It develops slowly and is uncommon, but it can significantly change overall skin colour. |
|
Mucosal Vitiligo |
A type that affects mucous membranes rather than the outer skin. |
Depigmentation appears inside the mouth, lips, or genital areas. |
It may remain limited to these regions and does not always spread to the skin. |
Vitiligo Causes
The exact causes of vitiligo are complex and usually multifactorial. Key contributors of the disease can be:
-
Autoimmune mechanisms: The immune system incorrectly targets melanocytes, causing their destruction. Vitiligo often coexists with other autoimmune conditions (thyroid disease and type 1 diabetes).
-
Genetic predisposition: Family history increases risk; multiple genes likely contribute small effects.
-
Oxidative stress and melanocyte vulnerability: Local biochemical changes can trigger melanocyte damage.
-
Neurogenic factors: Nerve-related signals may influence pigment loss in specific patterns.
-
Environmental triggers: Skin trauma (Koebner phenomenon), sunburn, chemical exposure, or stress can precipitate new patches in a predisposed person.
Knowing what causes vitiligo helps skin specialists create the appropriate treatment plan and suggest the best possible lifestyle changes for a better standard of living.
How is Vitiligo Diagnosed?
Diagnosis is usually clinical, based on visible white spots on skin and history. Key steps include:
-
Clinical inspection in good light; Wood’s lamp examination can reveal subclinical lesions.
-
Medical history to check for autoimmune disease, recent triggers, and family history.
-
Skin biopsy is rarely needed, but it can confirm loss of melanocytes when the diagnosis is uncertain.
-
Blood tests to screen for associated autoimmune conditions (thyroid function tests, blood glucose levels) when indicated.
First-line Medical Treatments
Early, limited vitiligo often responds best to topical measures.
-
Topical corticosteroids for vitiligo (e.g., mid- to high-potency steroids) reduce local immune activity and can repigment small areas if used appropriately and for limited periods to avoid skin thinning.
-
Topical calcineurin inhibitors (tacrolimus and pimecrolimus) are alternatives for the face and sensitive areas; they modulate immune response without steroid-related skin atrophy.
-
Combination strategies (topical plus targeted phototherapy) increase success rates.
Light-based Therapies
Phototherapy for vitiligo uses controlled ultraviolet light to stimulate melanocyte function and reduce immune attack.
-
Narrowband UVB (NB-UVB) is the most widely used and effective form for widespread vitiligo. It requires multiple sessions (typically 2–3 times weekly) and gradual improvement over months.
-
An excimer laser offers targeted high-intensity UV for small, stubborn patches.
-
Phototherapy works best when disease activity is controlled. You can combine phototherapy with topical agents to improve repigmentation rates.
Systemic and Advanced Medical Options
For rapidly progressive or extensive disease:
-
Oral corticosteroids (short courses) may stabilise rapidly spreading vitiligo.
-
Immunomodulators and biologic therapies are under study and may be options in specialist settings for refractory cases.
-
Janus kinase (JAK) inhibitors have shown promise in clinical trials and in selected clinical use when combined with phototherapy, but access and long-term safety monitoring are considerations.
Surgical Repigmentation
When patches are stable for at least 6–12 months, and medical therapy fails, surgical repigmentation can be considered.
-
Techniques include autologous skin grafting, mini-punch grafting, and cell suspension grafting.
-
Surgery transfers pigment-producing cells to depigmented areas to restore colour.
-
Expectations must be realistic: success depends on site, skin type, and disease stability; not all patches are suitable.
Surgical options provide durable results for selected patients and are part of comprehensive vitiligo treatment pathways.
When to Seek Specialist Care?
Refer to dermatology or a specialist centre when:
-
Patches are rapidly spreading.
-
Initial treatments fail after an appropriate trial.
-
Large cosmetic areas of the face and hands are involved.
-
Associated autoimmune conditions or unusual features raise concern.
Specialist teams offer a full range of vitiligo treatment options, access to phototherapy units, and surgical repigmentation expertise.
Conclusion
Timely assessment and a tailored vitiligo treatment plan reduce uncertainty and improve outcomes. Combining topical therapies, phototherapy for vitiligo, lifestyle measures, and psychological support gives the best chance of meaningful repigmentation and improved well-being.
For assessment and a full range of treatment options, consult our top dermatologists at Manipal Hospital Kanakapura Road.
FAQ's
No. Vitiligo is not infectious. It cannot spread between people, though it can progress within the same person.
Topical steroids or calcineurin inhibitors may show improvement in weeks, but meaningful repigmentation often takes several months. Combining topical therapy with phototherapy for vitiligo speeds results for many people.
Patches are painless and do not cause physical illness, but affected skin is more prone to sunburn, and the condition can affect mental health.
No guaranteed cure exists, but many vitiligo treatment options restore pigment and control progression. Surgical repigmentation offers durable results for stable patches.
Choice depends on patch size, disease activity, location, skin type, and personal preference. Start with topical and phototherapy for active or widespread disease; consider surgical repigmentation for stable, limited patches.





















 8 Min Read
8 Min Read