Living with a chronic condition like Ulcerative Colitis can be challenging. A form of Inflammatory Bowel Disease (IBD), this condition affects millions worldwide, often causing significant discomfort and impacting daily life. This blog is a comprehensive guide aiming to shed light on ulcerative colitis, its symptoms, underlying causes, and the effective treatment options available today.
Synopsis
Understanding Ulcerative Colitis
Before looking for treatments for ulcerative colitis, it is important to understand the condition. Ulcerative colitis is a chronic inflammatory disease that primarily affects the large intestine (colon) and rectum. It occurs when the immune system mistakenly attacks the lining of the colon, leading to inflammation and sores called ulcers.
This inflammation can cause a range of debilitating symptoms, varying in severity from person to person.
Despite being a problem that affects a large number of people worldwide, proper management can help individuals lead an active and fulfilling life.
What Causes Ulcerative Colitis?
While the singular cause of ulcerative colitis remains unknown, research suggests it is a complex interplay of several factors:
-
Immune System Dysfunction: Here, the immune system reacts against normal bacteria in the digestive tract, leading to chronic inflammation.
-
Genetics: A family history of ulcerative colitis increases one's risk, indicating a genetic predisposition.
-
Environmental Factors: Diet, stress, and certain medications may be triggering or exacerbating symptoms in genetically susceptible individuals, though they are not direct causes.
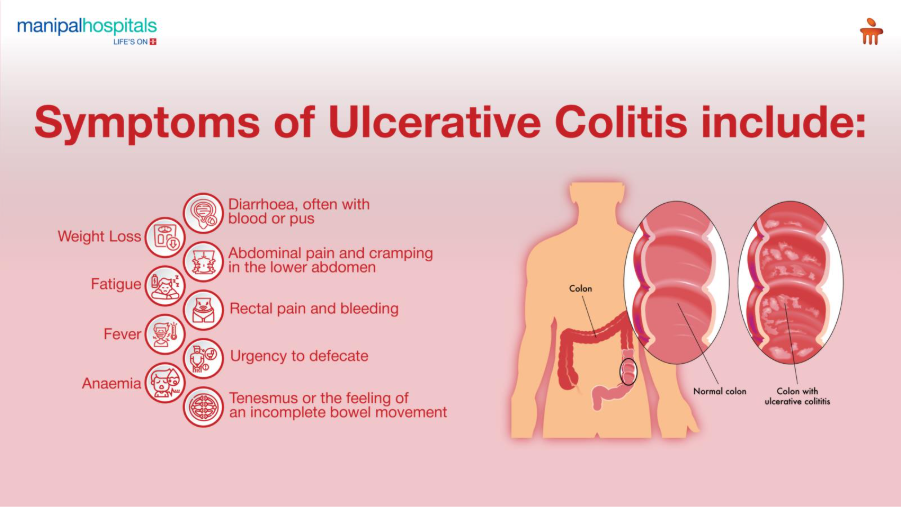
Ulcerative Colitis Symptoms
Ulcerative colitis symptoms often develop gradually and can range from mild to severe. Some of the most common symptoms include:
-
Diarrhoea: Often with blood or pus.
-
Abdominal Pain and Cramping: Usually felt in the lower abdomen.
-
Rectal Pain: Discomfort or pain in the rectum.
-
Rectal Bleeding: Passing small amounts of blood with stool.
-
Urgency to Defecate: A strong, sudden need to use the bathroom.
-
Tenesmus: The feeling of an incomplete bowel movement.
-
Weight Loss: Unexplained weight loss, often due to malabsorption of nutrients or loss of appetite.
-
Fatigue: Persistent tiredness even with minimal activity.
-
Fever: Indicating inflammation or infection.
-
Anaemia: Due to chronic blood loss.
Diagnosing Ulcerative Colitis
Diagnosing ulcerative colitis typically involves a combination of tests:
-
Physical Exam and Medical History: Your doctor will ask about your symptoms and family history.
-
Blood Tests: To check for anaemia, inflammation, and other indicators.
-
Stool Sample Analysis: To rule out infections and identify markers of inflammation.
-
Colonoscopy with Biopsy: This is the most definitive diagnostic tool. A thin, flexible tube with a camera is inserted into the rectum to examine the entire colon, and tissue samples (biopsies) are taken for microscopic analysis.
Ulcerative Colitis Treatment
Thanks to the advancement in modern medicine, ulcerative colitis treatment has effectively helped patients in reducing inflammation, relieve symptoms, induce and maintain remission, and improve overall quality of life.
Medical Management
Medications are the cornerstone of ulcerative colitis treatment and often involve a step-up approach:
-
Anti-inflammatory Drugs: These are often the first line of treatment for mild to moderate ulcerative colitis, helping to reduce inflammation in the colon lining.
-
Immune System Suppressors: For moderate to severe cases, these medications reduce the immune response that triggers inflammation.
-
Biologic Therapies: These advanced treatments target specific proteins in the immune system involved in the inflammatory process. They have revolutionized ulcerative colitis treatment.
Studies have shown that up to 70-80% of patients achieve significant clinical response and remission with these therapies.
Lifestyle and Dietary Considerations
While diet is not a cause behind ulcerative colitis, certain foods can trigger or worsen symptoms. Thus, it is important to identify and avoid trigger foods. Stress management techniques, regular exercise, and avoiding smoking are also crucial for managing symptoms and improving well-being.
Ulcerative Colitis Surgery
While medical therapy is usually the most common type of treatment, for some patients, it might be ineffective. In those cases, ulcerative colitis surgery is typically considered. Surgery is considered when:
-
Medical treatments are ineffective (refractory ulcerative colitis).
-
There are severe complications like toxic megacolon, severe bleeding, or perforation.
-
There's a high risk of colon cancer due to long-standing, extensive ulcerative colitis.
The most common surgical procedure is a total colectomy, which involves removing the entire colon and rectum. Often, this is followed by an ileal pouch-anal anastomosis (IPAA), also known as a J-pouch surgery. This procedure constructs an internal pouch from the small intestine, allowing for a more natural bowel function, with many patients reporting a significant improvement in their quality of life post-surgery.
Care Essentials: Do's and Don'ts
Do's
-
Do follow your medication regimen strictly: Consistency is vital for managing inflammation and preventing flare-ups.
-
Do communicate openly with your healthcare team: Report any new or worsening symptoms, side effects, or concerns.
-
Do maintain a balanced, nutrient-rich diet: Work with a dietician specialising in IBD management to identify trigger foods and ensure adequate nutrition.
-
Do manage stress effectively: Practices like yoga, meditation, or spending time in nature can help.
-
Do stay hydrated: Chronic diarrhoea due to ulcerative colitis can cause dehydration. Drink enough fluids to stay hydrated.
Don'ts
-
Don't skip or alter your medication dosage: This can lead to flare-ups or reduce treatment effectiveness.
-
Don't ignore symptoms: New or worsening symptoms require prompt medical attention.
-
Don't self-medicate: Always consult your doctor before taking any new over-the-counter medications or supplements.
-
Don't smoke: Smoking is a known risk factor for IBD and can worsen symptoms.
-
Don't hesitate to seek emotional support: Living with ulcerative colitis can be challenging; support groups or therapy can be beneficial.
Conclusion
Early diagnosis and timely intervention can significantly improve outcomes and prevent potential complications. At Manipal Hospitals, we believe in empowering our patients with knowledge and provide compassionate, state-of-the-art care. If you are experiencing symptoms suggestive of ulcerative colitis or have been recently diagnosed, it is crucial to seek expert medical advice. Book an appointment with our expert at Manipal Hospitals today for a comprehensive evaluation and personalized treatment plan.
FAQ's
Ulcerative colitis is a chronic condition, and it currently has no medical cure. However, some effective treatment options have helped many individuals achieve long-term remission, where symptoms are absent or minimal, allowing them to lead full, productive lives. Surgery can "cure" the disease by removing the affected colon, but it is a major intervention.
While there is so particular diet to be followed for ulcerative colitis, some foods can trigger or worsen symptoms. Spicy foods, high-fiber foods during flares, dairy products, fatty foods, and caffeine are some such foods.
Extensive ulcerative colitis increases the risk of colon cancer. Regular surveillance colonoscopies are recommended for patients with ulcerative colitis to detect and remove precancerous changes early, significantly reducing this risk.
While not purely hereditary, family history or genetic predisposition of ulcerative colitis can increase risk in individuals.
Both are forms of Inflammatory Bowel Disease (IBD). Ulcerative colitis affects only the large intestine and rectum, causing continuous inflammation of the innermost lining. Crohn's disease can affect any part of the digestive tract, from mouth to anus, and can involve all layers of the bowel wall, with inflamed and healthy areas often interspersed (skip lesions).
With proper diagnosis, consistent medical management, and lifestyle adjustments, the vast majority of individuals with ulcerative colitis can achieve remission and lead normal, active, and fulfilling lives.






















 6 Min Read
6 Min Read